Liver and Biliary Pathology — MCQs

On this page
Non-alcoholic steatohepatitis is seen in all, except:
All are features of hepatocellular carcinoma, except?
The hepatotoxic octapeptides of Amanita phalloides usually produce which of the following types of liver injury?
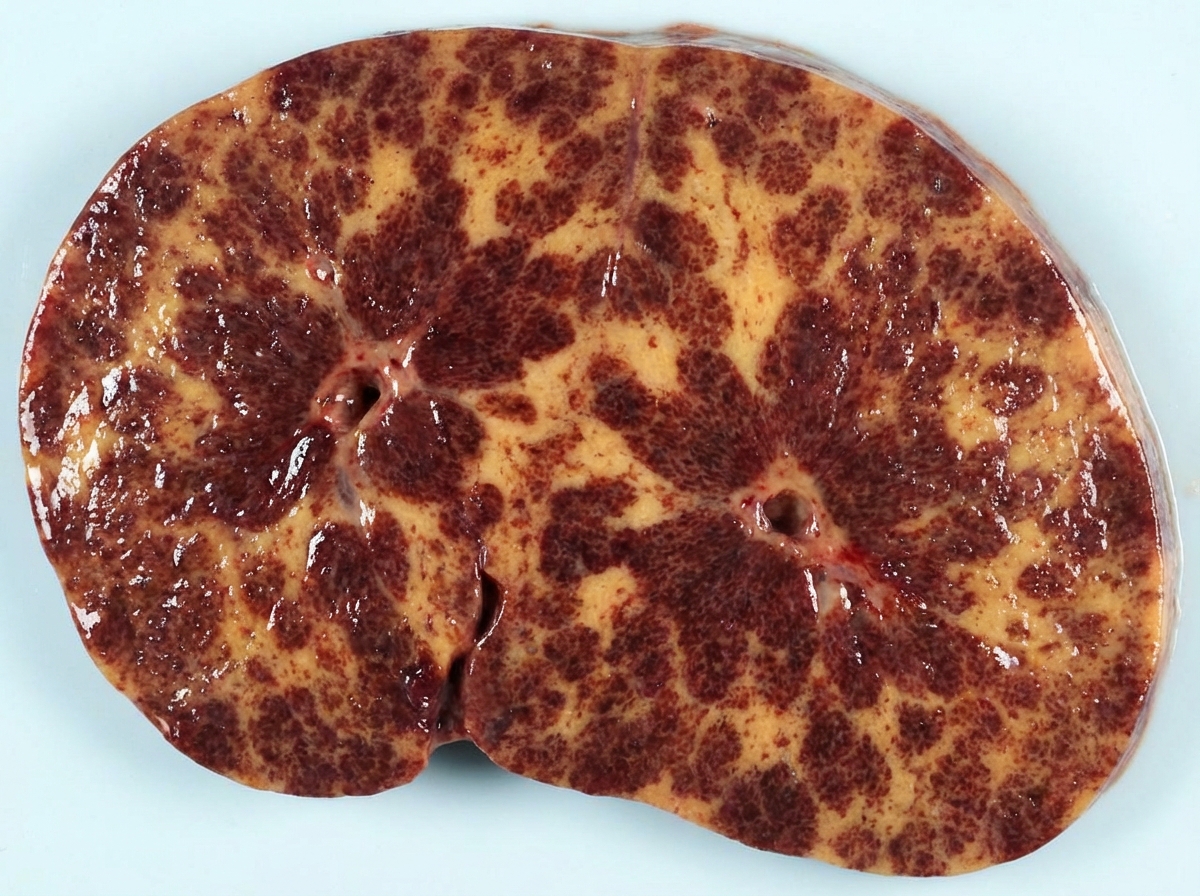
A 40-year-old woman dies after a long history of an illness characterized by dyspnea, orthopnea, hepatomegaly, distended neck veins, and peripheral edema. The cut surface of the liver as it appears at autopsy is shown in the image. Which of the following disorders is the most likely cause of these findings?
A 24-year-old patient presented with unexplained weight loss and fever. Routine examinations showed elevated liver function tests. USG showed a growth in the liver which was confirmed as fibrolamellar carcinoma of the liver. What is NOT true about fibrolamellar carcinoma of the liver?
Which of the following zones of the liver lobule is more prone to ischemia?
What differentiates chronic persistent hepatitis from chronic active hepatitis?
Alcoholic hyaline in alcoholic liver disease is composed of?
All of the following are true regarding epithelioid hemangioendothelioma except?
Budd-Chiari syndrome occurs in association with which of the following?
Practice by Chapter
Jaundice and Cholestasis
Practice Questions
Viral Hepatitis
Practice Questions
Alcoholic and Non-alcoholic Fatty Liver Disease
Practice Questions
Drug and Toxin Induced Liver Injury
Practice Questions
Cirrhosis and Its Complications
Practice Questions
Metabolic Liver Diseases
Practice Questions
Liver Tumors
Practice Questions
Gallbladder and Biliary Tract Diseases
Practice Questions
Congenital Liver Diseases
Practice Questions
Liver Transplantation Pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
