Cardiac Pathology — MCQs

On this page
What is the most common site of myocardial infarction?
What is the most likely diagnosis in a patient presenting with large, friable, irregular vegetations on the heart valves?
Early granulation tissue in acute myocardial infarction is typically seen within which timeframe?
Myxoma commonly arises from which chamber of the heart?
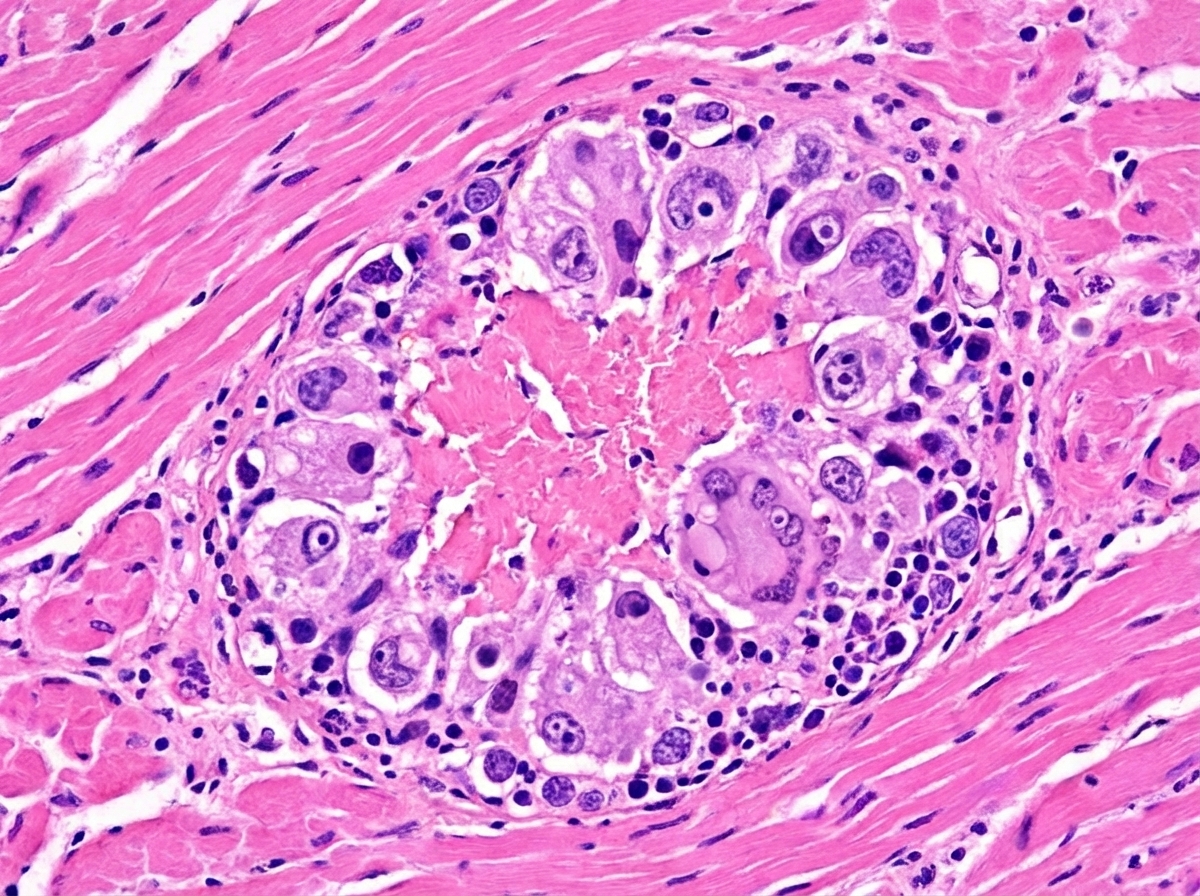
A 15-year-old boy presented with pancarditis. A myocardial biopsy showed a specific finding. What is the most likely diagnosis based on this finding?
Vegetations on the undersurface of Aortic and Mitral (A.V.) valves are found in which condition?
Which of the following is not seen in the early phase of myocardial infarction on microscopy?
Cardiac involvement in carcinoid syndrome is characterized by which of the following?
Which autopsy finding is characteristic after 12 hours in a case of death due to myocardial infarction?
What is the pathognomonic feature of rheumatic heart disease?
Practice by Chapter
Congenital Heart Disease
Practice Questions
Ischemic Heart Disease
Practice Questions
Hypertensive Heart Disease
Practice Questions
Valvular Heart Disease
Practice Questions
Myocarditis and Cardiomyopathies
Practice Questions
Pericardial Disease
Practice Questions
Cardiac Tumors
Practice Questions
Heart Failure Pathophysiology
Practice Questions
Cardiac Transplantation Pathology
Practice Questions
Endocarditis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
