Respiratory Pathology — MCQs

On this page
Bilateral malignant pleural effusion is most often seen in which of the following conditions?
On biopsy, a characteristic finding of malignant mesothelioma is:
Collar button lesions are characteristic of which of the following conditions?
All of the following statements about Emphysema are true, except:
What is true about Alpha-1 antitrypsin deficiency?
A 56-year-old man with a history of cigarette smoking presents with difficulty swallowing and a muffled voice. Laryngoscopy reveals a 2-cm laryngeal mass. If this mass is a malignant neoplasm, which of the following is the most likely histologic diagnosis?
Smoking is generally not associated as a risk factor with which of the following?
Carcinoid tumors of the lung arise from which of the following cells?
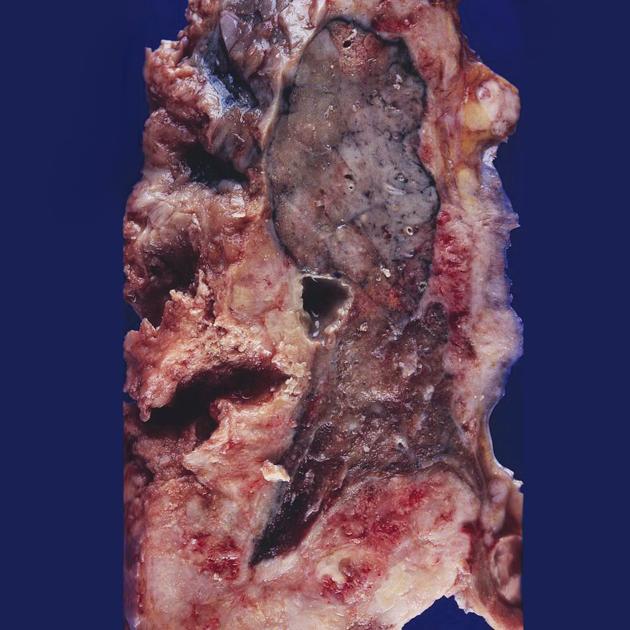
A 40-year-old female presented with a 3-month history of fever, loss of appetite, weight loss, cough, and weakness. A chest X-ray revealed consolidation in the upper lung. She died a few days after admission. Autopsy revealed gross lung findings and biopsy findings. What is your diagnosis?
Caplan syndrome is seen in which of the following conditions?
Practice by Chapter
Congenital Anomalies
Practice Questions
Atelectasis and Acute Lung Injury
Practice Questions
Obstructive Pulmonary Diseases
Practice Questions
Restrictive Pulmonary Diseases
Practice Questions
Lung Infections
Practice Questions
Pulmonary Vascular Diseases
Practice Questions
Lung Tumors
Practice Questions
Pleural Diseases
Practice Questions
Interstitial Lung Diseases
Practice Questions
Occupational Lung Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
