Gastrointestinal Pathology — MCQs

On this page
Toxic megacolon is a complication of which of the following conditions?
Which of the following statements is false regarding familial polyposis colon cancer syndrome?
Which of the following conditions shows the most specific change in a biopsy?
Mixed tumors of the salivary glands are most commonly found in which location?
Which of the following is NOT typically seen in Ulcerative colitis?
Biopsy of the lower esophagus in a patient with chronic reflux demonstrates epithelial metaplasia. Which of the following cell types was most likely observed in the involved areas?
Which of the following polyps is not premalignant?
This is a specimen of which condition?
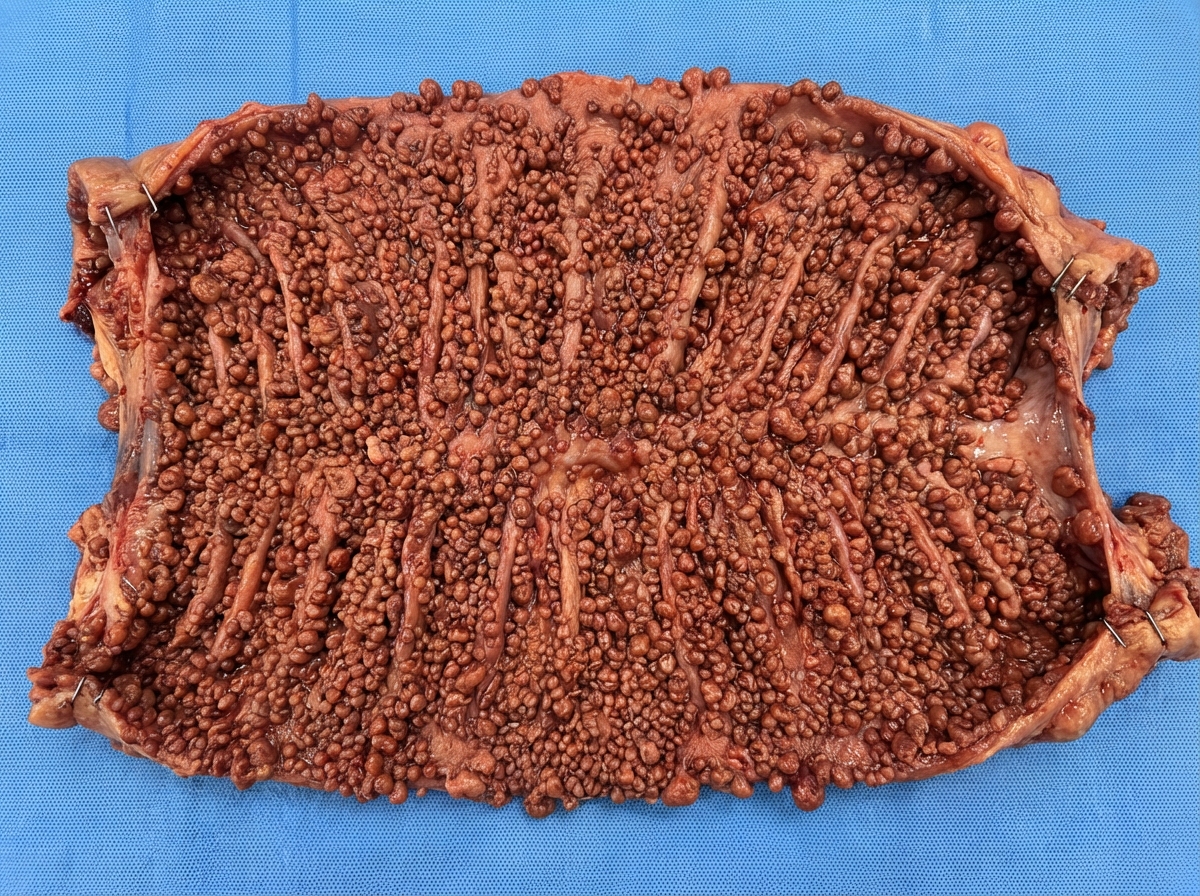
What is the most common tumor of the small intestine?
Which of the following is NOT true regarding the intestinal type of gastric carcinoma?
Practice by Chapter
Oral Cavity and Esophageal Pathology
Practice Questions
Gastritis and Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Malabsorption Syndromes
Practice Questions
Vascular Disorders of Intestine
Practice Questions
Diverticular Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Infections
Practice Questions
Polyps and Neoplasms
Practice Questions
Appendiceal Pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
