Endocrine Pathology — MCQs

On this page
Which of the following is true about the development of thyroid tumors in nodular goiter?
In which condition is thymic hyperplasia commonly observed?
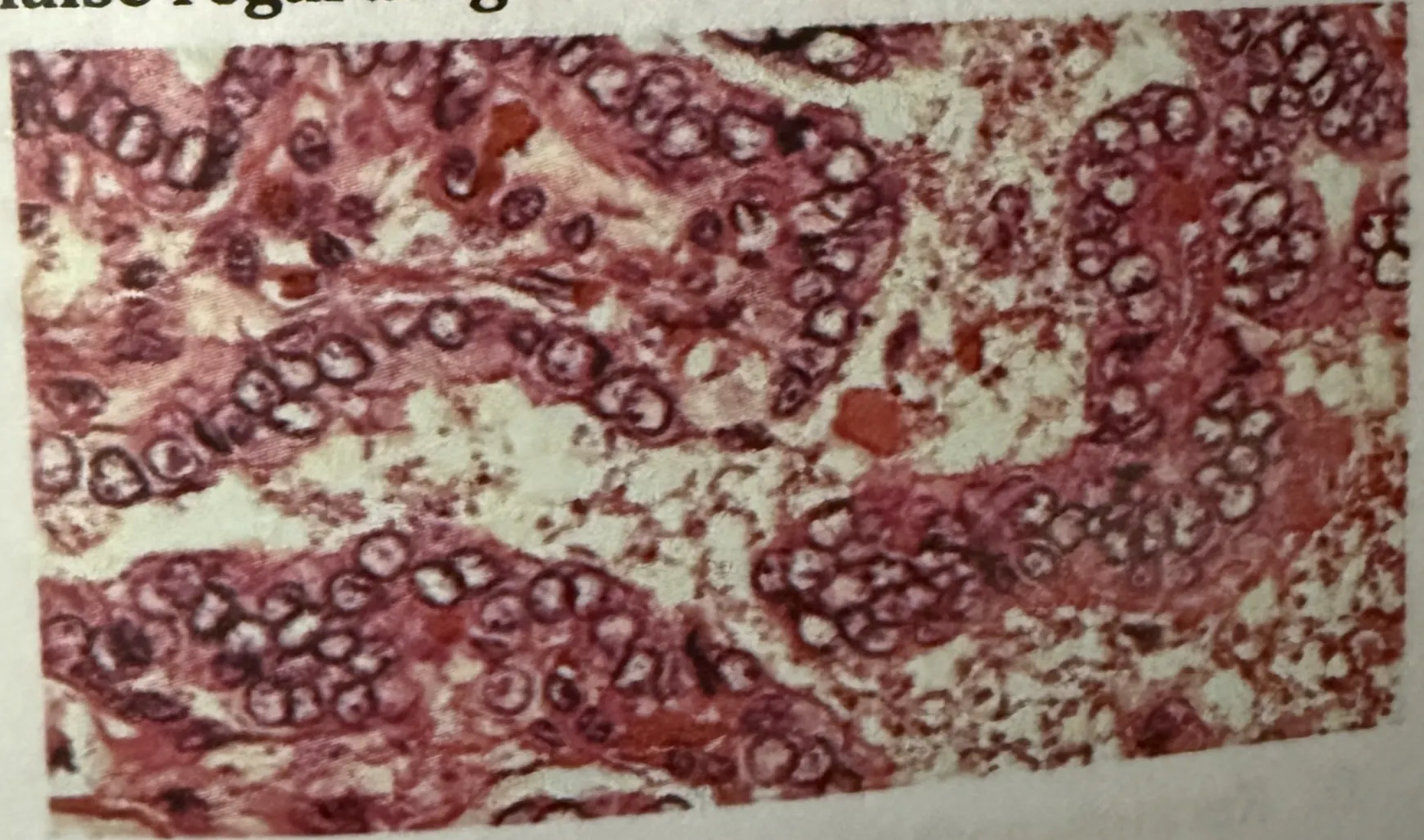
A middle aged male patient presents with painless slow growing neck swelling. On examination, lymph nodes are positive. Surgery is done and biopsy is shown in the image below. Which of the following is false regarding the HPE findings?
A 30-year-old woman presents with thyroid swelling. On investigations, her TSH levels are found to be elevated. Postoperative reports showed lymphocytic infiltration and Hurthle cells. A most probable diagnosis is?
All of the following are features of granulomatous thyroiditis except?
Orphan Annie nuclei are characteristic of which of the following?
Which of the following is a definitive feature of malignant pheochromocytoma?
Which of the following thyroid carcinomas cannot be definitively diagnosed by fine needle aspiration cytology (FNAC)?
What is the most common thyroid tumor associated with multiple endocrine neoplasia (MEN)?
All of the following are histological features of Hashimoto thyroiditis, except which of the following?
Practice by Chapter
Pituitary Gland Disorders
Practice Questions
Thyroid Gland Diseases
Practice Questions
Parathyroid Gland Pathology
Practice Questions
Adrenal Cortical Disorders
Practice Questions
Adrenal Medullary Disorders
Practice Questions
Pancreatic Endocrine Disorders
Practice Questions
Multiple Endocrine Neoplasia Syndromes
Practice Questions
Diffuse Neuroendocrine System
Practice Questions
Pineal Gland Pathology
Practice Questions
Laboratory Diagnosis of Endocrine Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
