Reproductive Pathology — MCQs

On this page
A 30-year-old female presents to the OPD with a 3 cm breast lump in the upper medial quadrant. The lump has an uneven, bosselated surface, and the overlying skin is mildly ulcerated. Microscopic examination reveals the given findings. What is the most likely diagnosis?
A 50 year old female presented with a breast mass that was operated and the microscopic examination in given. What is the diagnosis?
A biopsy from a breast mass in a 55-year-old woman shows infiltrating ductal carcinoma. Immunohistochemistry reveals ER negative, PR negative, and HER2/neu negative. What is the classification of this tumor?
Histopathological features of granulosa cell tumor include all except:
A 30-year-old man presents with a painless testicular mass. An ultrasound shows a well-circumscribed, homogeneous, non-hemorrhagic testicular tumor. Which of the following is the most likely diagnosis?
A 50-year-old lady developed ascites. CT abdomen showed bilateral ovarian masses which were resected. The histopathological slide from the mass is shown below. What is the diagnosis?
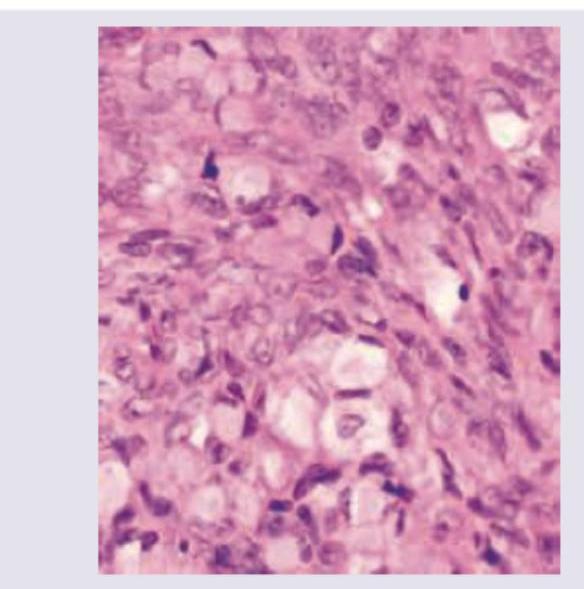
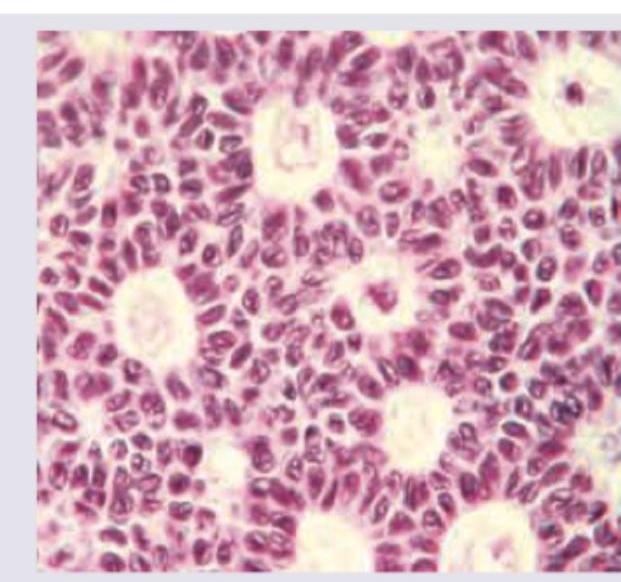
A 6-year-old girl with precocious puberty was found to have an ovarian tumour, which was resected laparoscopically. Histopathological slides were prepared. What is the diagnosis?
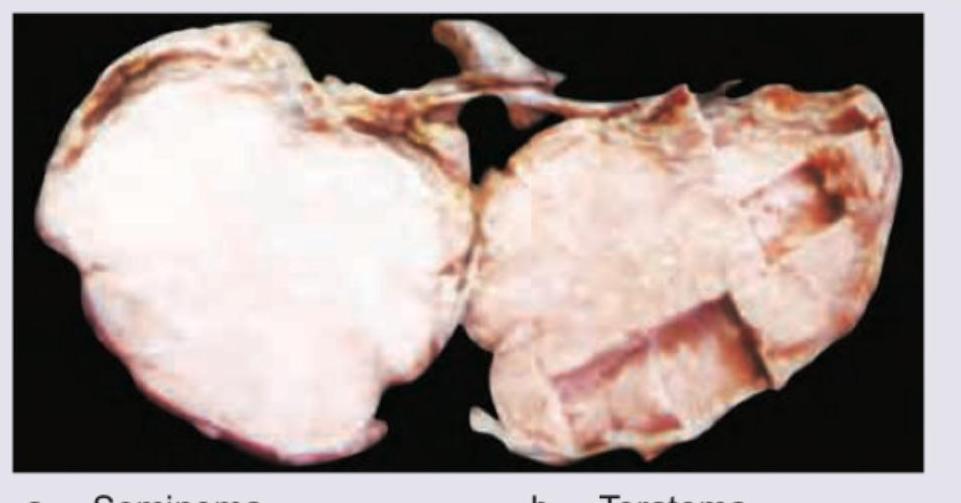
A 24 -year-old male patient with undescended testis has a lump in the groin since birth which was increasing since last 6 months. The resected specimen is shown below. All are correct about the condition except:
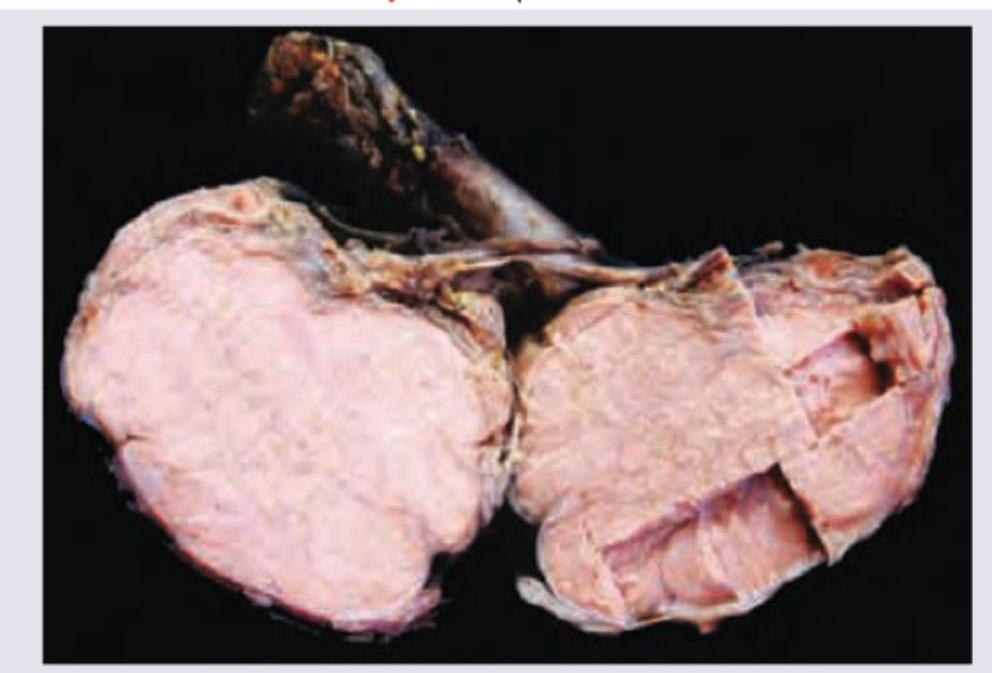
The following is a post-orchidectomy histopathological specimen. Diagnosis is:
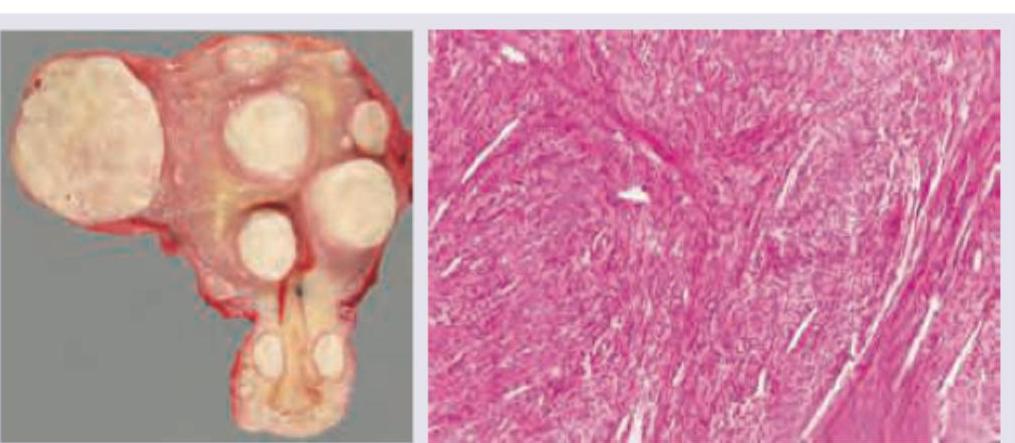
Hysterectomy specimen from a 40-year-old lady is shown along with histology slide. The diagnosis is:
Practice by Chapter
Diseases of Male Genital Tract
Practice Questions
Testicular Tumors
Practice Questions
Prostate Pathology
Practice Questions
Diseases of Female Genital Tract
Practice Questions
Cervical Pathology and Neoplasia
Practice Questions
Endometrial Pathology
Practice Questions
Ovarian Diseases and Tumors
Practice Questions
Gestational Trophoblastic Disease
Practice Questions
Placental Pathology
Practice Questions
Sexually Transmitted Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
