General Pathology — MCQs

On this page
Lipofuscin is associated with which type of atrophy?
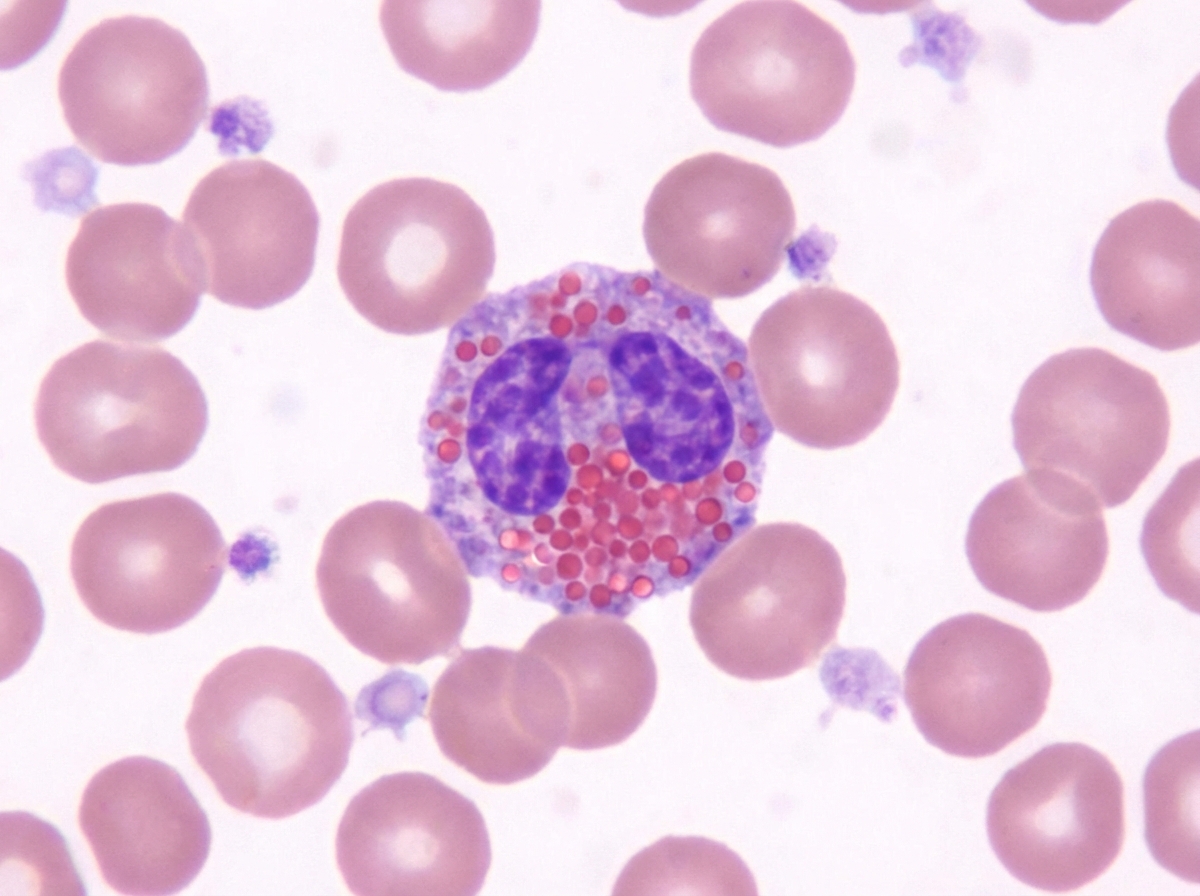
Which cytokine activates the given cell?
A Warthin's tumour is:
Which of the following is NOT a chromosomal breakage syndrome?
All of the following lesions may be classified as odontogenic tumours EXCEPT?
Which finding on electron microscopy indicates irreversible cell injury?
A 32-year-old woman with poorly controlled diabetes mellitus delivers a healthy boy at 38 weeks of gestation. As a result of maternal hyperglycemia during pregnancy, what morphologic response would be expected in the pancreatic islets of the neonate?
Elevated alpha-fetoprotein (AFP) levels are seen in all of the following conditions except?
Annexin V is a marker of which of the following?
Intermediate filaments (IFs) help link adjacent sarcomeres together in skeletal muscle. Which of the following proteins is an intermediate filament protein used diagnostically in pathologic cases to indicate muscle origin?
Practice by Chapter
Cell Injury and Cell Death
Practice Questions
Adaptations of Cellular Growth
Practice Questions
Accumulations and Deposits
Practice Questions
Acute and Chronic Inflammation
Practice Questions
Tissue Repair and Wound Healing
Practice Questions
Hemodynamic Disorders
Practice Questions
Genetic Disorders
Practice Questions
Environmental Pathology
Practice Questions
Nutritional Diseases
Practice Questions
Molecular Basis of Disease
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
