Reproductive Pathology — MCQs

On this page
A 72-year-old man presents with a 10-year history of increasing difficulty with urination, characterized by nocturia, urgency with small urine volumes, and hesitancy in starting and stopping micturition. Physical examination reveals an enlarged, non-tender prostate, approximately twice its normal size. His serum prostate-specific antigen (PSA) level was 6 ng/mL one year ago and remains unchanged. Which of the following drugs is most likely to be effective in treating this patient's condition?
Which of the following is an exception for secreting hormones?
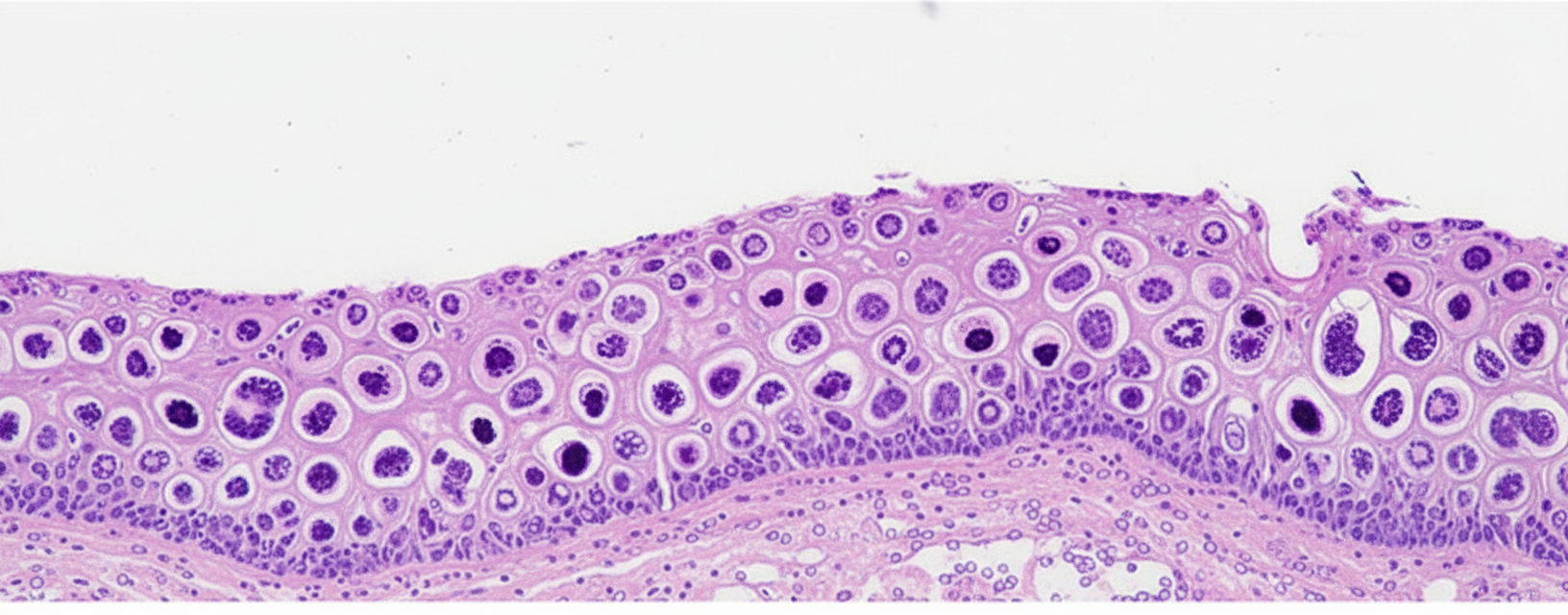
A cervical lesion is shown, which is similar to that obtained in a cone cervical biopsy from a 28-year-old sexually active woman who had had a "positive" Pap smear. What type of cervical change is often characterized by the lesion shown?
A patient presents with an abdominal mass. Investigations reveal bilateral ovarian masses with smooth surfaces. Microscopy shows cells with signet ring shapes. What is the most likely diagnosis?
P57KIP2 immunostaining is helpful in diagnosing which of the following conditions?
Gleason score is used to grade which cancer?
A pathologist is examining placentas from five different patients. He notes the following characteristics in the placentas: Patient A: fused dichorionic diamniotic; Patient B: dichorionic diamniotic; Patient C: circumvallate placenta; Patient D: monochorionic diamniotic. Which of the patients unquestionably gave birth to identical twins?
Which of the following is a marker for testicular tumor?
Which of the following microscopic features is NOT typically seen in seminoma?
HCG is raised in all of the following conditions except:
Practice by Chapter
Diseases of Male Genital Tract
Practice Questions
Testicular Tumors
Practice Questions
Prostate Pathology
Practice Questions
Diseases of Female Genital Tract
Practice Questions
Cervical Pathology and Neoplasia
Practice Questions
Endometrial Pathology
Practice Questions
Ovarian Diseases and Tumors
Practice Questions
Gestational Trophoblastic Disease
Practice Questions
Placental Pathology
Practice Questions
Sexually Transmitted Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
