Reproductive Pathology — MCQs

On this page
What is the most common primary tumor to cause a Krukenberg tumor?
Which of the following markers is NOT typically elevated in a testicular teratoma?
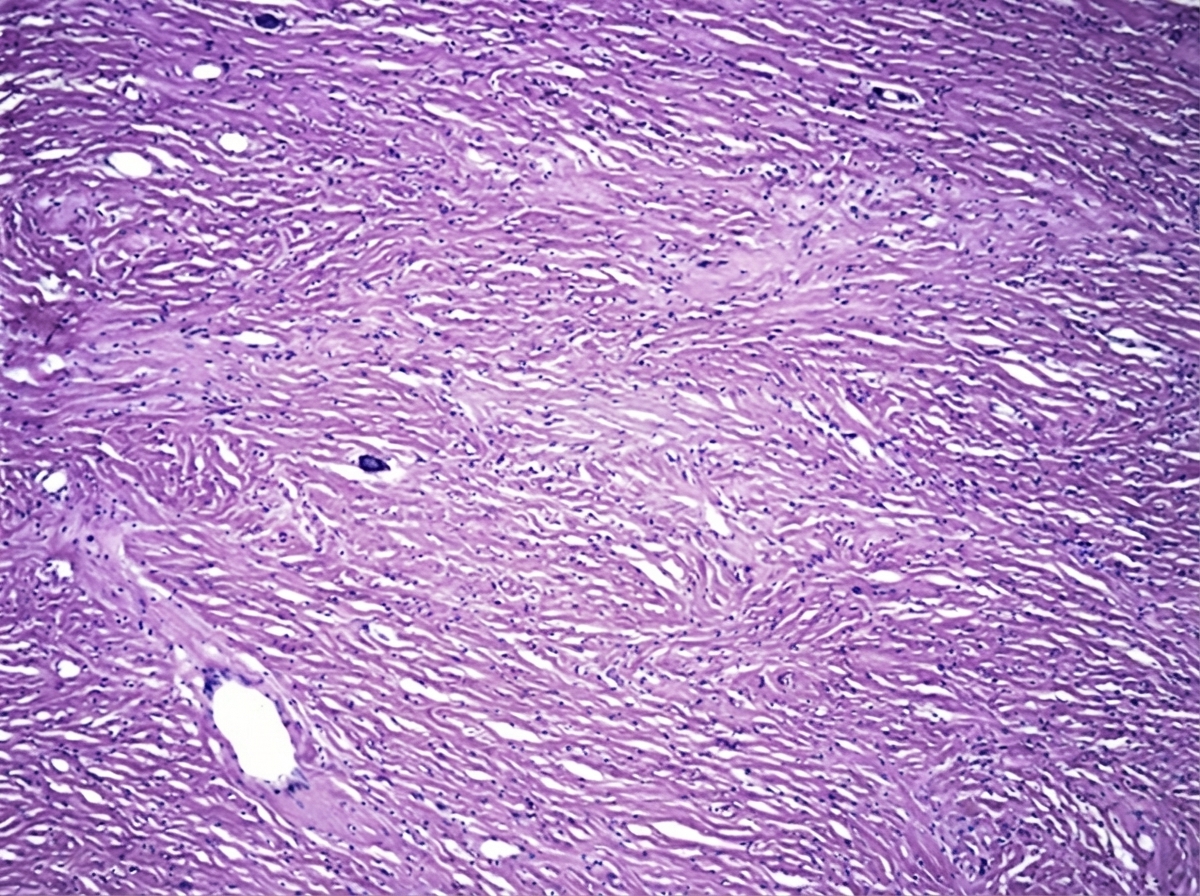
A 35-year-old female underwent hysterectomy, which revealed specific gross and histological features. What is the most likely diagnosis?
Schiller-Duval bodies are seen in which of the following tumor types?
Which of the following benign breast lesions is associated with a moderately increased risk of invasive breast carcinoma?
All changes occur in a fibroid uterus. Except?
What is the histological type of cervical cancer that is most sensitive to radiotherapy?
How does seminoma typically spread?
A 30-year-old patient presents with testicular hypoechoic mass and back pain. Which tumor marker is most appropriate?
Seminoma is carcinoma of:
Practice by Chapter
Diseases of Male Genital Tract
Practice Questions
Testicular Tumors
Practice Questions
Prostate Pathology
Practice Questions
Diseases of Female Genital Tract
Practice Questions
Cervical Pathology and Neoplasia
Practice Questions
Endometrial Pathology
Practice Questions
Ovarian Diseases and Tumors
Practice Questions
Gestational Trophoblastic Disease
Practice Questions
Placental Pathology
Practice Questions
Sexually Transmitted Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
