Endocrine Pathology — MCQs

On this page
A 45-year-old male presents with a neck mass. Fine needle aspiration shows pleomorphic cells with grooved nuclei (coffee bean appearance), nuclear pseudoinclusions, and psammoma bodies. What is the most likely diagnosis?
A patient presents with a mass in the front of the neck, along with odynophagia and dyspnea. Histopathology reveals tumor cells positive for TTF-1, synaptophysin, and chromogranin, and there is evidence of amyloid deposition. What is the most likely diagnosis?
Osteitis fibrosa cystica is a feature of
The following is a histopathological image of thyroid pathology. What is the diagnosis?
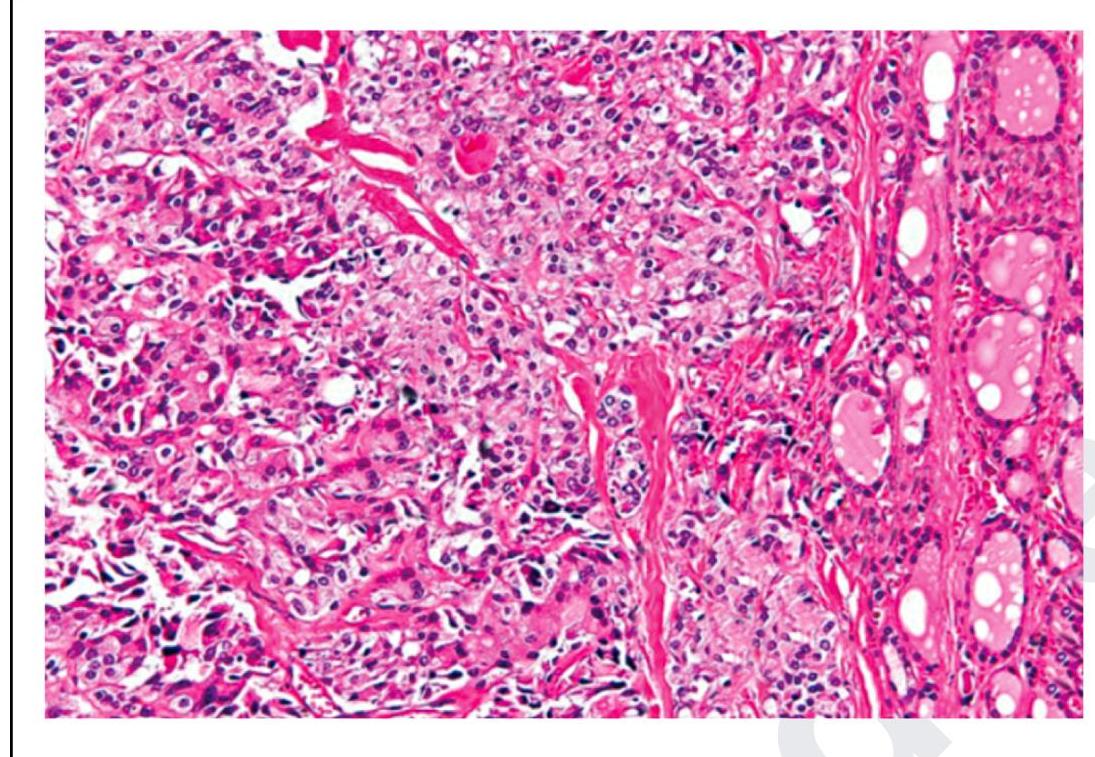
A thyroid FNA shows 'bubble gum' colloid. Which nuclear feature would best support papillary thyroid carcinoma?
Malignancy in a multinodular goiter is most often:-
Nesidioblastoma is due to hyperplasia of?
Which of the following occurs in long standing goitre:
Marker for pancreatic non-functional neuro-endocrine tumor is
A patient presents with neck swelling causing compression of the trachea and esophagus. Histopathological assessment reveals cell nests and pink extracellular amyloid stroma. What is the cell of origin of the tumor associated with these findings?
Practice by Chapter
Pituitary Gland Disorders
Practice Questions
Thyroid Gland Diseases
Practice Questions
Parathyroid Gland Pathology
Practice Questions
Adrenal Cortical Disorders
Practice Questions
Adrenal Medullary Disorders
Practice Questions
Pancreatic Endocrine Disorders
Practice Questions
Multiple Endocrine Neoplasia Syndromes
Practice Questions
Diffuse Neuroendocrine System
Practice Questions
Pineal Gland Pathology
Practice Questions
Laboratory Diagnosis of Endocrine Diseases
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
