Gastrointestinal Pathology — MCQs

On this page
Barrett's esophagus is characterized by which of the following histological changes?
Which of the following is NOT true about Menetrier's disease?
What is the most common congenital anomaly of the gastrointestinal tract?
Which of the following is the most prominent feature of immunoproliferative small intestinal disease (IPSID)?
Which of the following is associated with Familial Adenomatous Polyposis (FAP)?
What is the term for gas-filled cysts found in the subserosa or submucosa of the small intestine or colon?
Which mutation is NOT seen in diffuse type of gastric cancer?
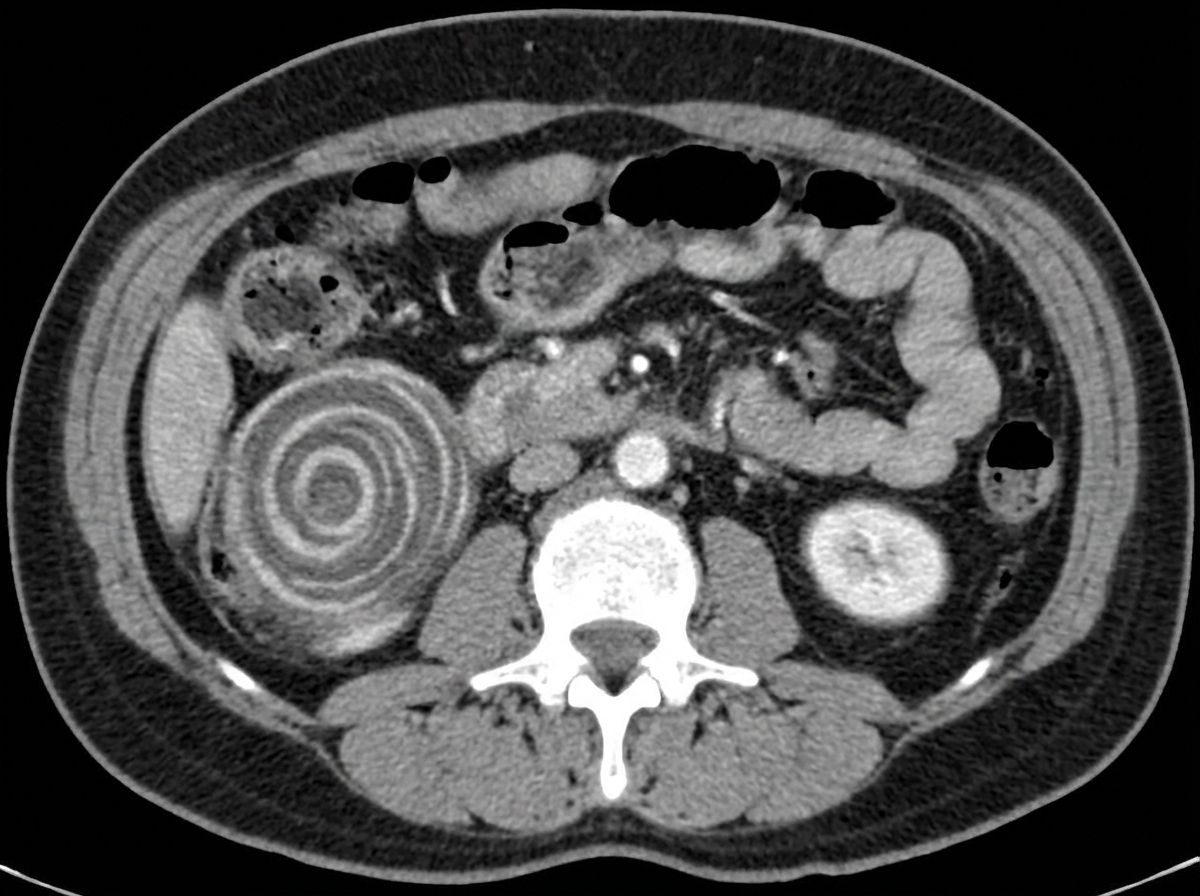
A 51-year-old male presents with blood-stained stools and abdominal pain. Based on the image shown, what is the most likely diagnosis?
Morphologic features of celiac disease include all, except?
All of the following polyps are premalignant except?
Practice by Chapter
Oral Cavity and Esophageal Pathology
Practice Questions
Gastritis and Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Malabsorption Syndromes
Practice Questions
Vascular Disorders of Intestine
Practice Questions
Diverticular Disease
Practice Questions
Intestinal Obstruction
Practice Questions
Gastrointestinal Infections
Practice Questions
Polyps and Neoplasms
Practice Questions
Appendiceal Pathology
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
