Hematopathology — MCQs

On this page
During a routine blood test among members of a family, abnormally high potassium values were noted. Which hematological anomaly is known to cause such a finding?
Deficiency of all three components of coagulation factor VIII results in which of the following conditions?
A 32-year-old asymptomatic female, not requiring blood transfusion, presents with Hb 13.0 gm/dl. Her HbF levels are 95% and Hb A2 levels are 1.5%. Which of the following is the most likely diagnosis?
Bence Jones proteins are found in all of the following conditions except?
All are examples of microangiopathic hemolytic anemia except?
Dohle bodies can be seen in which of the following conditions?
All of the following are present in cryoprecipitate, except?
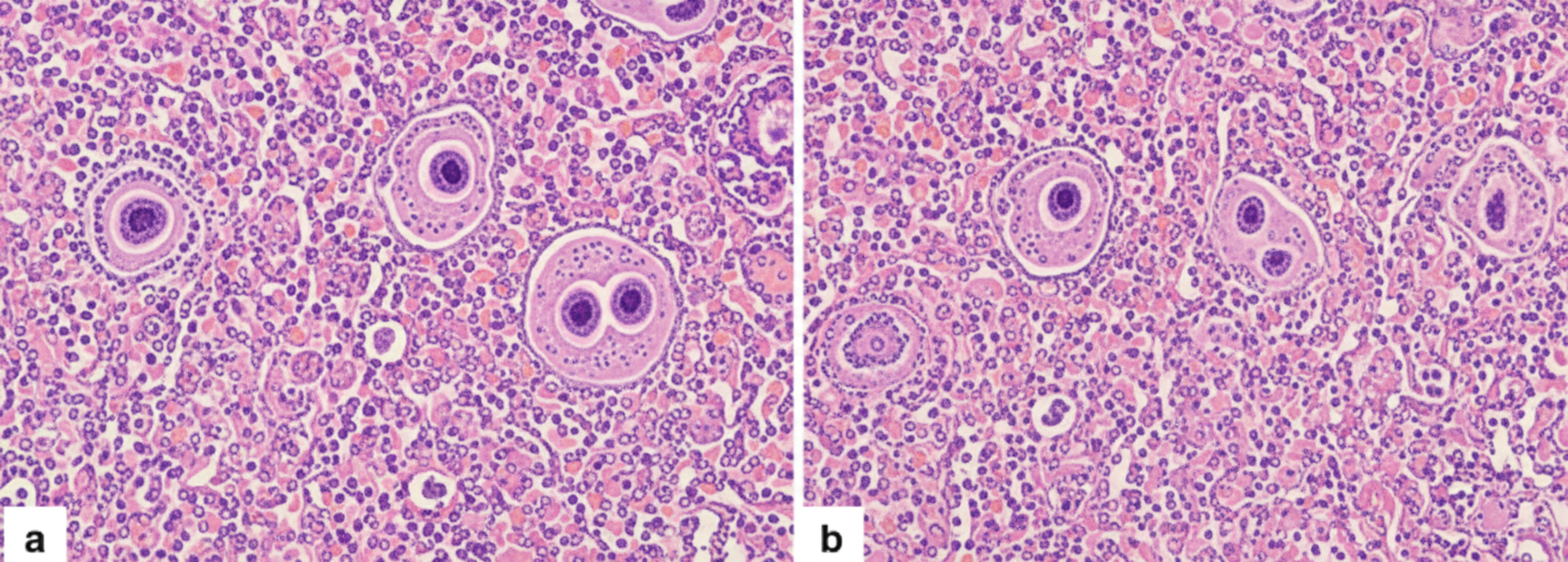
Examination of a lymph node from the neck of a 26-year-old man with bilateral cervical lymphadenopathy reveals total effacement of nodal architecture, and at higher power, the characteristic cell shown below. Which of the following additional studies is best suited for confirmation of diagnosis in this case?
Smudge cells are characteristic findings in which of the following hematological malignancies?
Which blood index most accurately reflects iron deficiency?
Practice by Chapter
Anemias: Classification and Approach
Practice Questions
Hemolytic Anemias
Practice Questions
Myeloproliferative Neoplasms
Practice Questions
Myelodysplastic Syndromes
Practice Questions
Acute Leukemias
Practice Questions
Chronic Leukemias
Practice Questions
Lymphomas and Lymphoid Neoplasms
Practice Questions
Plasma Cell Disorders
Practice Questions
Bleeding Disorders
Practice Questions
Thrombotic Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
