General Pathology — MCQs

On this page
All of the following are features of reversible cell injury, except?
Which of the following statements regarding pyroptosis is not true?
Which of the following is NOT affected in Graft-Versus-Host disease?
All of the following are autosomal dominant disorders, except?
Which of the following is NOT a component of the Virchow triad?
Psammoma bodies are seen in which of the following conditions?
Aneuploidy is seen with all except:
What does 'adeno lymphoma' refer to?
Examine the above pedigree chart. Which one of the following diseases is the most likely for this situation?
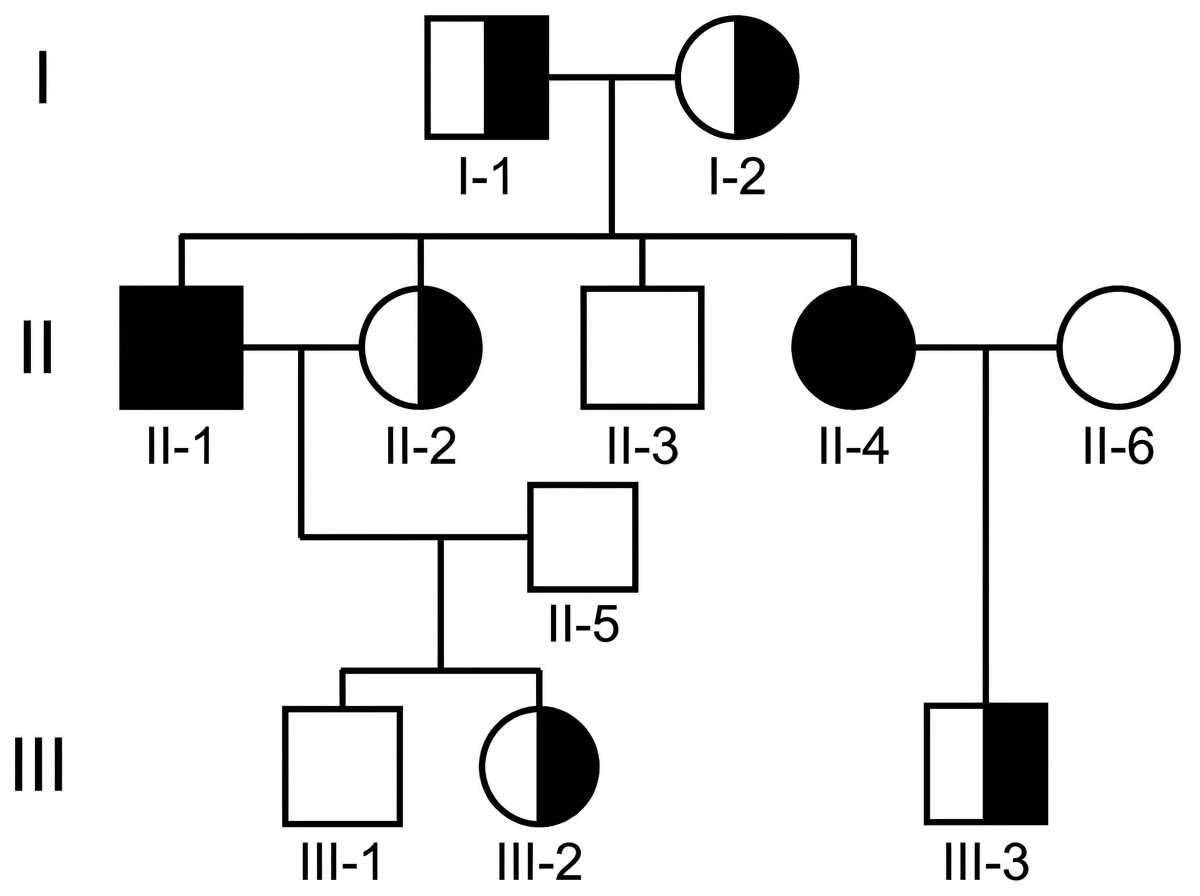
Trisomy 13 is identified as:
Practice by Chapter
Cell Injury and Cell Death
Practice Questions
Adaptations of Cellular Growth
Practice Questions
Accumulations and Deposits
Practice Questions
Acute and Chronic Inflammation
Practice Questions
Tissue Repair and Wound Healing
Practice Questions
Hemodynamic Disorders
Practice Questions
Genetic Disorders
Practice Questions
Environmental Pathology
Practice Questions
Nutritional Diseases
Practice Questions
Molecular Basis of Disease
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
