Liver and Biliary Pathology — MCQs

On this page
Vinyl chloride exposure is associated with which of the following malignancies?
A 58-year-old male with history of multiple sexual partners presented with anorexia and jaundice. The biopsy shows ground-glass opacity in the cells. What is the most probable diagnosis?
A liver biopsy shows ballooning degeneration of hepatocytes, Mallory-Denk bodies, and neutrophilic infiltration. The patient has a history of chronic alcohol abuse. What is the most likely diagnosis?
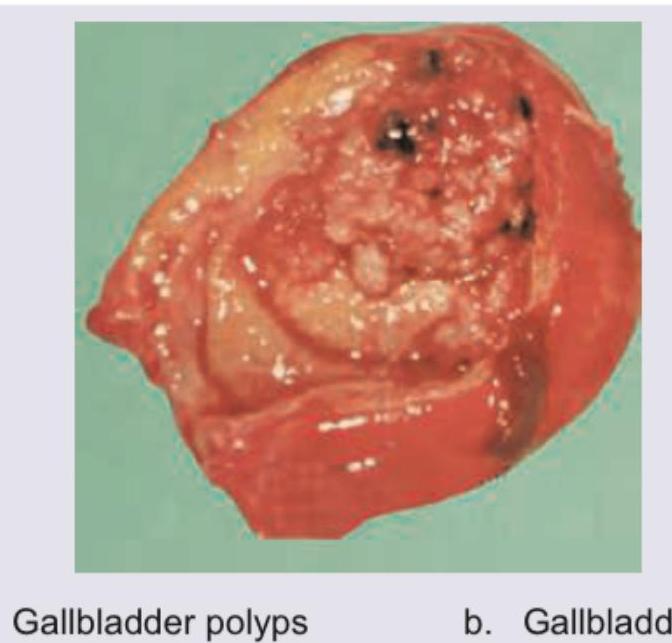
Comment on the diagnosis of the gallbladder specimen provided: (Recent NEET Pattern 2016-17)
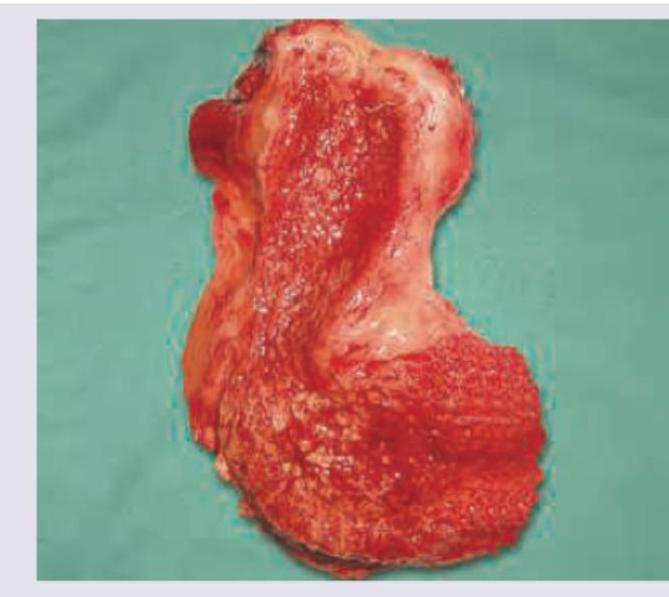
A patient with symptomatic cholecystitis underwent a cholecystectomy. The following specimen was obtained. What is the diagnosis?
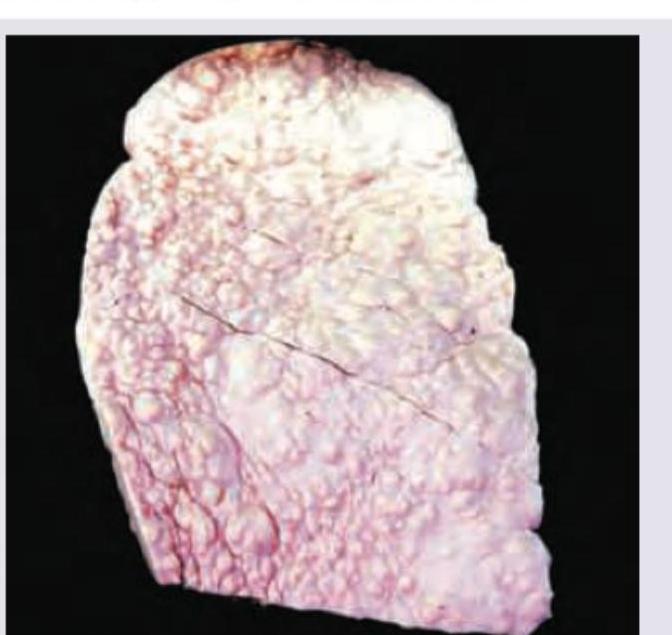
All are true about this liver specimen except:
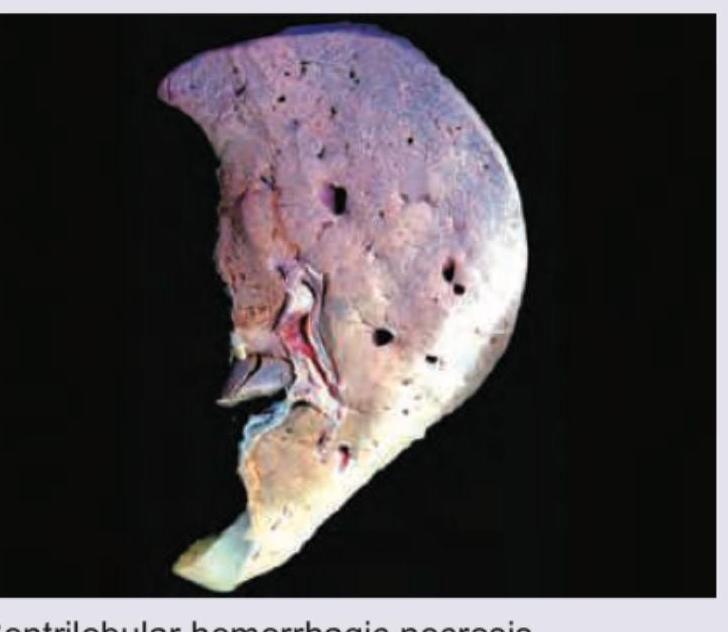
The following liver specimen shows:
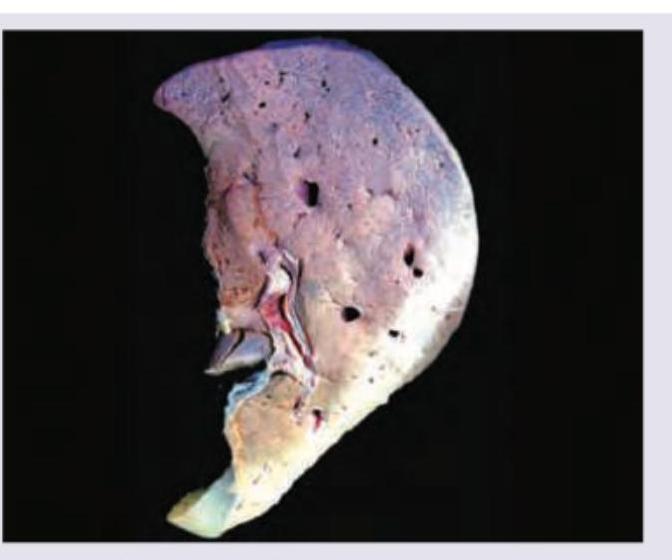
The liver specimen is diagnostic of:
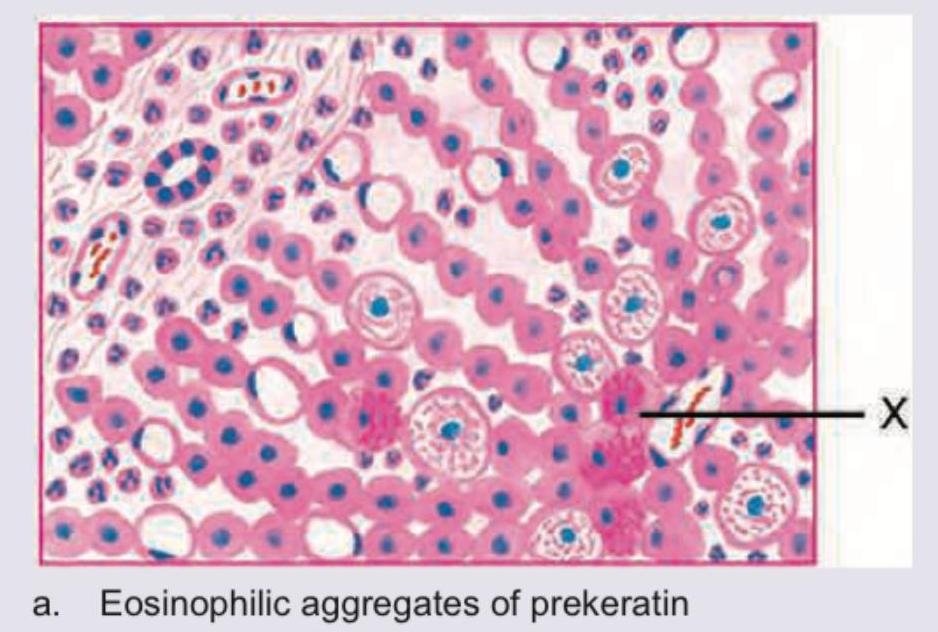
All are true about the marking X in histopathological specimen from a patient of fatty liver except:
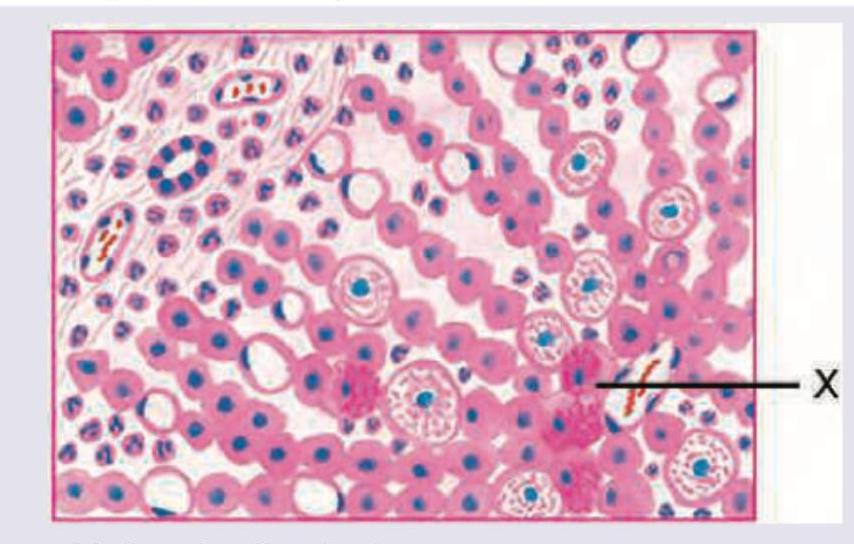
The marking X in a histopathological specimen from a patient of fatty liver shows:
Practice by Chapter
Jaundice and Cholestasis
Practice Questions
Viral Hepatitis
Practice Questions
Alcoholic and Non-alcoholic Fatty Liver Disease
Practice Questions
Drug and Toxin Induced Liver Injury
Practice Questions
Cirrhosis and Its Complications
Practice Questions
Metabolic Liver Diseases
Practice Questions
Liver Tumors
Practice Questions
Gallbladder and Biliary Tract Diseases
Practice Questions
Congenital Liver Diseases
Practice Questions
Liver Transplantation Pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
