Hematopathology — MCQs

On this page
A blood smear is best visualized at which pH?
Which of the following is not associated with the disorder characterized by findings on a peripheral blood smear?
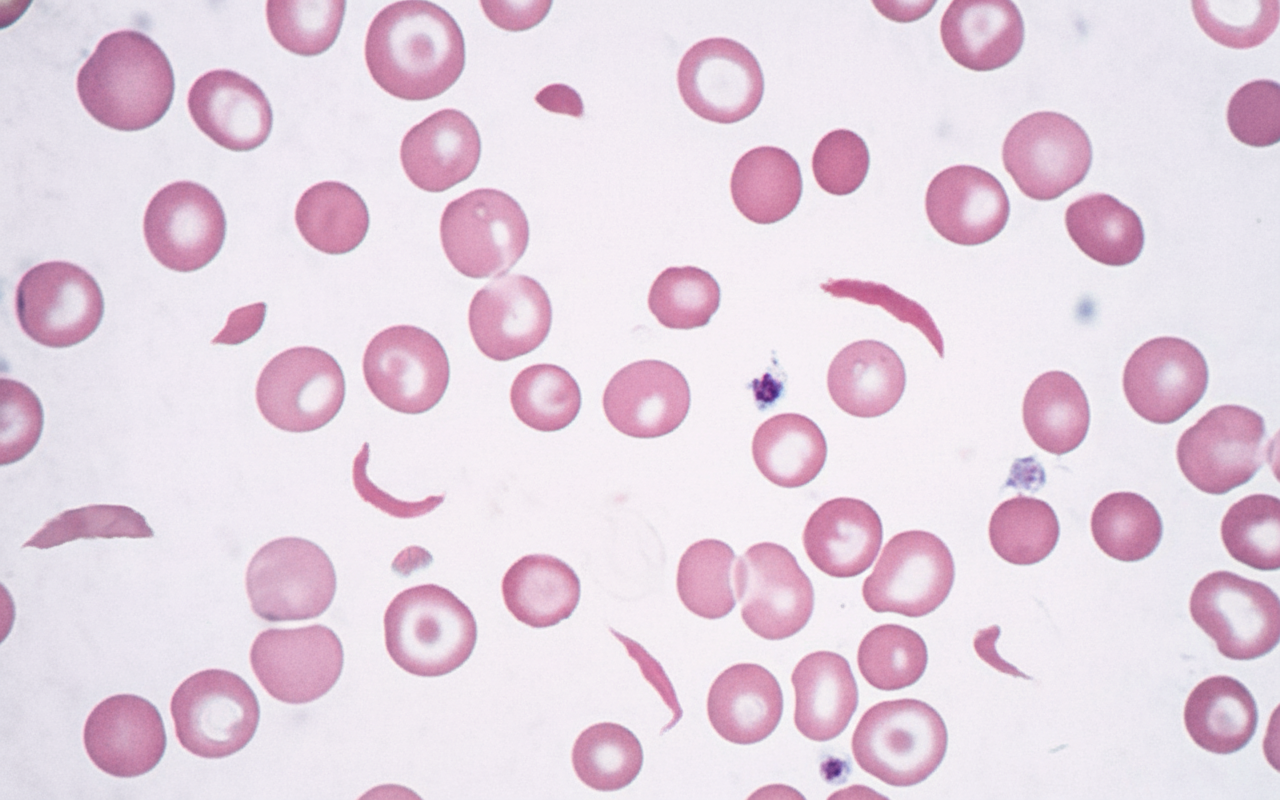
Estimation of the degradation products of the cross-linked fibrin fibers in DIC can best, specifically, and accurately be done by which of the following tests?
Which of the following statements regarding megaloblastic anemia is true?
Stored blood, which has been preserved in a blood bank, is deficient in which of the following coagulation factors?
A 62-year-old man develops itchy, scaling, and non-scaling patches and plaques over his chest and back. The rest of the examination is normal, except for lymphadenopathy. Blood film and skin biopsy histology both reveal unusually large monocytoid cells. Which of the following is the most likely diagnosis?
Which of the following conditions is LEAST likely to be accompanied by lymphocytosis in the peripheral blood?
Which of the following subtypes of Acute Myeloid Leukemia (AML) is characterized by gum hyperplasia, bleeding, and visceral infiltration?
A localized presentation of Non-Hodgkin Lymphoma (NHL) is typically associated with which histological subtype?
A 72-year-old female presents with complaints of generalized lymphadenopathy and a total WBC count of 80,000. Flow cytometry revealed CD19+, CD20+, CD5+, CD23-. Cyclin D1 is positive. Which of the following genetic abnormalities is expected in this condition?
Practice by Chapter
Anemias: Classification and Approach
Practice Questions
Hemolytic Anemias
Practice Questions
Myeloproliferative Neoplasms
Practice Questions
Myelodysplastic Syndromes
Practice Questions
Acute Leukemias
Practice Questions
Chronic Leukemias
Practice Questions
Lymphomas and Lymphoid Neoplasms
Practice Questions
Plasma Cell Disorders
Practice Questions
Bleeding Disorders
Practice Questions
Thrombotic Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
