Cardiac Pathology — MCQs

On this page
All of the following are seen in Coarctation of the Aorta, except?
Ground glass appearance of the ventricular septum is seen in which of the following conditions?
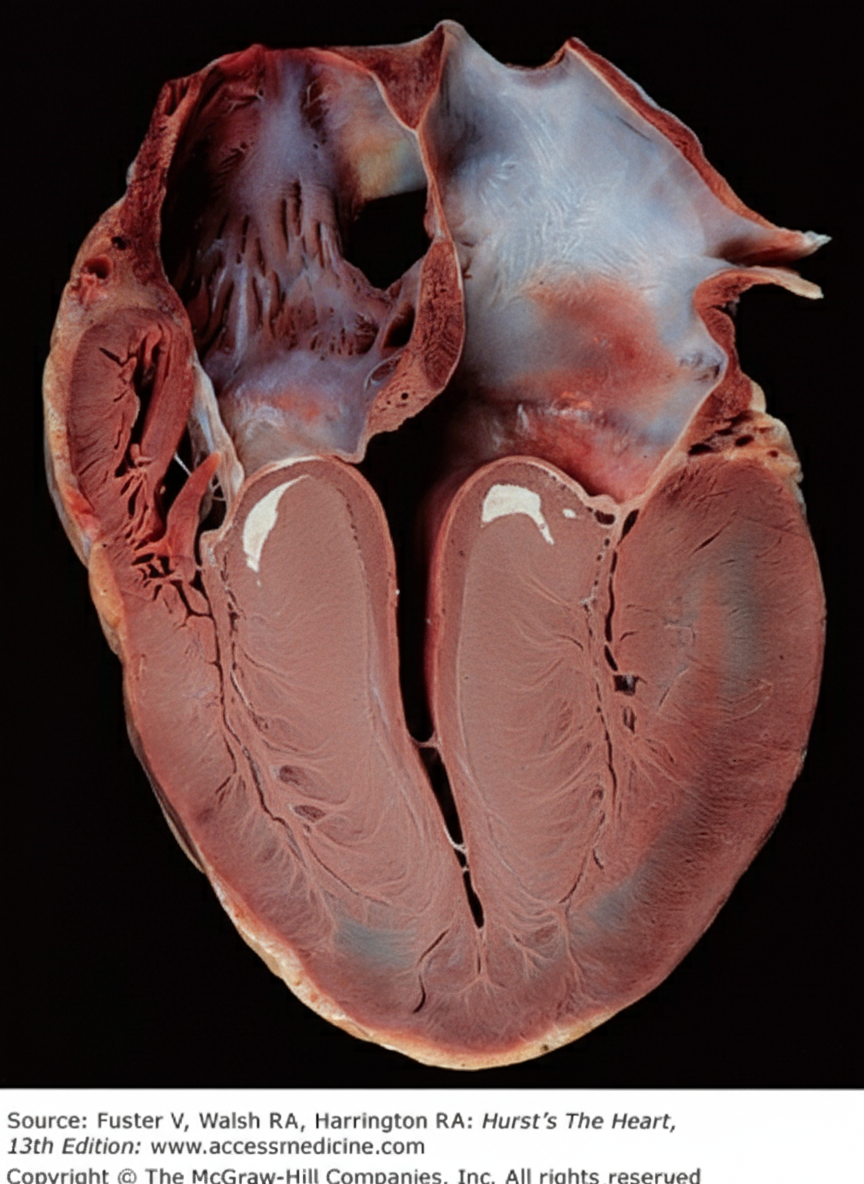
Which of the following statements is NOT true regarding the specimen shown?
Osler's nodes are seen in which of the following conditions?
Antischkow cells are seen in all conditions EXCEPT:
Which carcinoma metastasizes to the heart?
What type of exudate is characteristic of rheumatic fever?
A young female presents with verrucous vegetations on the surface of mitral valve cusps. What is the most likely diagnosis?
Aschoff's bodies are seen in which of the following conditions?
What are Aschoff cells?
Practice by Chapter
Congenital Heart Disease
Practice Questions
Ischemic Heart Disease
Practice Questions
Hypertensive Heart Disease
Practice Questions
Valvular Heart Disease
Practice Questions
Myocarditis and Cardiomyopathies
Practice Questions
Pericardial Disease
Practice Questions
Cardiac Tumors
Practice Questions
Heart Failure Pathophysiology
Practice Questions
Cardiac Transplantation Pathology
Practice Questions
Endocarditis
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
