Molecular Pathology — MCQs

On this page
Laminin is present in?
Which of the following is a part of secondary granules in neutrophils?
Anticipation is seen in which of the following genetic phenomena?
What is the most common site of liquefactive necrosis?
A 25-year-old man presents with headaches, visual disturbances, and hypertension. MRI brain shows a cerebellar hemangioblastoma, and abdominal imaging reveals multiple cysts in the kidneys along with a solid renal mass suggestive of renal cell carcinoma. His father had similar findings and died from a brain tumor in his 40s. Which of the following chromosomal abnormalities is most likely associated with his condition?
Which of the following is not an aneuploidy?
A 15-year-old tall boy with long limbs presents to the OPD. On ocular examination, bilateral ectopia lentis is noted. Which gene is most likely affected in this inherited disorder?
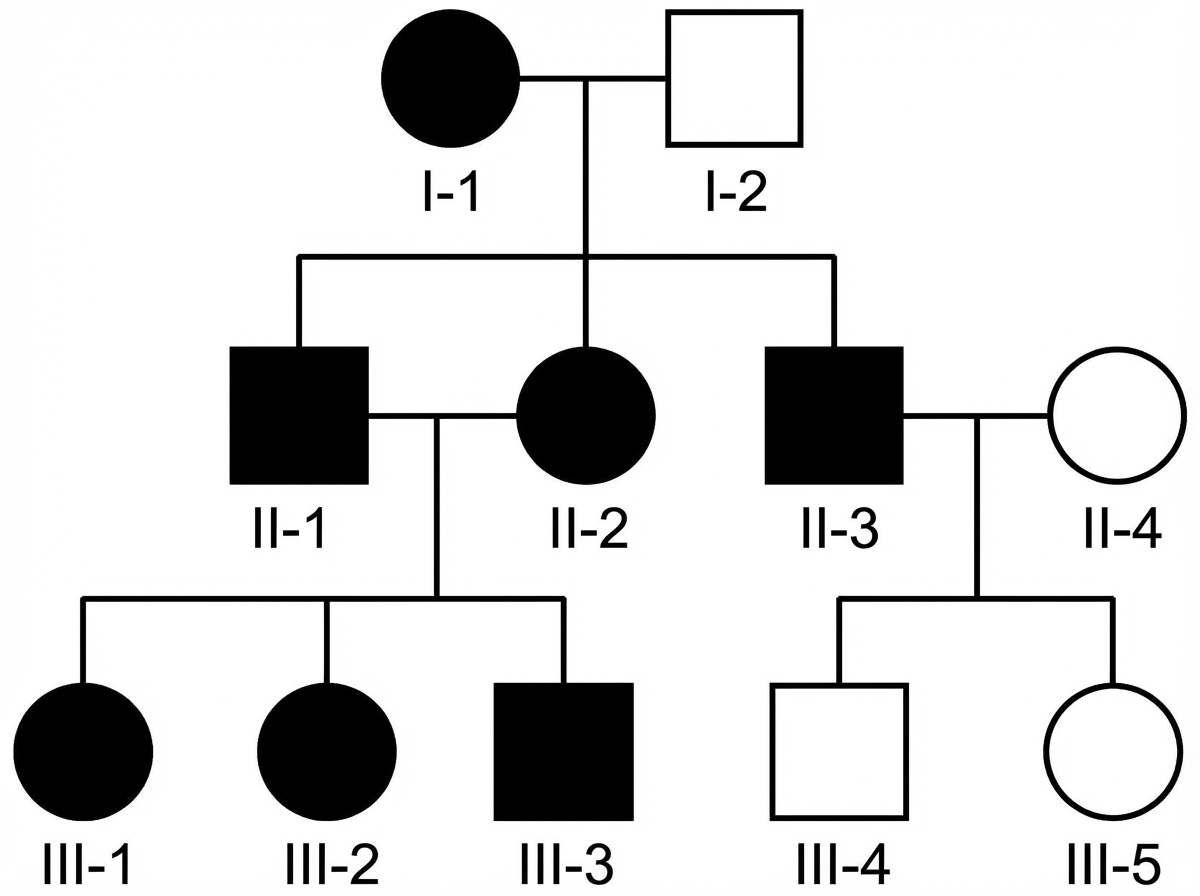
The pedigree chart shown in the image demonstrates a specific pattern of inheritance. Which of the following conditions is most likely to follow this pattern of inheritance?
A 22-year-old tall male presents with long limbs, increased arm span, hypermobile joints, and high-arched palate. On examination, he has lens subluxation and a diastolic murmur suggestive of aortic root dilation. Which of the following genes is most likely mutated in this condition?
Which of the following is an incorrect gene-disease association?
Practice by Chapter
Principles of Molecular Pathology
Practice Questions
DNA and RNA Analysis Techniques
Practice Questions
Cytogenetics
Practice Questions
Polymerase Chain Reaction Applications
Practice Questions
Next-Generation Sequencing
Practice Questions
Molecular Diagnosis of Infectious Diseases
Practice Questions
Molecular Oncology
Practice Questions
Pharmacogenomics
Practice Questions
Genetic Counseling and Risk Assessment
Practice Questions
Molecular Diagnostics Quality Control
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
