Cardiac Pathology — MCQs

On this page
A 5-year-old child presents with fever with chest pain. On auscultation, pericardial friction rub was heard with bilaterally clear lung fields. The Histopathological finding shows presence of:
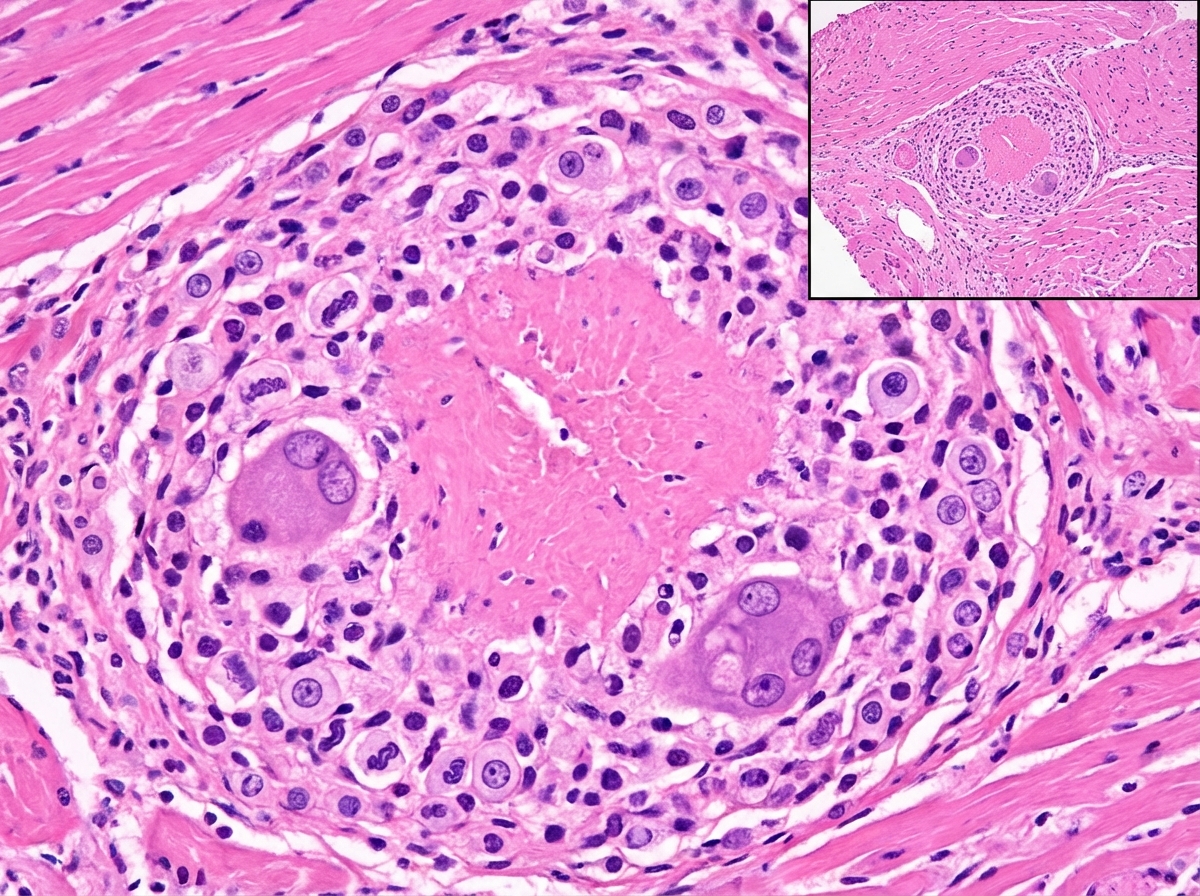
The following image shows presence of:
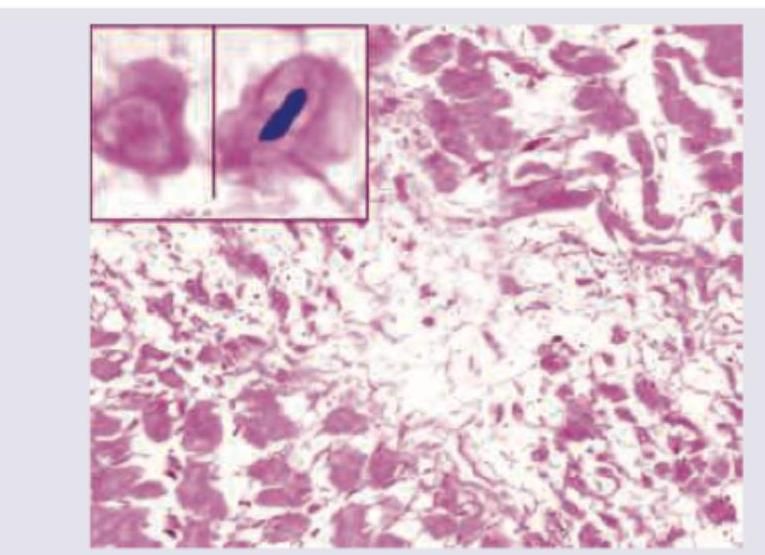
The image shows infarcted tissue of the heart that develops after
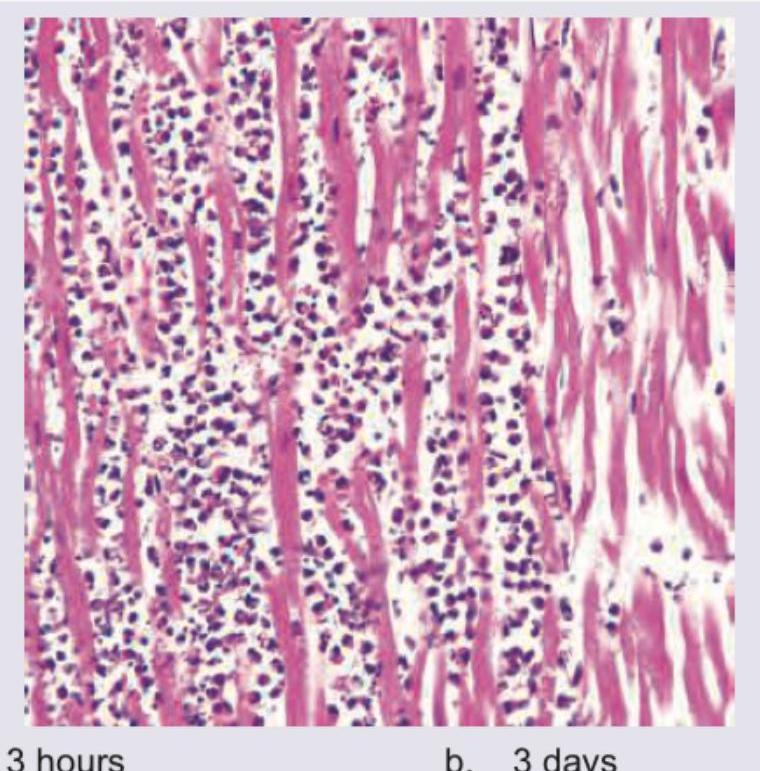
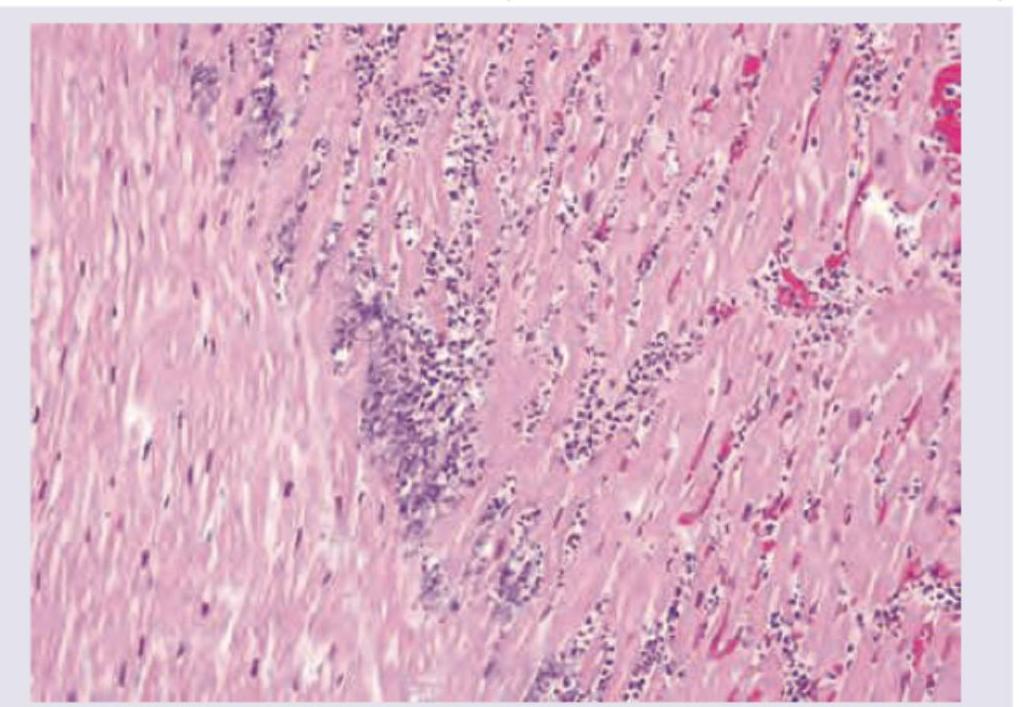
The following is the Hematoxylin and Eosin stained section from the heart of a patient after myocardial infarction. What can you say about the age of the infarction?
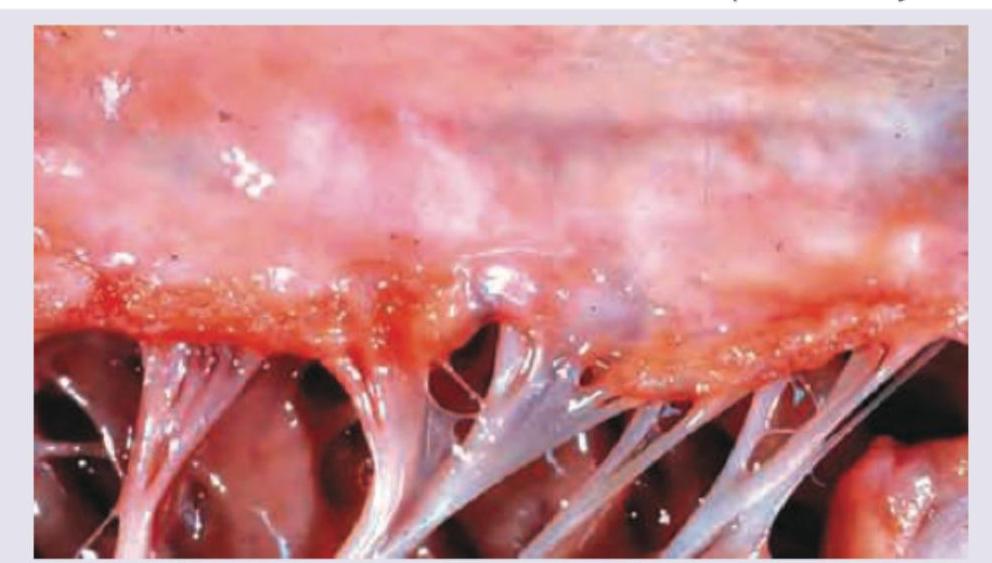
In a patient, Mitral valve vegetations are seen along the lines of closure along with fusion of commissures. What is the likely diagnosis?
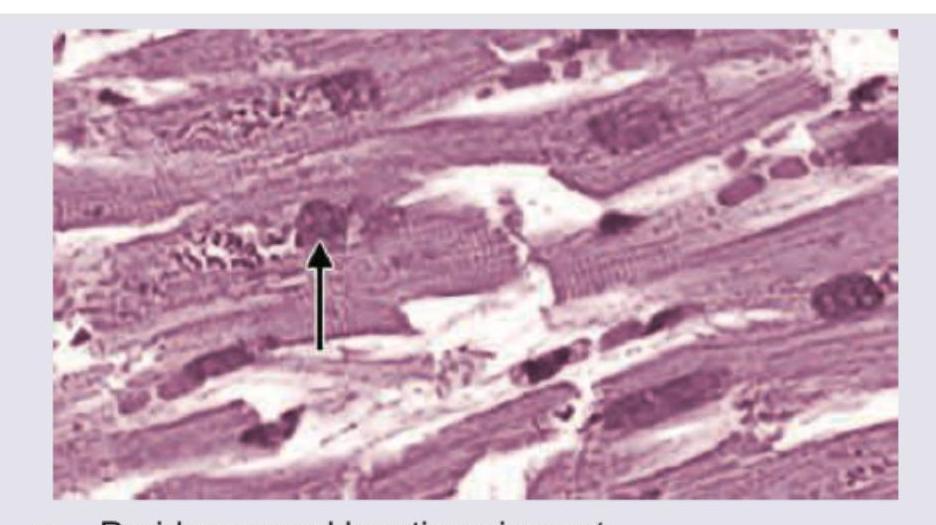
An 80-year-old Parkinsonism patient died due to pneumonia. All are true about the heart histopathology slide except:
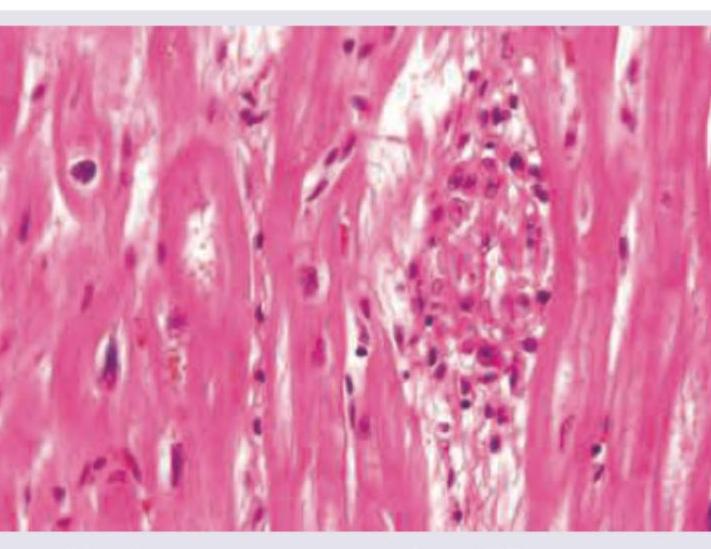
An 18-year-old male with severe effort intolerance and dyspnea is found to have left atrial enlargement on Chest X-ray. Histopathological examination shows:
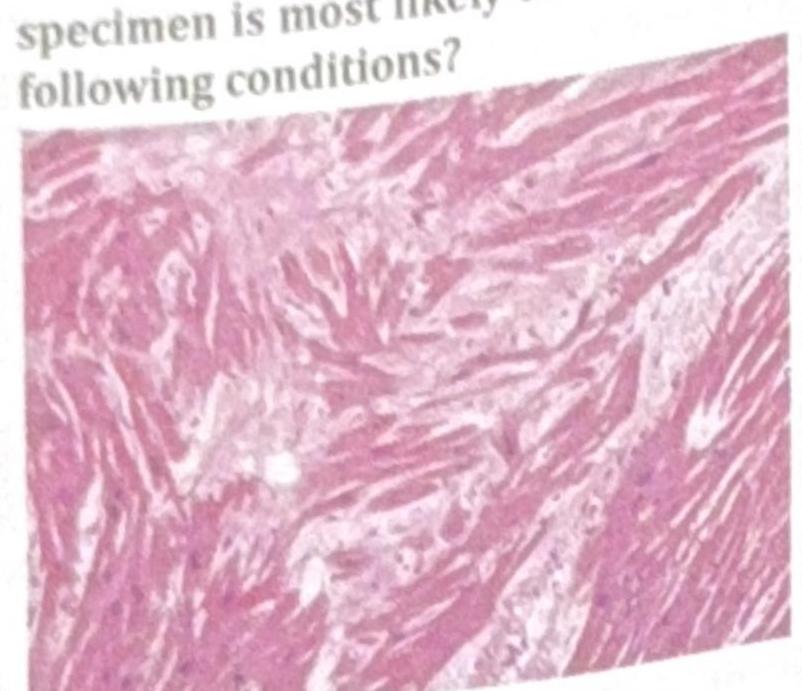
An athlete collapsed and expired while playing school basketball. Histology of the cardiac specimen is most likely to indicate which of the following conditions?
What is the histopathological finding 12 hours after ischemic injury to heart?
Which of the following has the most friable vegetations:
Practice by Chapter
Congenital Heart Disease
Practice Questions
Ischemic Heart Disease
Practice Questions
Hypertensive Heart Disease
Practice Questions
Valvular Heart Disease
Practice Questions
Myocarditis and Cardiomyopathies
Practice Questions
Pericardial Disease
Practice Questions
Cardiac Tumors
Practice Questions
Heart Failure Pathophysiology
Practice Questions
Cardiac Transplantation Pathology
Practice Questions
Endocarditis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
