Gastrointestinal Pathology — MCQs

On this page
All are true about the esophageal condition shown in the image except:
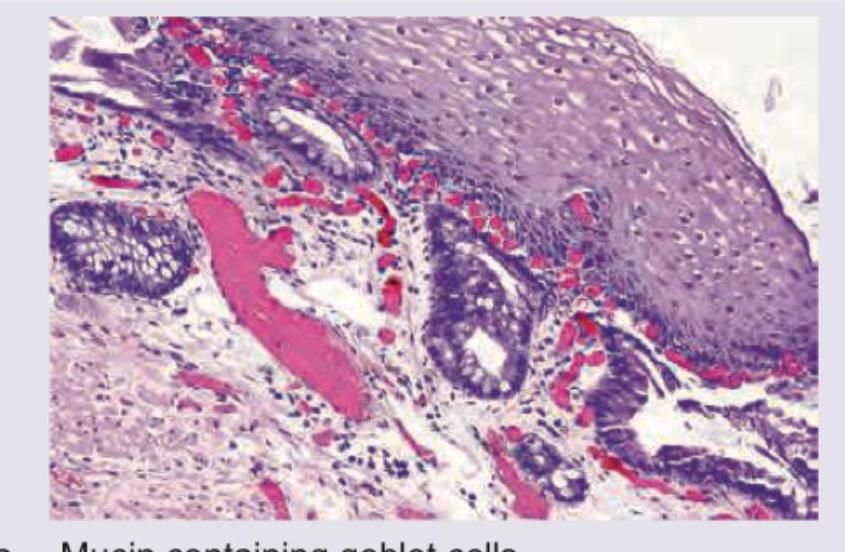
A 35-year-old male patient presents with a history of heartburn. An upper GI endoscopy was done and a biopsy from a suspicious lesion showed the following picture. What does this show? Which special stain will you use for confirmation and what will you look for?
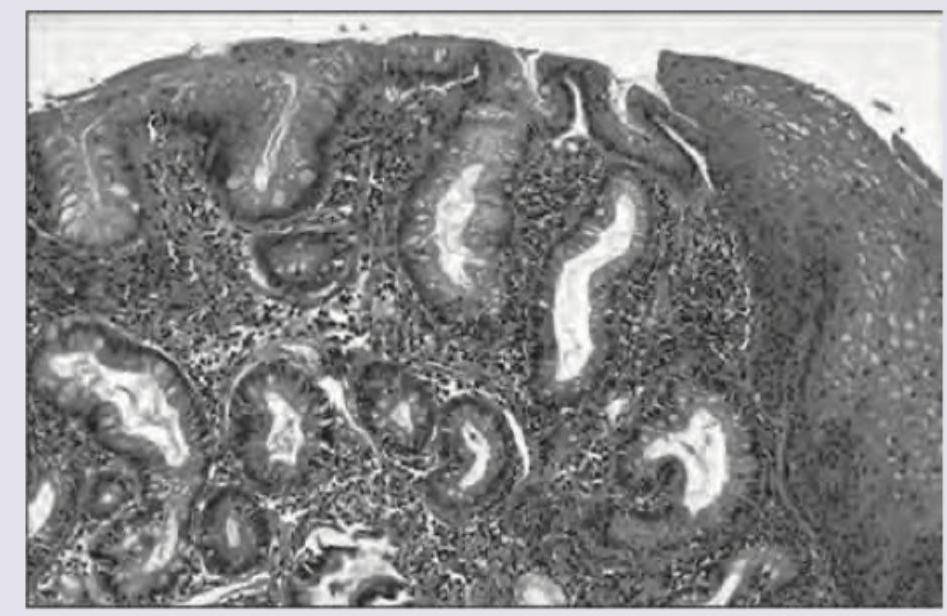
A 15-year-old patient develops intussusception for which he was operated and a segment of intestine showing multiple polyps was resected. The microscopy showed the following pathology. What is the likely diagnosis?
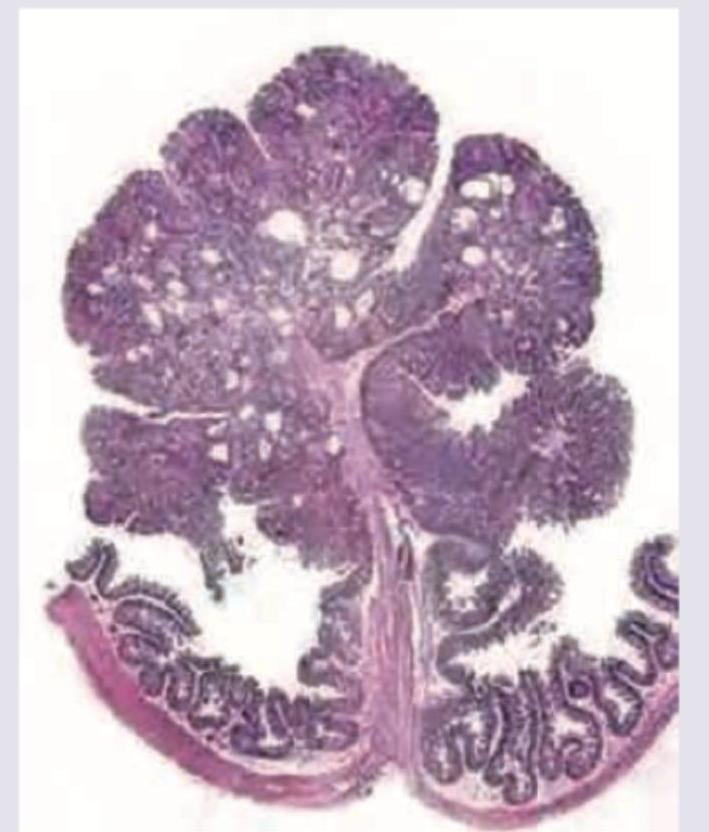
A 50-year-old male presents with colicky abdominal pain and recurrent bloody diarrhea. Colonoscopy shows geographical ulcers. Histopathology is shown below. Diagnosis is:
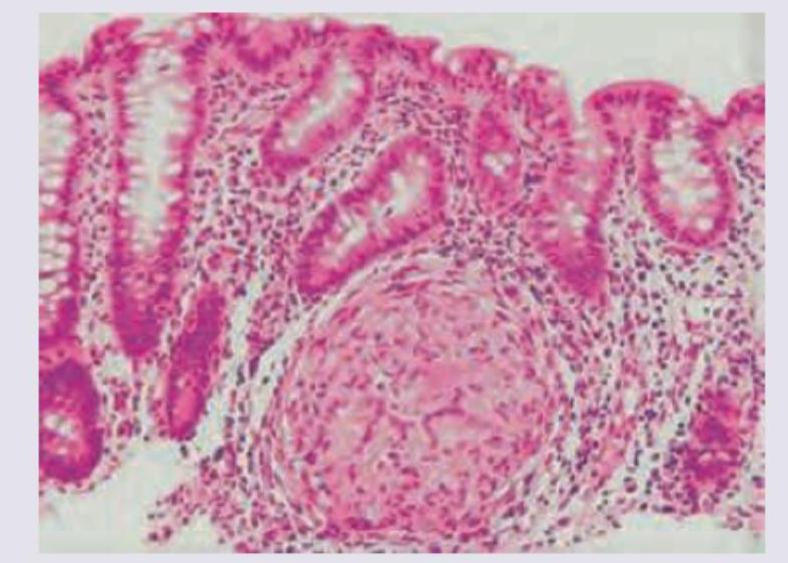
Melanosis coli, which occurs due to long term consumption of stimulant laxatives, presents as brown discolouration of colonic mucosa due to deposition of which one of the following pigments?
Which one of the following is correct regarding Gastrointestinal Stromal Tumour (GIST)?
Consider the following: 1. Cholesterolosis 2. Adenomyomatosis 3. Polyposis 4. Cholelithiasis To which of the above does cholecystoses refer to?
A 40 year old male patient complains of severe acute abdominal pain. Radiologic examination reveals multiple gall stones. On histologic examination, foci of necrosis containing shadowy outlines of necrotic cells surrounded by basophilic calcium deposits were seen. Which type of necrosis is seen in this patient?
Congenital megacolon is confirmed by:
Hirschsprung disease is due to
Practice by Chapter
Oral Cavity and Esophageal Pathology
Practice Questions
Gastritis and Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Malabsorption Syndromes
Practice Questions
Vascular Disorders of Intestine
Practice Questions
Diverticular Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Infections
Practice Questions
Polyps and Neoplasms
Practice Questions
Appendiceal Pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
