Cardiac Pathology — MCQs

On this page
What is the major histological feature of myocardial infarction?
Senile cardiac amyloidosis is due to deposition of amyloid which is similar to which of the following proteins?
Which of the following is the most common tumor of the heart?
What is the characteristic pathological finding in carcinoid of the heart?
A 15-year-old boy died suddenly while playing in the field. On autopsy, fibrofatty replacement of the right ventricular myocardium is seen. What is the most likely diagnosis?
Which type of cardiomyopathy is characterized by contractile dysfunction?
Which is the most sensitive and specific marker for myocardial infarction?
A 25-year-old basketball player suddenly collapsed during an athletic event and died. Autopsy revealed a hypertrophied septum. What is the most probable diagnosis?
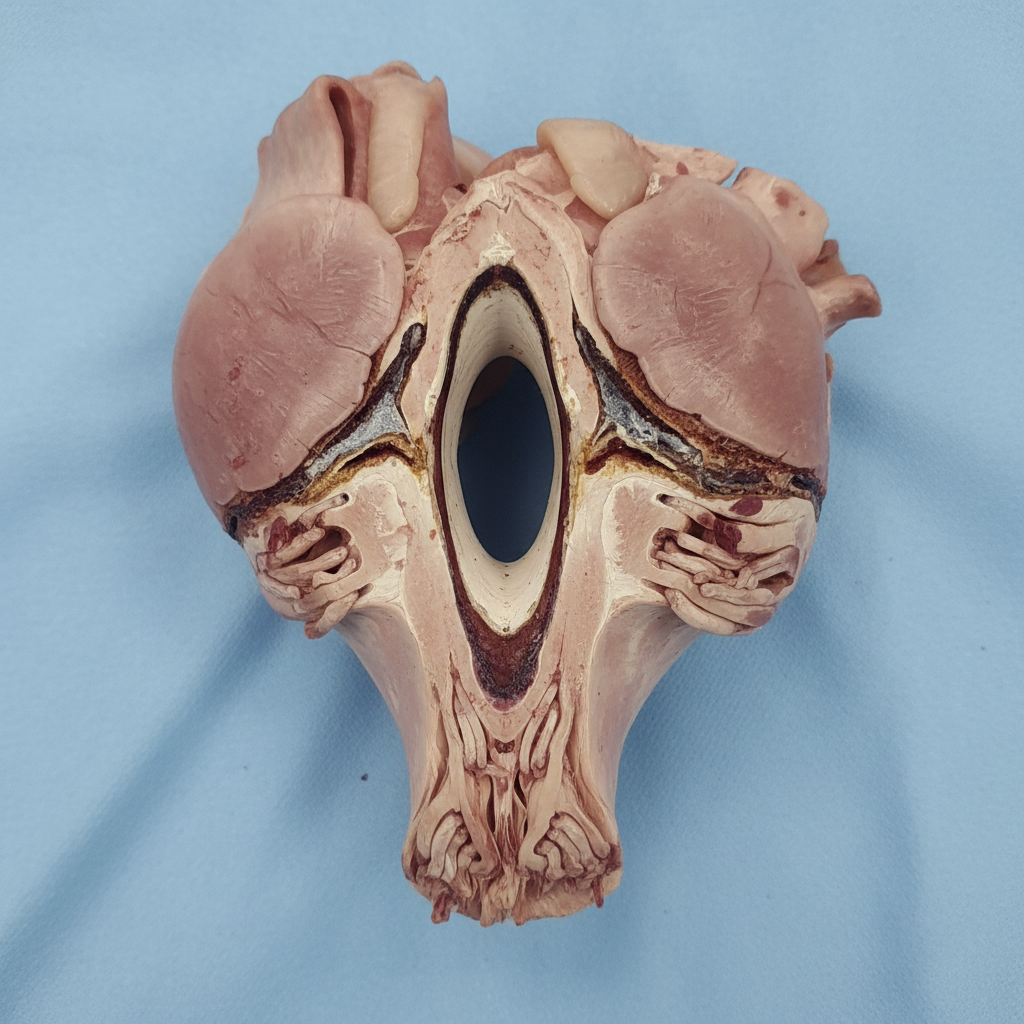
A 30-year-old male patient presented with dyspnea. Echocardiography showed mitral stenosis with left atrial hypertrophy. The excised mitral valve is shown in the image. What is the most likely diagnosis given the findings?
Which of the following statements about Nonbacterial thrombotic endocarditis (NBTE) is false?
Practice by Chapter
Congenital Heart Disease
Practice Questions
Ischemic Heart Disease
Practice Questions
Hypertensive Heart Disease
Practice Questions
Valvular Heart Disease
Practice Questions
Myocarditis and Cardiomyopathies
Practice Questions
Pericardial Disease
Practice Questions
Cardiac Tumors
Practice Questions
Heart Failure Pathophysiology
Practice Questions
Cardiac Transplantation Pathology
Practice Questions
Endocarditis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
