Trauma to the Central Nervous System — MCQs

Which of the following represents a secondary brain injury mechanism?
Post contusional syndrome includes:
The earliest manifestation of increased intracranial pressure following head injury is:
A 43-year-old man presents to the emergency department after falling down a flight of stairs and landing on his head. He did not lose consciousness. He complains of severe headache, marked decreased acuity in hearing in the left ear, and a "runny nose" since the fall. On physical examination, he is found to have a left-sided Battle's sign (an ecchymosis in the area of the left mastoid process) and hemotympanum. He has a constant dripping of a clear, watery fluid through his nose. Findings on his neurologic examination, other than the hearing loss, are completely normal. X-ray studies will reveal which of the following?
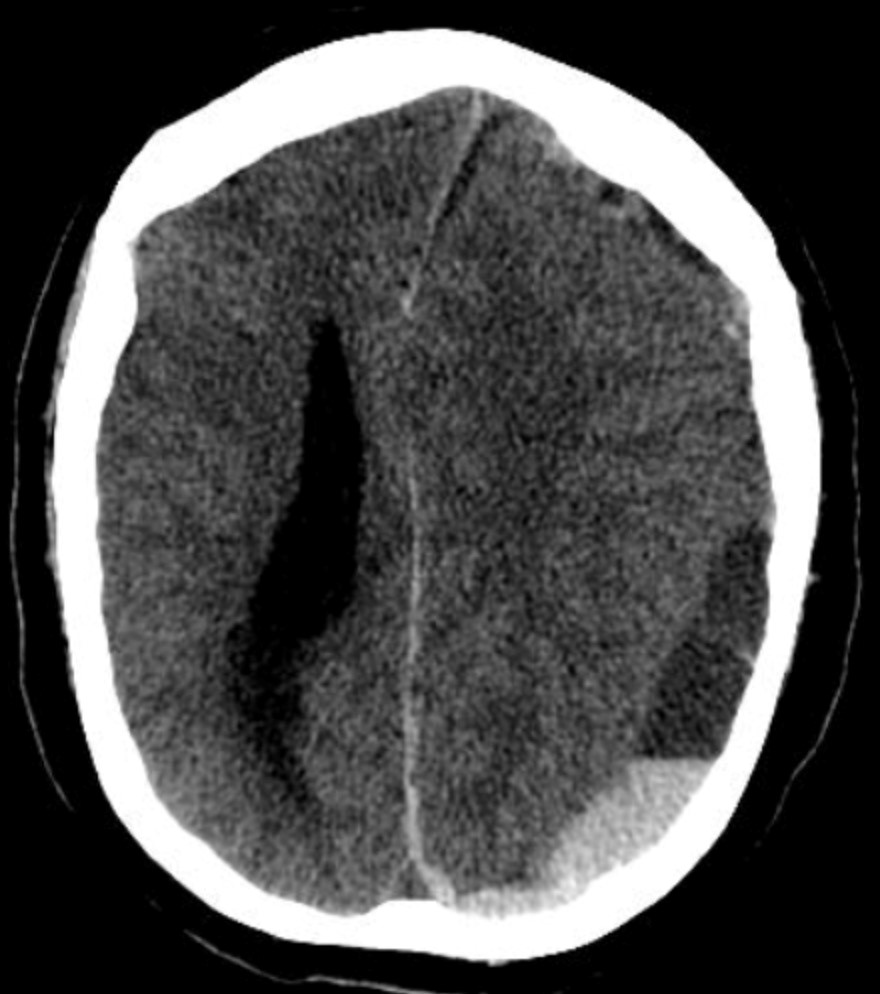
A polytrauma patient's CT brain shows a crescent-shaped extra-axial collection with a concave inner margin. What is the most likely diagnosis?
Glasgow coma scale -moderate includes
What is the primary pathological mechanism in classical Guillain-Barré syndrome affecting the peripheral nervous system?
A child presented with microcephaly, hepatomegaly and periventricular calcification. What is the best specimen for diagnosis of CMV by PCR?
Investigation of choice for leptomeningeal carcinomatosis:
Treatment of Neurocysticercosis includes all of the following except -
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
