Immunopathology — MCQs

On this page
All of the following statements are true about Wiskott-Aldrich syndrome, except:
Which of the following diseases is characterized by the features presented?
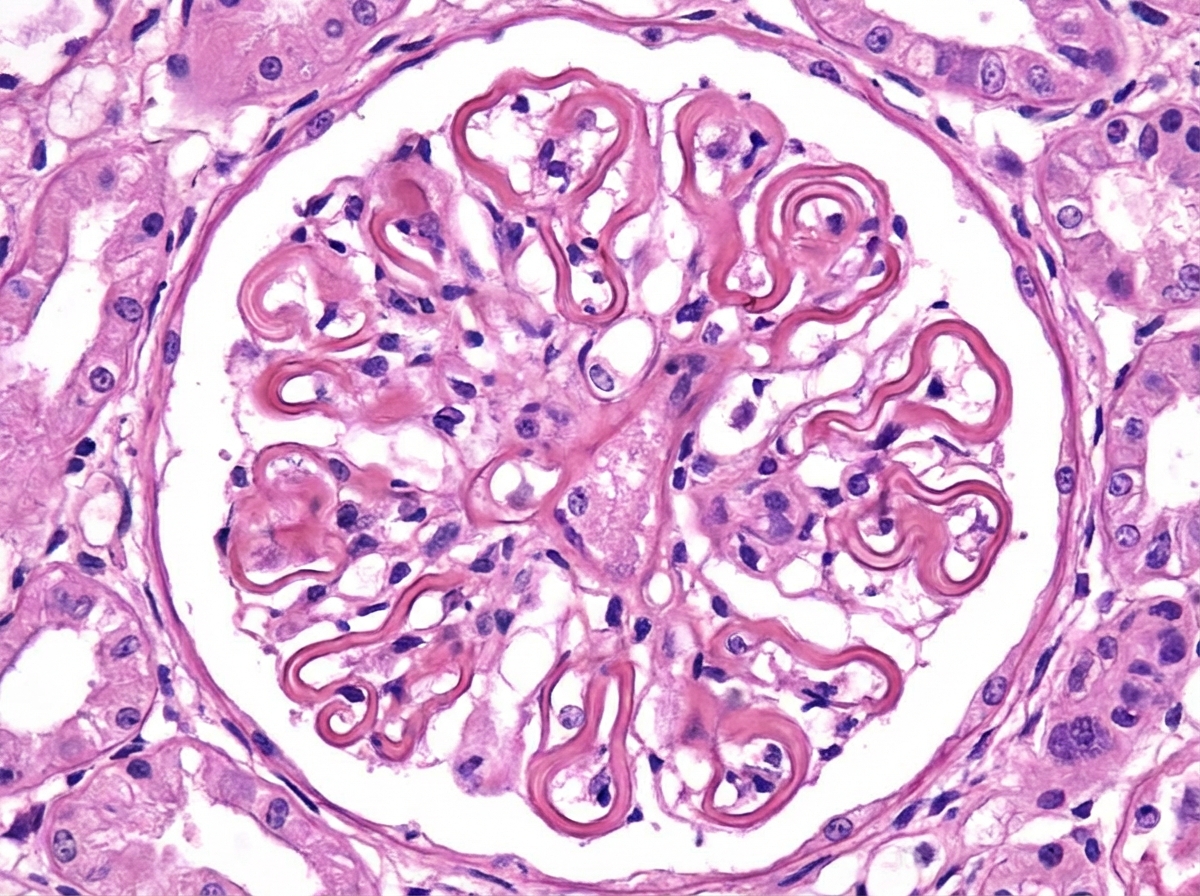
Which type of collagen is primarily affected in Goodpasture syndrome?
Leukocyte adhesion deficiency type 1 is associated with which chromosome?
A 45-year-old woman with autoimmune hemolytic anemia presents with increasing fatigue. Which of the following mediators of inflammation is primarily responsible for antibody-mediated hemolysis in this patient?
DiGeorge's syndrome is due to which of the following?
Which of the following conditions is an example of Type II hypersensitivity?
A patient with recurrent bacterial infections is diagnosed to have a genetic deficiency in myeloperoxidase. What is the cause of this increased susceptibility to infections?
Which of the following hypersensitivity types cannot be detected by a skin test?
A 42-year-old man develops urticaria, stridor, and hypotension during a blood transfusion, requiring IV epinephrine. He has a history of frequent sinusitis and bronchitis. Which is the most likely immunologic deficiency?
Practice by Chapter
Cells and Tissues of the Immune System
Practice Questions
Innate Immunity
Practice Questions
Adaptive Immunity
Practice Questions
Hypersensitivity Reactions
Practice Questions
Autoimmune Diseases
Practice Questions
Immunodeficiency Disorders
Practice Questions
Transplantation Immunopathology
Practice Questions
Immune Response to Infections
Practice Questions
Immunologic Laboratory Techniques
Practice Questions
Tumor Immunology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
