Liver and Biliary Pathology — MCQs

On this page
A 44-year-old patient presented with jaundice and had a needle prick injury 2 years back. Based on the provided histological features of a liver biopsy, classify the type of hepatitis.
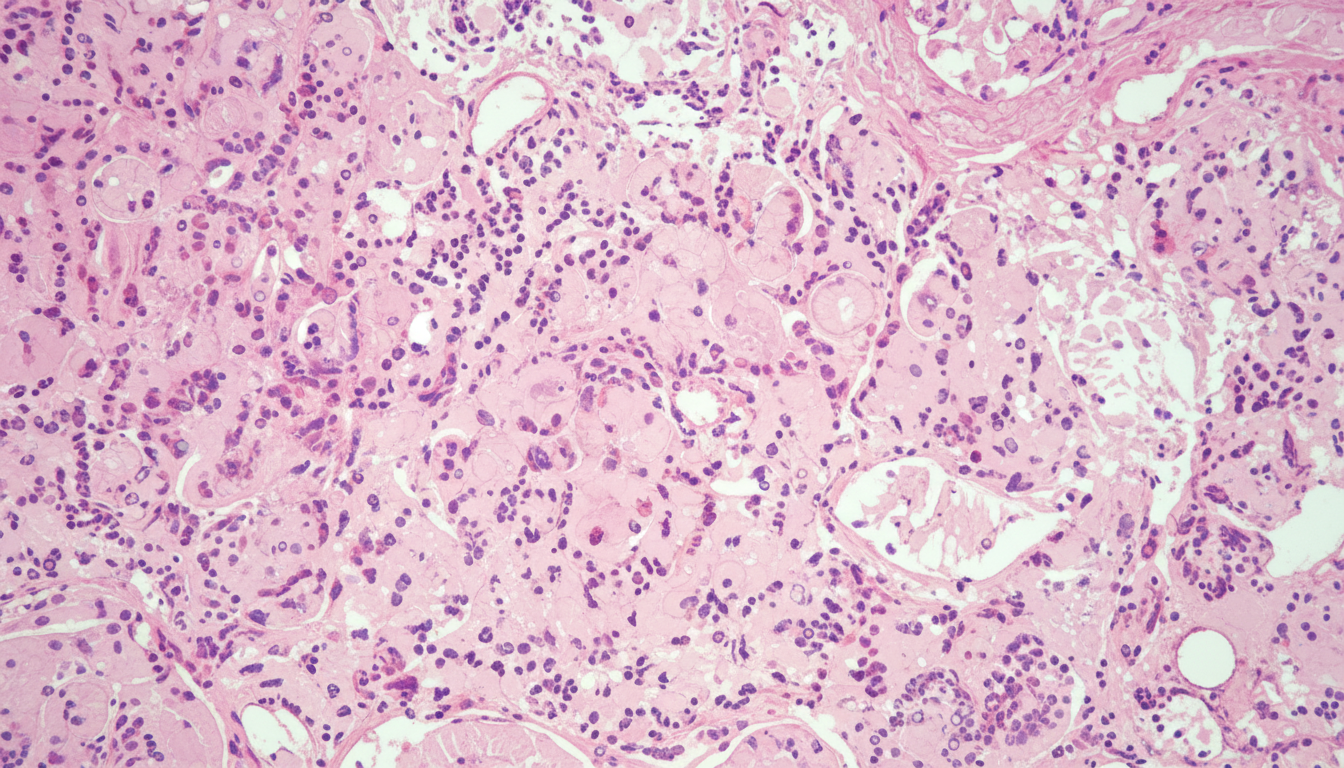
Ballooning of hepatocytes is not associated with which of the following conditions?
Which clinical test is done to assess hepatic function related to bleeding disorders?
OVAL cells are seen in the stem cells of which organ?
A 42-year-old man experiences malaise and increasing icterus for 2 weeks. Physical examination shows jaundice, but there are no other significant findings. Serologic test results are positive for IgM anti-HAV and negative for anti-HCV, HBsAg, and IgM anti-HBc. Which of the following outcomes is most likely to occur in this man?
Bile infarct is related to which of the following conditions?
Ductopenia is a characteristic finding in which of the following conditions?
What is the most common paraneoplastic syndrome associated with hepatocellular carcinoma?
Mallory denk bodies are seen in all of the following conditions except?
Granulomatous hepatitis is not caused by which of the following?
Practice by Chapter
Jaundice and Cholestasis
Practice Questions
Viral Hepatitis
Practice Questions
Alcoholic and Non-alcoholic Fatty Liver Disease
Practice Questions
Drug and Toxin Induced Liver Injury
Practice Questions
Cirrhosis and Its Complications
Practice Questions
Metabolic Liver Diseases
Practice Questions
Liver Tumors
Practice Questions
Gallbladder and Biliary Tract Diseases
Practice Questions
Congenital Liver Diseases
Practice Questions
Liver Transplantation Pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
