Vascular Pathology — MCQs

On this page
A 25-year-old female underwent septic abortion. What is the most likely site for embolism of tricuspid valve vegetation?
Which of the following arteries is most likely to be involved with serious atherosclerosis?
Churg-Strauss syndrome involves which of the following, except?
Which of the following conditions are classified as small vessel vasculitis?
Deficiency of which of the following factors increases the incidence of thrombus formation?
Which of the following statements is NOT true regarding hypersensitivity vasculitis?
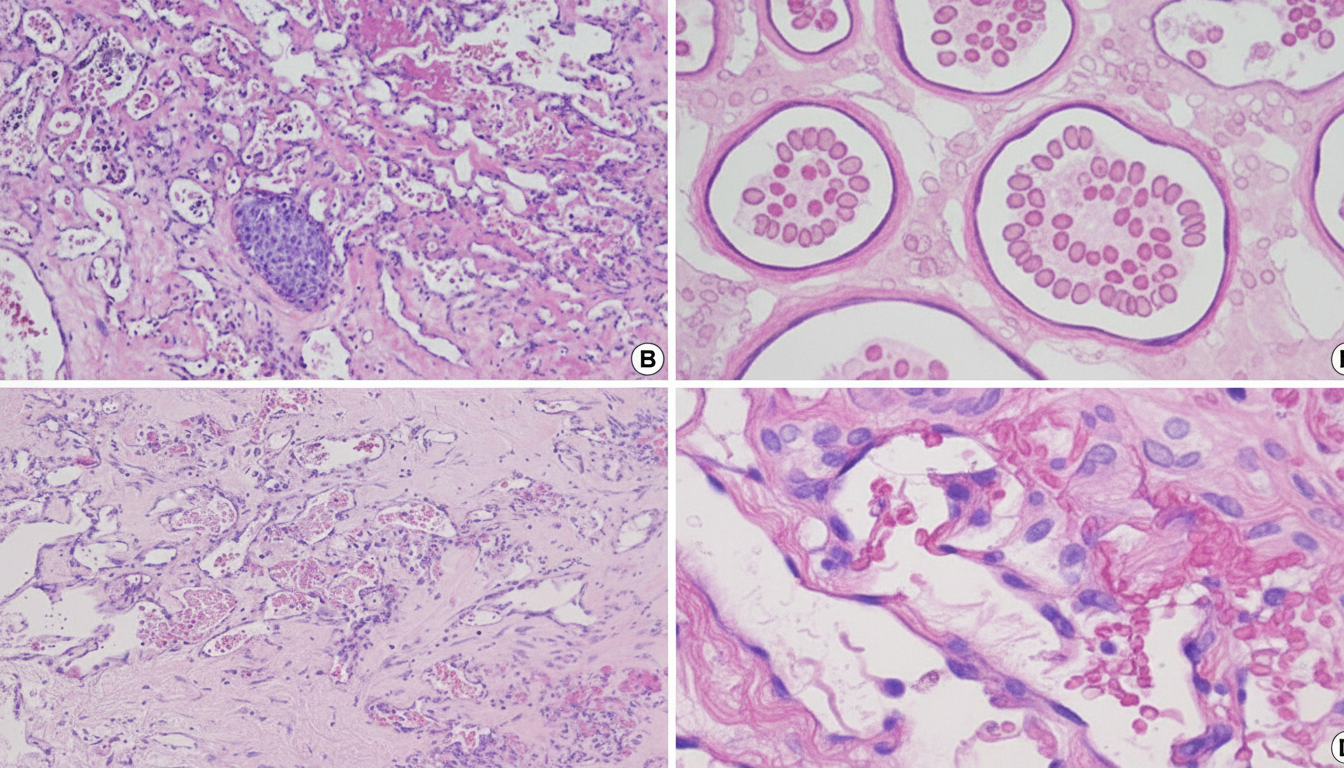
A 20-year-old patient presents with a soft to firm reddish swelling progressing in size over the precordium. Histopathological examination showed findings consistent with this lesion. What is the most likely diagnosis?
What is the most common site of acute aortic dissection?
What is an important feature in Henoch-Schönlein purpura?
Neointimal hyperplasia causes vascular graft failure as a result of hypertrophy of -
Practice by Chapter
Atherosclerosis
Practice Questions
Hypertensive Vascular Disease
Practice Questions
Aneurysms and Dissection
Practice Questions
Vasculitis
Practice Questions
Venous Disease and Thrombosis
Practice Questions
Vascular Tumors
Practice Questions
Varicose Veins and Lymphatics
Practice Questions
Pathology of Vascular Interventions
Practice Questions
Vascular Diseases in Specific Organs
Practice Questions
Congenital Vascular Anomalies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
