Reproductive Pathology — MCQs

On this page
Which of the following statements about benign prostatic hyperplasia (BPH) is true?
A 23-year-old male presents with a testicular mass. A biopsy shows a mixture of syncytiotrophoblasts and cytotrophoblasts. Which tumor marker is likely to be elevated?
A 40-year-old man presents with a painless testicular mass. Laboratory results show high AFP and high hCG levels. Biopsy reveals sheets of large anaplastic cells with abundant cytoplasm. What is the likely diagnosis?
Identify the condition represented in the image of a testicular tumor.
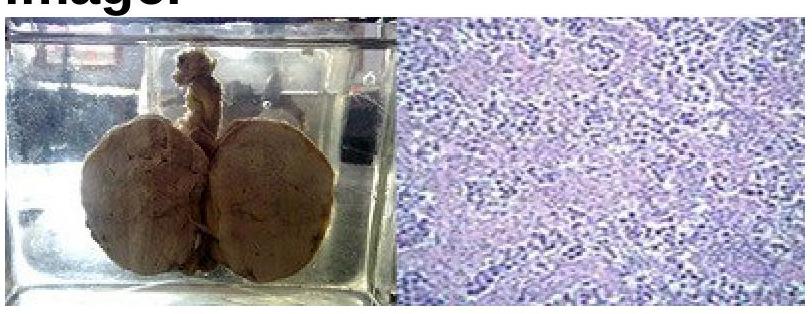
Which karyotype is most commonly associated with true hermaphroditism?
Dysgerminoma spreads mainly via ?
In Grade 1 endometrial cancer, what is the percentage of solid growth pattern typically observed?
What is the approximate percentage of cases in which simple hyperplasia with atypia progresses to endometrial cancer?
In a case of Dysgerminoma of ovary one of the following tumor markers is likely to be raised :
In the context of Endometrial carcinoma, which tumor suppressor gene is most commonly mutated?
Practice by Chapter
Diseases of Male Genital Tract
Practice Questions
Testicular Tumors
Practice Questions
Prostate Pathology
Practice Questions
Diseases of Female Genital Tract
Practice Questions
Cervical Pathology and Neoplasia
Practice Questions
Endometrial Pathology
Practice Questions
Ovarian Diseases and Tumors
Practice Questions
Gestational Trophoblastic Disease
Practice Questions
Placental Pathology
Practice Questions
Sexually Transmitted Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
