Liver and Biliary Pathology — MCQs

On this page
Mallory hyaline is seen in all the following conditions except:
Centrilobular necrosis in the liver is due to which of the following conditions?
Acetaminophen poisoning causes which of the following changes in the liver?
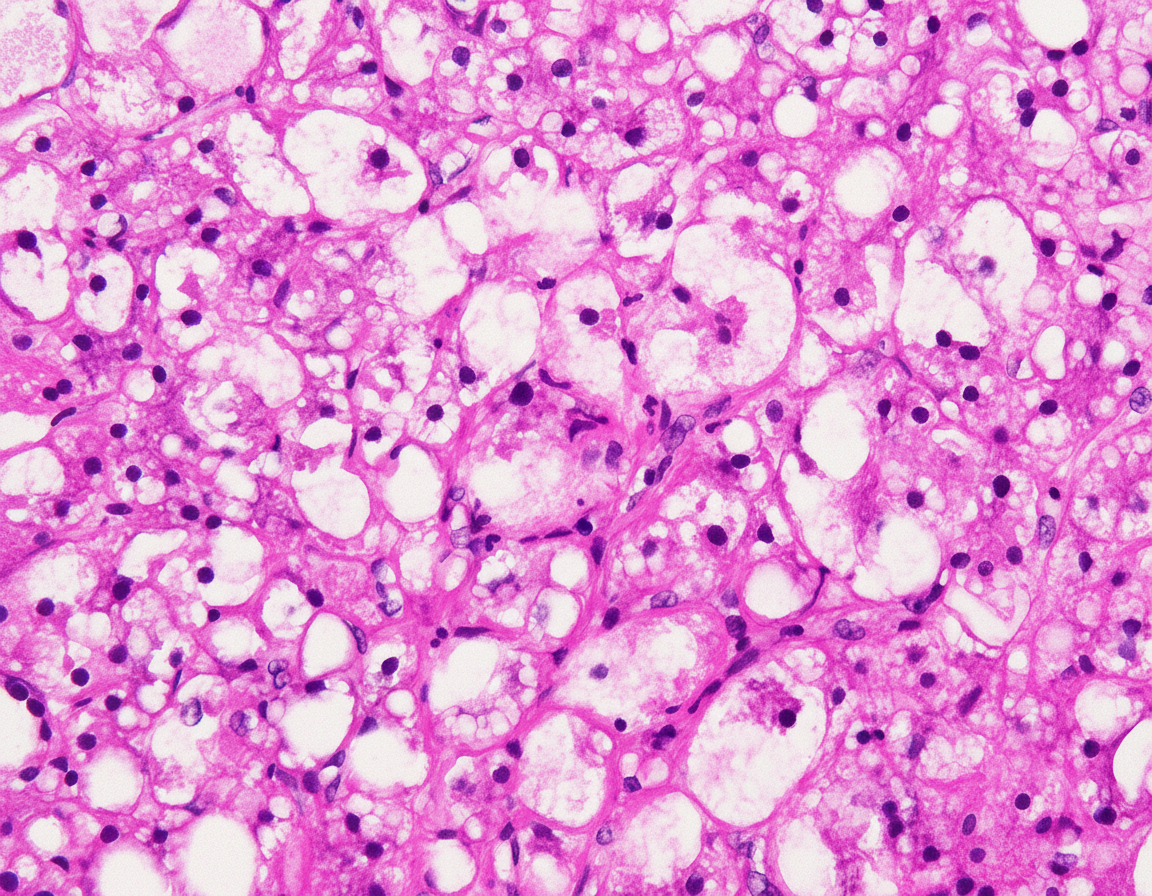
A 45-year-old male with a history of chronic alcoholism presented with pain in the abdomen. Ultrasound suggested fatty liver. A liver biopsy was performed and is shown below. What is your interpretation and likely diagnosis?
Which of the following is the inheritance pattern of Caroli's syndrome?
Strawberry gallbladder is a condition characterized by which of the following findings?
More than 80% of gallstones are composed of which of the following substances?
Which of the following conditions is associated with Hepatitis B?
Centrilobular necrosis of the liver is typically associated with which of the following agents?
Anti-LKM antibodies are a series of autoantibodies directed against enzymes in the endoplasmic reticulum of hepatocytes and other cells that are mainly associated with various liver diseases. Which of the following statements about LKM antibodies is FALSE?
Practice by Chapter
Jaundice and Cholestasis
Practice Questions
Viral Hepatitis
Practice Questions
Alcoholic and Non-alcoholic Fatty Liver Disease
Practice Questions
Drug and Toxin Induced Liver Injury
Practice Questions
Cirrhosis and Its Complications
Practice Questions
Metabolic Liver Diseases
Practice Questions
Liver Tumors
Practice Questions
Gallbladder and Biliary Tract Diseases
Practice Questions
Congenital Liver Diseases
Practice Questions
Liver Transplantation Pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
