Reproductive Pathology — MCQs

On this page
A patient presents with complaints of sciatica. Radiological examination reveals sclerotic lesions on his skull. Which of the following is most likely to be elevated in this patient?
What is the most common carcinoma of the breast?
Which of the following is NOT a tumor marker for testicular tumors?
Which of the following is the most common type of ovarian tumors?
Corkscrew shaped endometrial glands are seen in which phase of the menstrual cycle?
Which is a specific marker for prostatic cancer?
Reinke crystalloids can be seen in which of the following sex cord-stromal tumors?
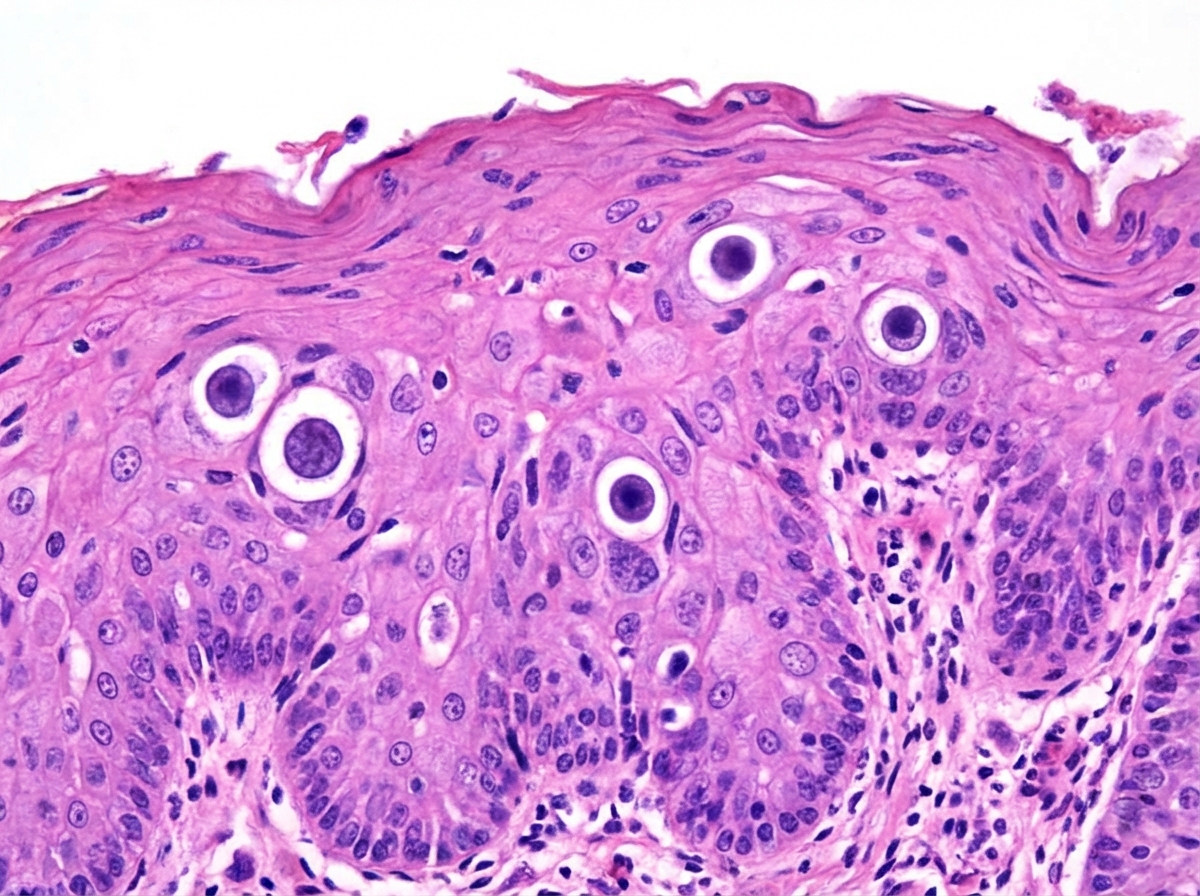
The lesion shown below is caused by:
Type 2 endometrial carcinoma is associated with what histological finding?
Which tumor typically presents with a grape-like cluster appearance and consistency?
Practice by Chapter
Diseases of Male Genital Tract
Practice Questions
Testicular Tumors
Practice Questions
Prostate Pathology
Practice Questions
Diseases of Female Genital Tract
Practice Questions
Cervical Pathology and Neoplasia
Practice Questions
Endometrial Pathology
Practice Questions
Ovarian Diseases and Tumors
Practice Questions
Gestational Trophoblastic Disease
Practice Questions
Placental Pathology
Practice Questions
Sexually Transmitted Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
