Gastrointestinal Pathology — MCQs

On this page
Collar button ulcer is found in?
Which condition is characterized by skip lesions in the gastrointestinal tract?
A 5-year-old child was admitted to the hospital for a prolapsing rectal mass and painless rectal bleeding. Histopathological examination reveals enlarged and inflamed glands filled with mucin. What is the likely diagnosis?
A 5-year-old child presented with a history of blood in the stools. On examination, there was a polypoid mass in the rectum, a biopsy of which showed as below. The most probable diagnosis is?
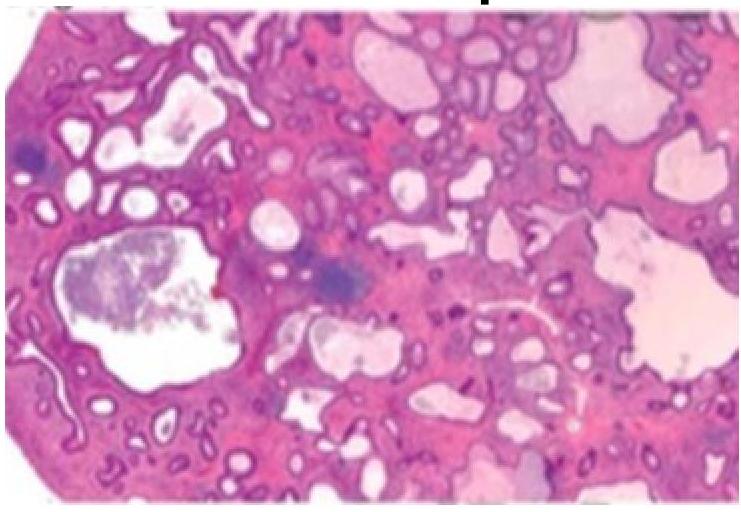
Identify the condition shown in the image.
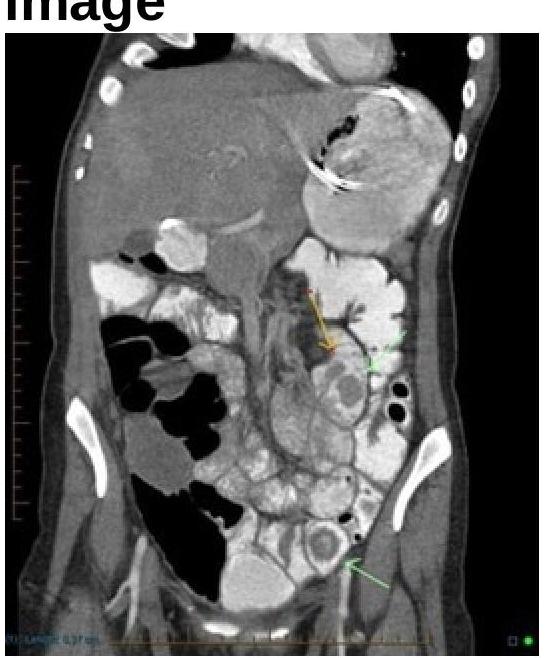
Which of the following statements about Barrett’s esophagus is false?
Which histological feature is more characteristically associated with Ulcerative Colitis compared to Crohn's Disease?
In a patient presenting with gallbladder abnormalities, which condition is characterized by a speckled appearance of the gallbladder mucosa resembling a strawberry?
Most significant risk factor for development of gastric carcinoma is
Centrilobular necrosis of the liver may be seen with?
Practice by Chapter
Oral Cavity and Esophageal Pathology
Practice Questions
Gastritis and Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Malabsorption Syndromes
Practice Questions
Vascular Disorders of Intestine
Practice Questions
Diverticular Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Infections
Practice Questions
Polyps and Neoplasms
Practice Questions
Appendiceal Pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
