Endocrine Pathology — MCQs

On this page
A 24-year-old male presented with a swelling on the anterior aspect of the neck. On examination, the swelling was firm and moved with deglutition. A biopsy from the lesion is shown. What is the typical finding and diagnosis?
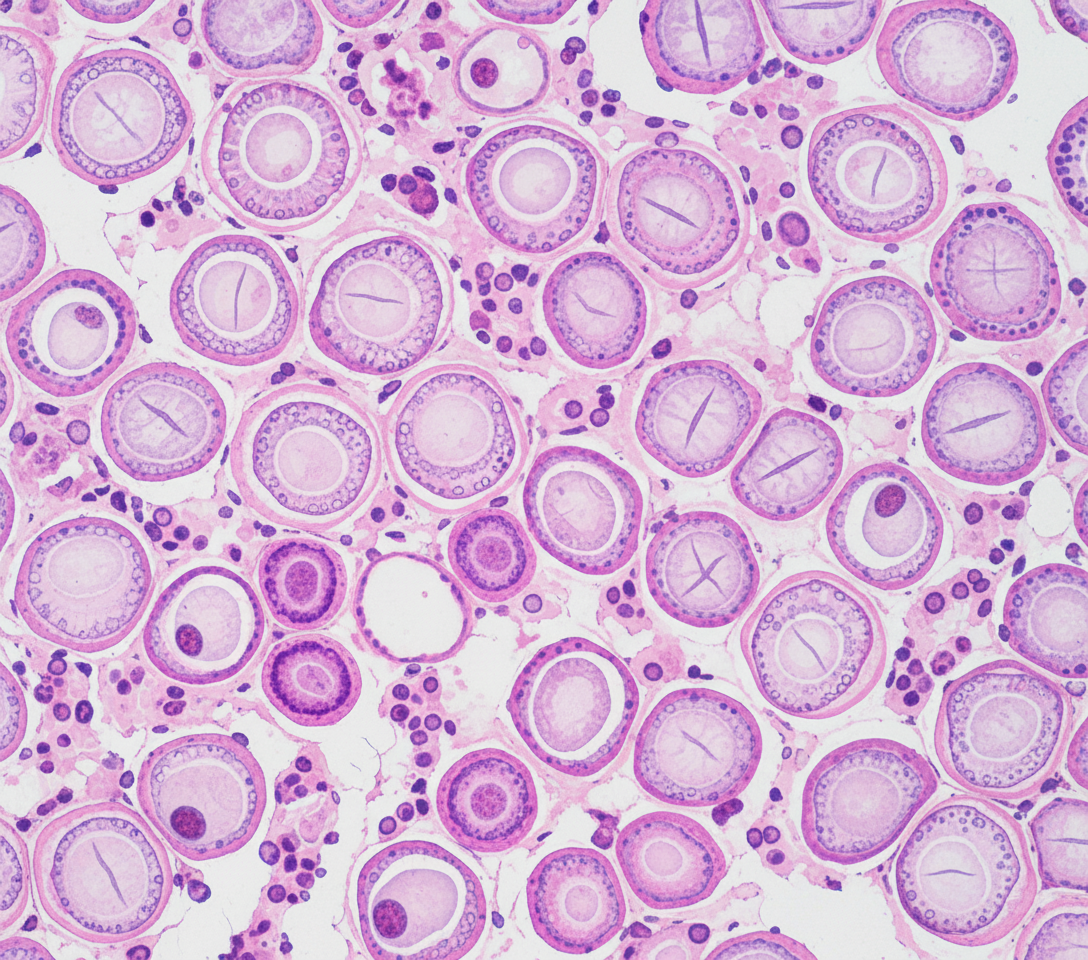
Which of the following features is NOT seen in papillary carcinoma of the thyroid?
Psammoma bodies in a thyroid lesion or the adjacent metastatic lymph nodes increase the possibility of which diagnosis?
What is characteristic of parathyroid carcinoma?
Hashimoto's disease is:
What is the prognosis of thyroid cancer?
A 27-year-old female presented with a long-standing 2 cm x 2 cm nodule in the right lobe of her thyroid, for which she underwent a right hemithyroidectomy. What is the most likely histopathological finding given these clinical details?
A 40-year-old female patient complains of a painless anterior neck mass. She has a history of hypothyroidism. Her blood work suggests increased TSH levels and decreased T3 and T4 levels. Circulating thyroid autoantibodies are also confirmed. What is the most likely diagnosis?
What is the pathognomic feature of hyperparathyroidism?
A 25-year-old man presents with 3 months of polyuria and increased thirst. The patient suffered trauma to the base of the skull in a motorcycle accident 4 months ago. A 24-hour urine collection shows polyuria but no evidence of hematuria, glucosuria, or proteinuria. The pathogenesis of polyuria in this patient is most likely caused by a lesion in which of the following areas of the brain?
Practice by Chapter
Pituitary Gland Disorders
Practice Questions
Thyroid Gland Diseases
Practice Questions
Parathyroid Gland Pathology
Practice Questions
Adrenal Cortical Disorders
Practice Questions
Adrenal Medullary Disorders
Practice Questions
Pancreatic Endocrine Disorders
Practice Questions
Multiple Endocrine Neoplasia Syndromes
Practice Questions
Diffuse Neuroendocrine System
Practice Questions
Pineal Gland Pathology
Practice Questions
Laboratory Diagnosis of Endocrine Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
