General Pathology — MCQs

On this page
A 40-year-old male patient complains of muscle and joint pain. The patient has a history of systemic lupus erythematosus. Which type of necrosis is typically associated with the vascular changes seen in this condition?
Which cluster of differentiation (CD) molecule serves as a marker for T lymphocytes?
The AGE-RAGE signaling axis is related to which of the following processes?
All of the following genetic conditions are associated with an increased risk for cancers except?
Apoptosis is inhibited by?
All are features of apoptosis EXCEPT?
ESR is a critical investigation in the diagnosis of TB. Which of the following is true about ESR in TB?
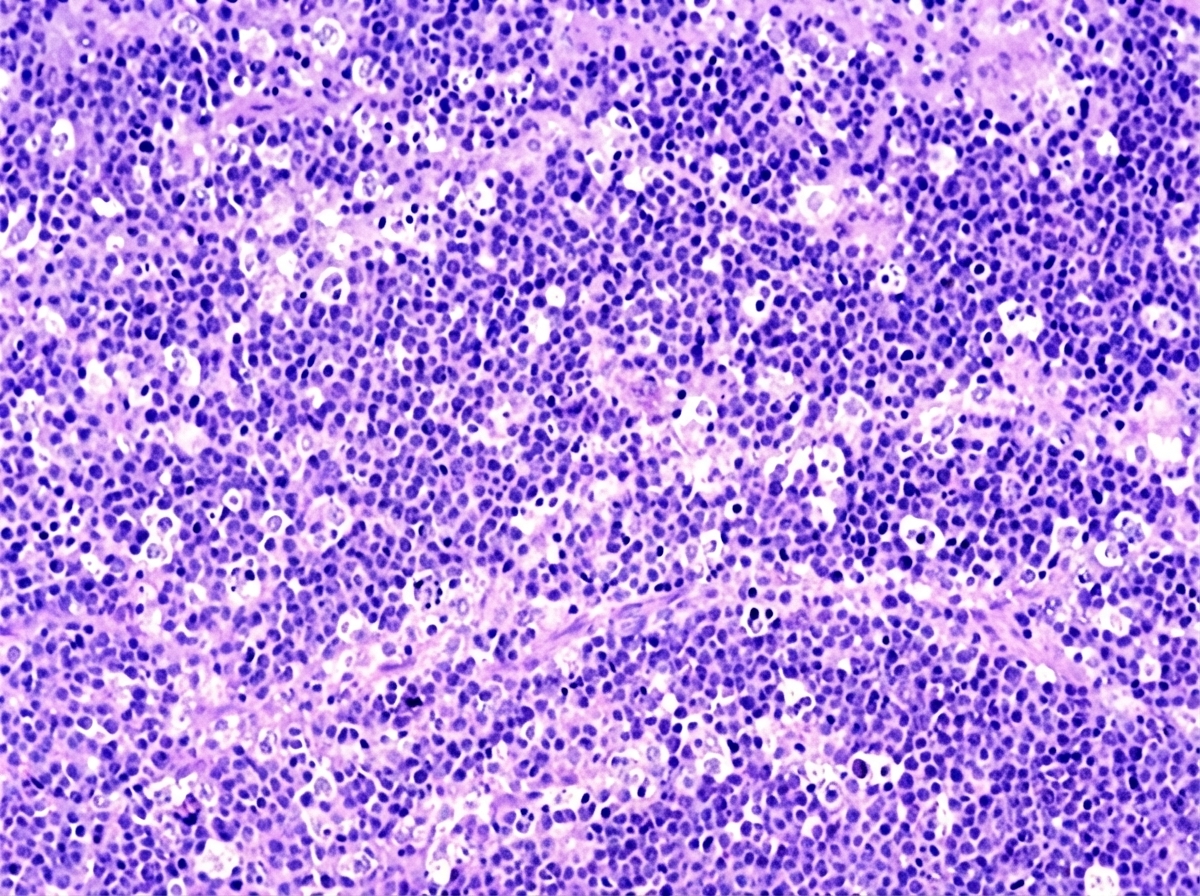
A 4-year-old African boy develops a rapidly enlarging mass that involves the right side of his face. Biopsies of this lesion are shown below. Which chromosomal translocation is associated with this neoplasm?
A 20-year-old female presents for an infertility workup. She has never had a menstrual period. She is short with a broad chest, webbed neck, and low-set ears. It is demonstrated that she has an abnormal karyotype. Which one of the following best describes the cause of this genetic abnormality?
Multiple epidermoid cysts are seen in which of the following conditions?
Practice by Chapter
Cell Injury and Cell Death
Practice Questions
Adaptations of Cellular Growth
Practice Questions
Accumulations and Deposits
Practice Questions
Acute and Chronic Inflammation
Practice Questions
Tissue Repair and Wound Healing
Practice Questions
Hemodynamic Disorders
Practice Questions
Genetic Disorders
Practice Questions
Environmental Pathology
Practice Questions
Nutritional Diseases
Practice Questions
Molecular Basis of Disease
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
