Hematopathology — MCQs

On this page
Hairy cell leukemia is which type of tumor?
The histological feature shown is seen in which of the following conditions?
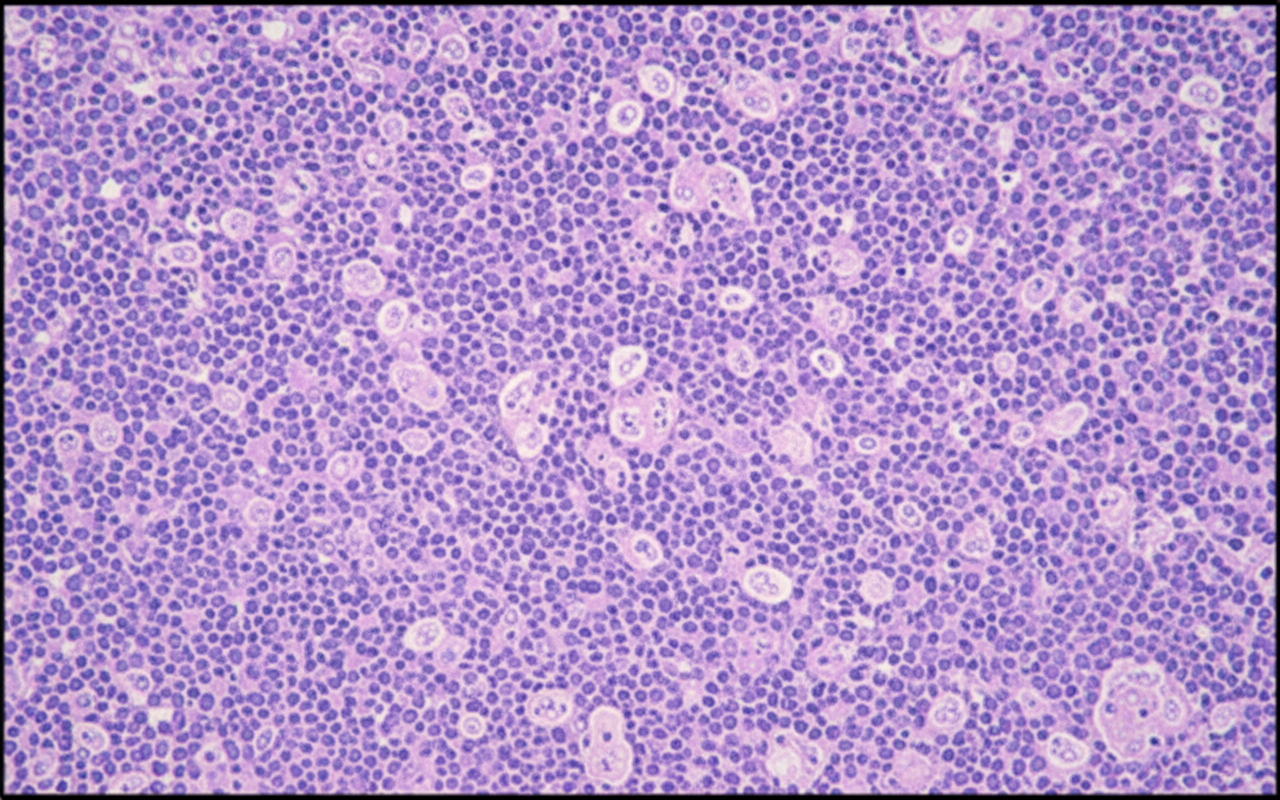
Which of the following statements regarding leukemias is true?
Low LAP score may be seen in the following EXCEPT:
Which of the following toxic states is not associated with anemia?
Which is the most immunogenic RBC blood group system among the given options?
Pancytopenia with hypercellular marrow may be seen due to all of the following except:
Which of the following are types of Hodgkin's lymphoma?
A 36-year-old male presents with weakness, pallor, and bleeding gums. His HB was 7 g/dL, total leukocyte count was 110,000/mm³ with many immature white blood cells positive for MPO, and platelet count was 22,000/mm³. What is the most likely diagnosis?
Microangiopathic hemolytic anemia (MAHA) is a component of all of the following, except?
Practice by Chapter
Anemias: Classification and Approach
Practice Questions
Hemolytic Anemias
Practice Questions
Myeloproliferative Neoplasms
Practice Questions
Myelodysplastic Syndromes
Practice Questions
Acute Leukemias
Practice Questions
Chronic Leukemias
Practice Questions
Lymphomas and Lymphoid Neoplasms
Practice Questions
Plasma Cell Disorders
Practice Questions
Bleeding Disorders
Practice Questions
Thrombotic Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
