General Pathology — MCQs

On this page
Which type of necrosis is typically seen in acute pancreatitis?
What is a reason for tissue analysis in surgery?
All of the following mediators of acute inflammation are derived from cells except?
Tooth discolouration due to high bilirubin secretion is seen in which condition?
Which of the following is seen in both apoptosis and necrosis?
Histologic sections of the thymus that reveal reactive follicles with germinal centers are diagnostic of what condition?
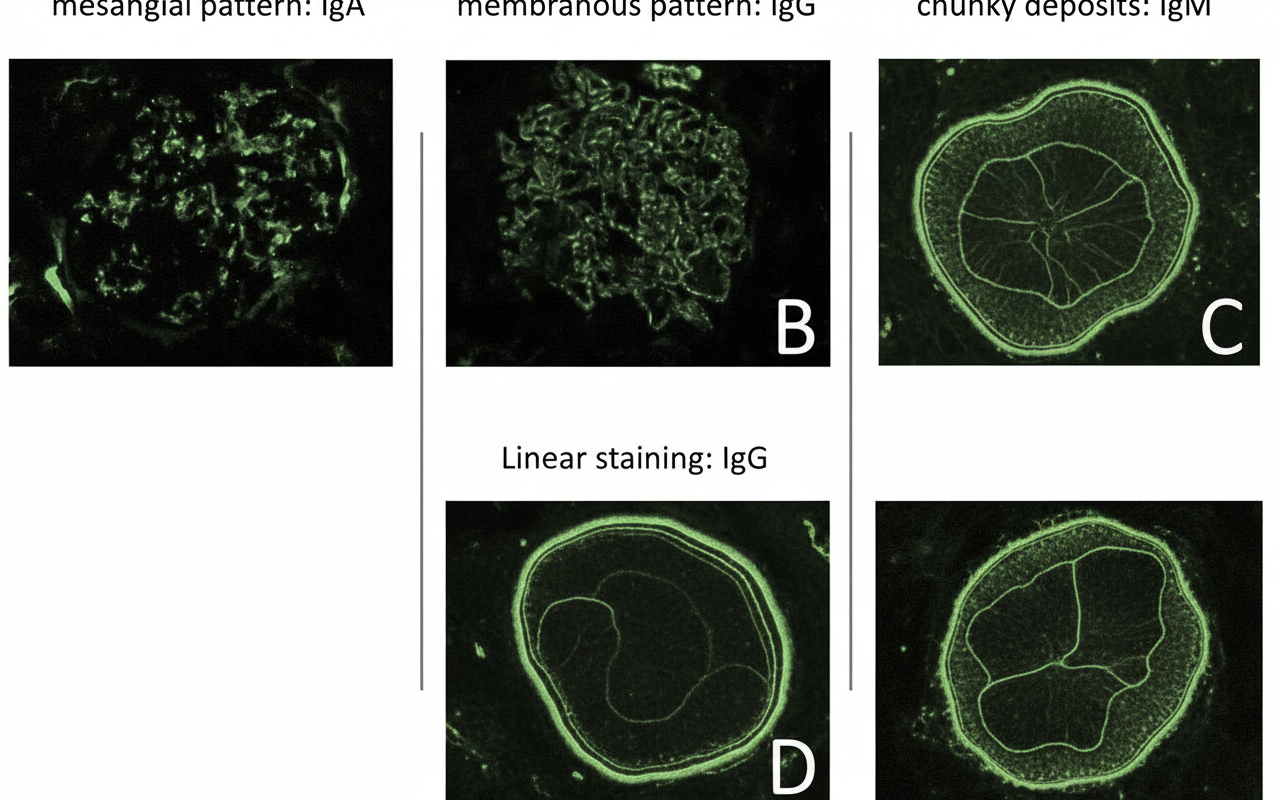
Which of the following types of hypersensitivity reactions is associated with the given condition?
A couple is referred to the physician because their first three pregnancies have ended in spontaneous abortion. Chromosomal analysis reveals that the wife has two cell lines in her blood, one with a missing X chromosome (45,X) and the other normal (46,XX). Her chromosomal constitution can be described as?
Secondary amyloidosis complicates which of the following?
Amyloid protein in human beings is:
Practice by Chapter
Cell Injury and Cell Death
Practice Questions
Adaptations of Cellular Growth
Practice Questions
Accumulations and Deposits
Practice Questions
Acute and Chronic Inflammation
Practice Questions
Tissue Repair and Wound Healing
Practice Questions
Hemodynamic Disorders
Practice Questions
Genetic Disorders
Practice Questions
Environmental Pathology
Practice Questions
Nutritional Diseases
Practice Questions
Molecular Basis of Disease
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
