Gastrointestinal Pathology — MCQs

On this page
What is the most common location for a carcinoid tumor?
Puetz-Jegher syndrome is characterised by
Glossodynia is defined as:
A 49-year-old female taking ibuprofen for increasing joint pain in her hands presents with increasing pain in her midsternal area. Gastroscopy reveals multiple, scattered, punctate hemorrhagic areas in her gastric mucosa. Biopsies from one of these hemorrhagic lesions reveal mucosal erosions with edema and hemorrhage. No mucosal ulceration is seen. What is the most likely diagnosis?
In Barrett's oesophagus, which of the following epithelial transformations occurs?
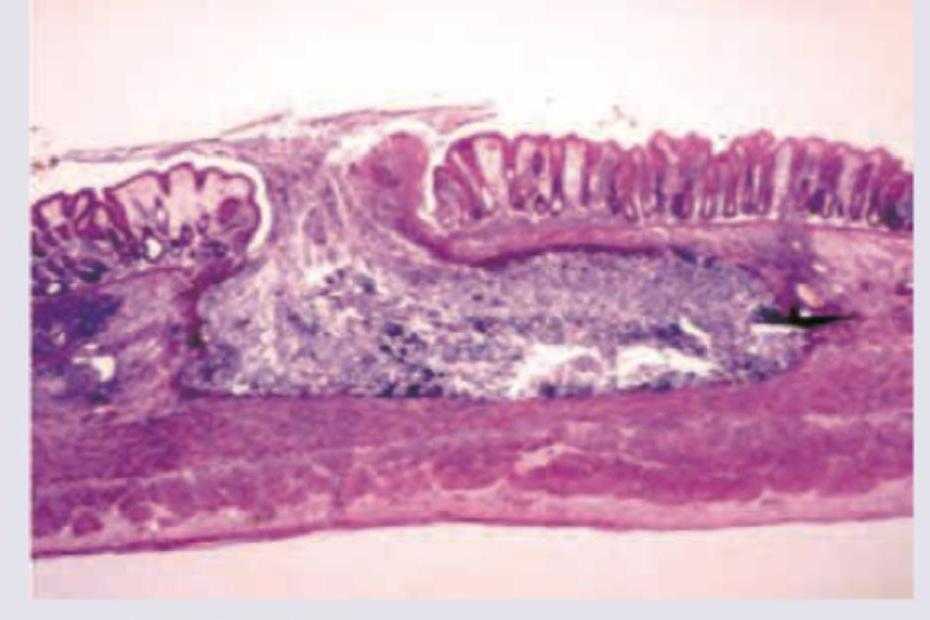
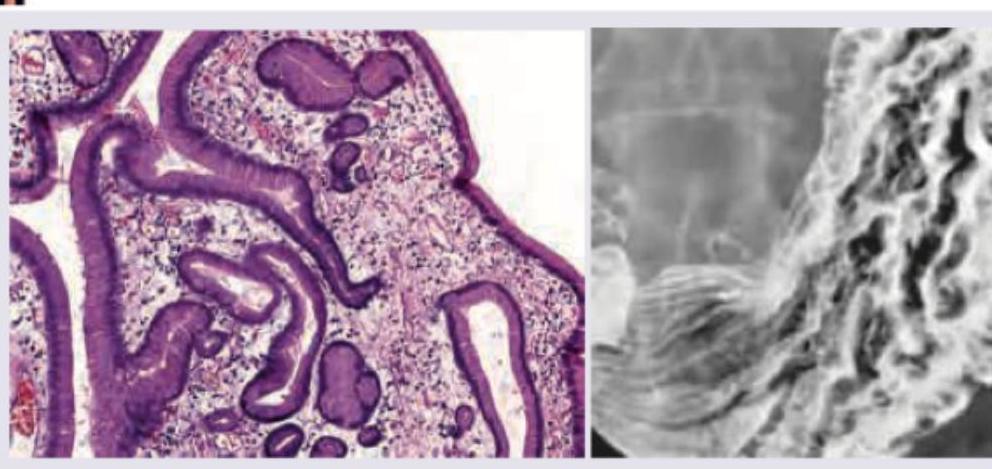
The following histological slide demonstrates:
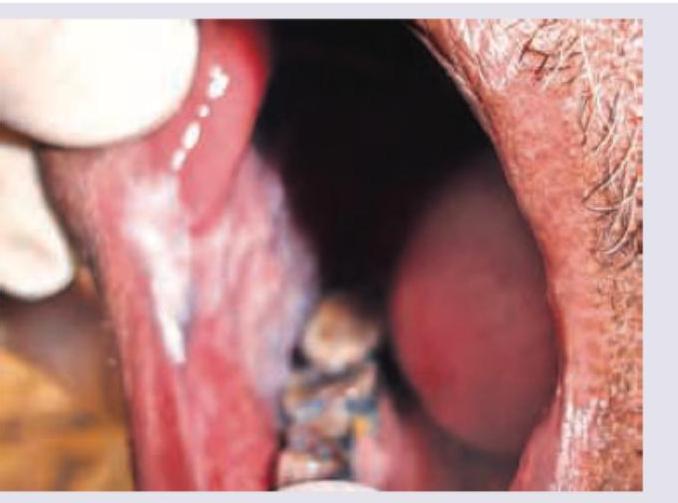
A 60-year-old man with tobacco chewing history presents with trismus and ankyloglossia. The lesion is shown below. Diagnosis is? (NEET Pattern 2018)
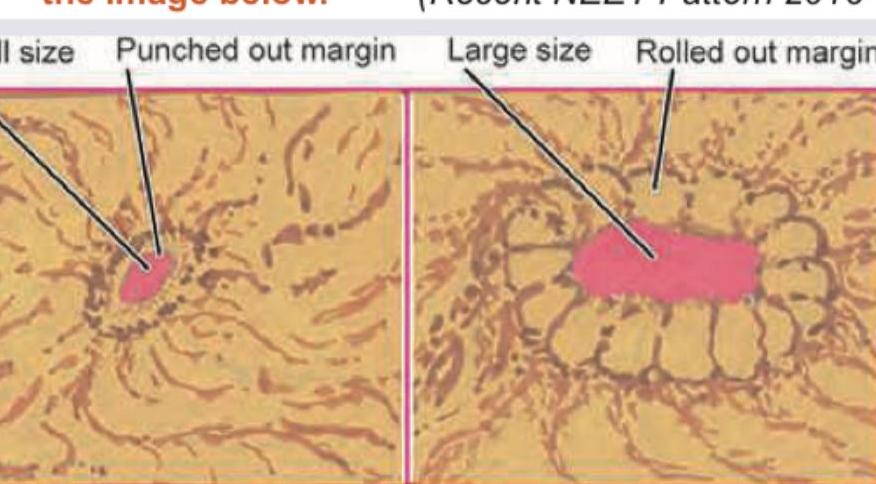
Identify the types of gastric ulcers labeled A and B in the image below.
The following specimen of esophagus and biopsy performed shows all except:
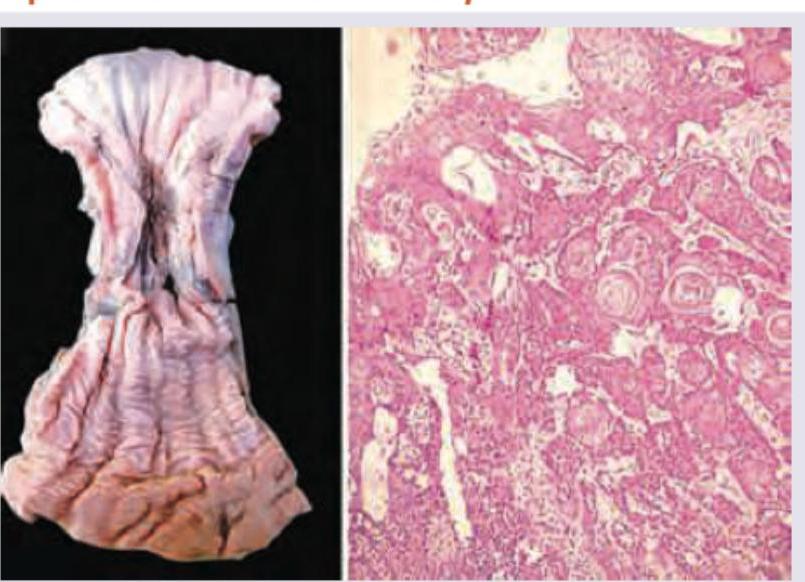
All are true about the condition shown except:
Practice by Chapter
Oral Cavity and Esophageal Pathology
Practice Questions
Gastritis and Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Malabsorption Syndromes
Practice Questions
Vascular Disorders of Intestine
Practice Questions
Diverticular Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Infections
Practice Questions
Polyps and Neoplasms
Practice Questions
Appendiceal Pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
