Vascular Pathology — MCQs

On this page
A 22-year-old biker sustained a severe injury in a road traffic accident. After admission to the hospital, his condition suddenly worsened, leading to death. A pathological specimen was provided. What is the likely cause of death?
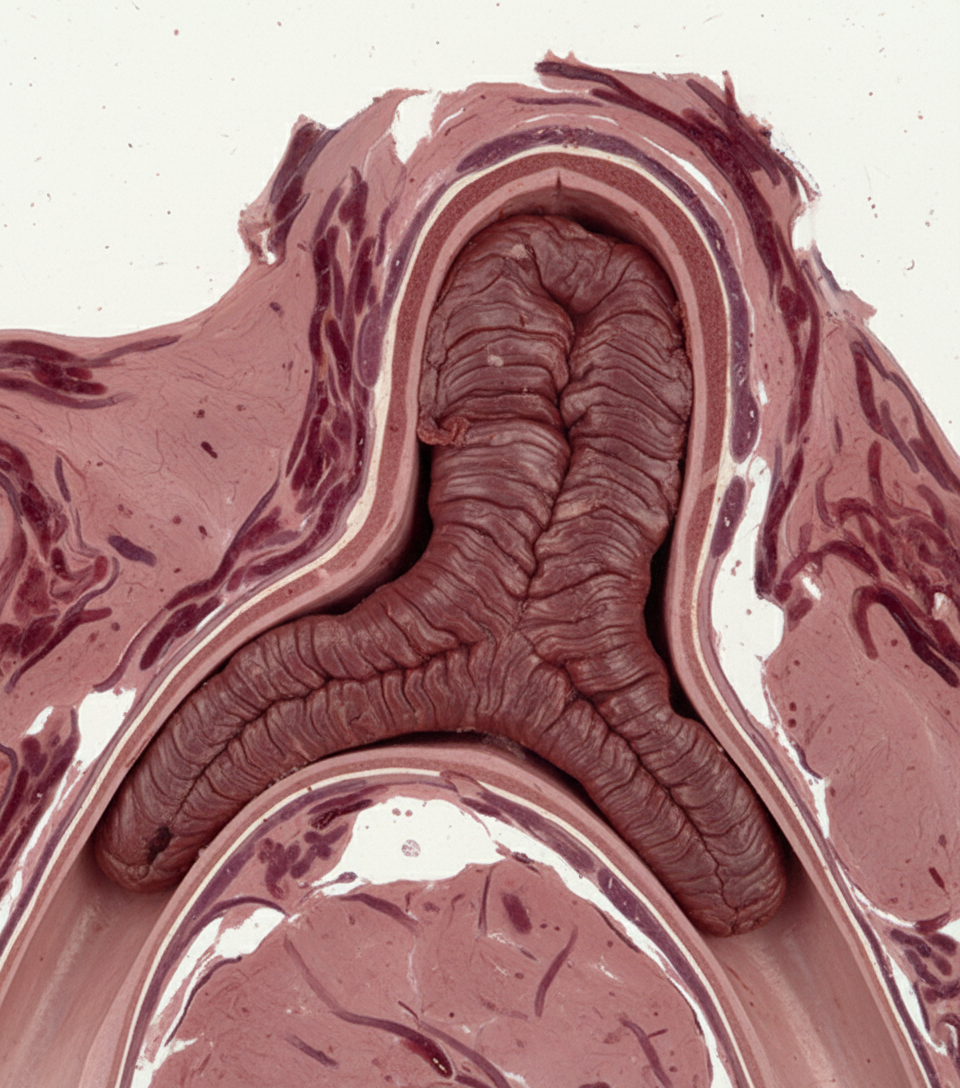
The Virchow triad includes all of the following except:
All of the following are true about pulmonary embolism except:
Lymphangiosarcoma most commonly occurs in the setting of which condition?
Which of the following shows a pumping action?
Mönckenberg's sclerosis involves which layer of the artery?
Which vasculitis is not commonly seen in adults?
Kaposi sarcoma arises from which type of tissue?
An embolus which passes through an arteriovenous communication and enters the systemic circulation is called?
What is the most common site of thrombosis?
Practice by Chapter
Atherosclerosis
Practice Questions
Hypertensive Vascular Disease
Practice Questions
Aneurysms and Dissection
Practice Questions
Vasculitis
Practice Questions
Venous Disease and Thrombosis
Practice Questions
Vascular Tumors
Practice Questions
Varicose Veins and Lymphatics
Practice Questions
Pathology of Vascular Interventions
Practice Questions
Vascular Diseases in Specific Organs
Practice Questions
Congenital Vascular Anomalies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
