Bone and Soft Tissue Pathology — MCQs

On this page
Keratocyst has all of the following features except?
Which of the following is characteristic of Osteogenesis imperfecta?
Which of the following has the strongest association with osteosarcoma?
An 8-year-old boy presents with progressive muscle weakness and walking difficulties. On examination, pseudohypertrophy of calf muscles was noted. Which of the following is true regarding this condition?
A patient presents with morning stiffness and tests positive for anti-CCP antibodies. Which of the following histological features is most characteristic of the underlying disease?
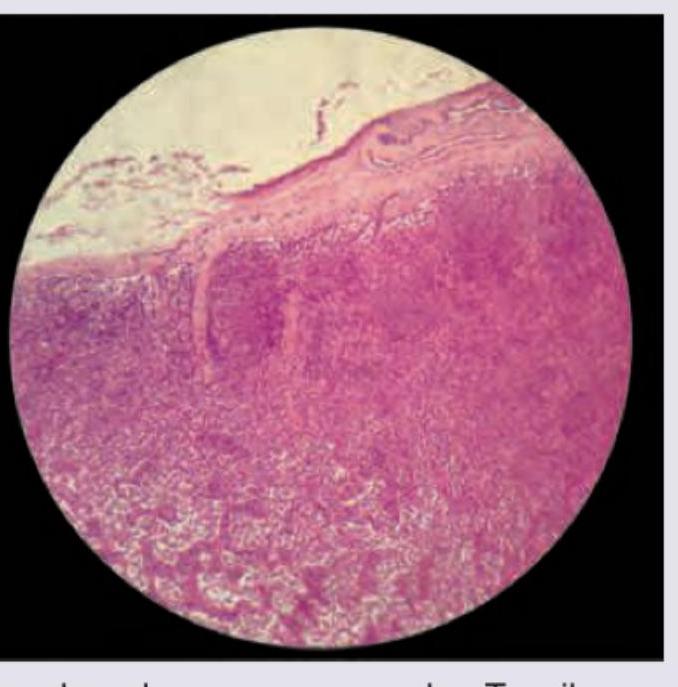
Identify the tissue
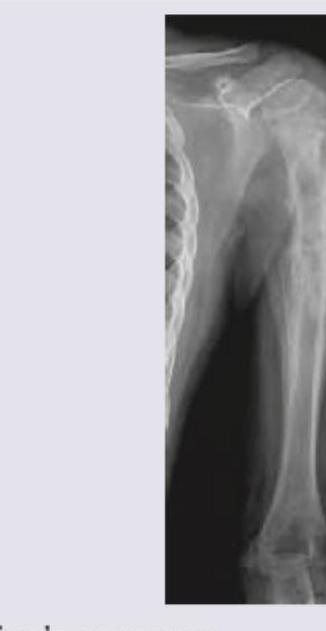
A 16-year-old boy presents with pain and swelling around the knee for 3 months. X-ray of the affected region is shown below. What is the most likely diagnosis?
Bone biopsy specimen is shown below. Diagnosis is:
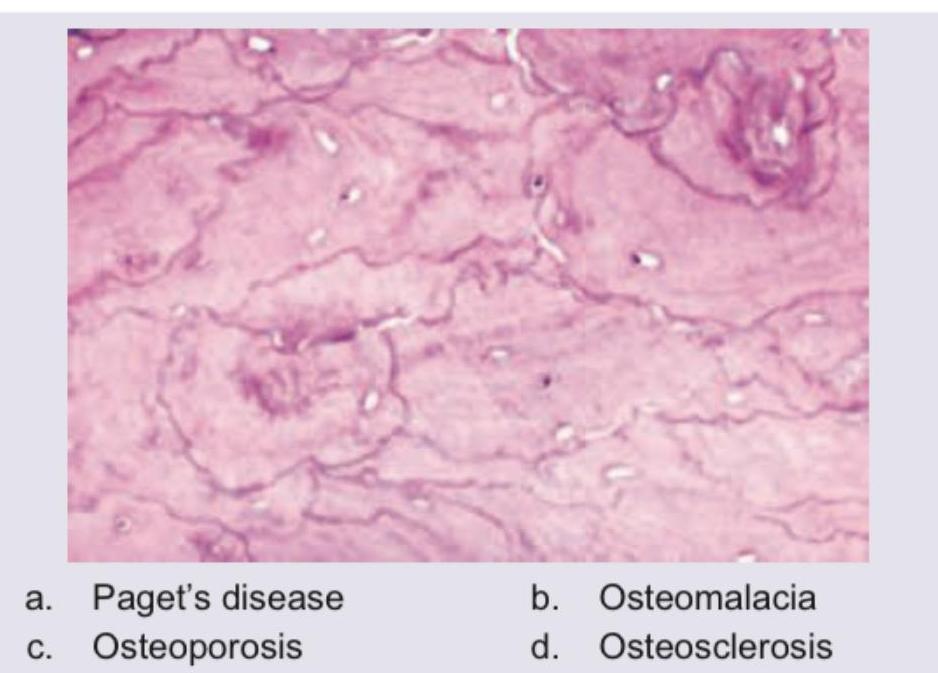
The most common site for osteosarcoma is:
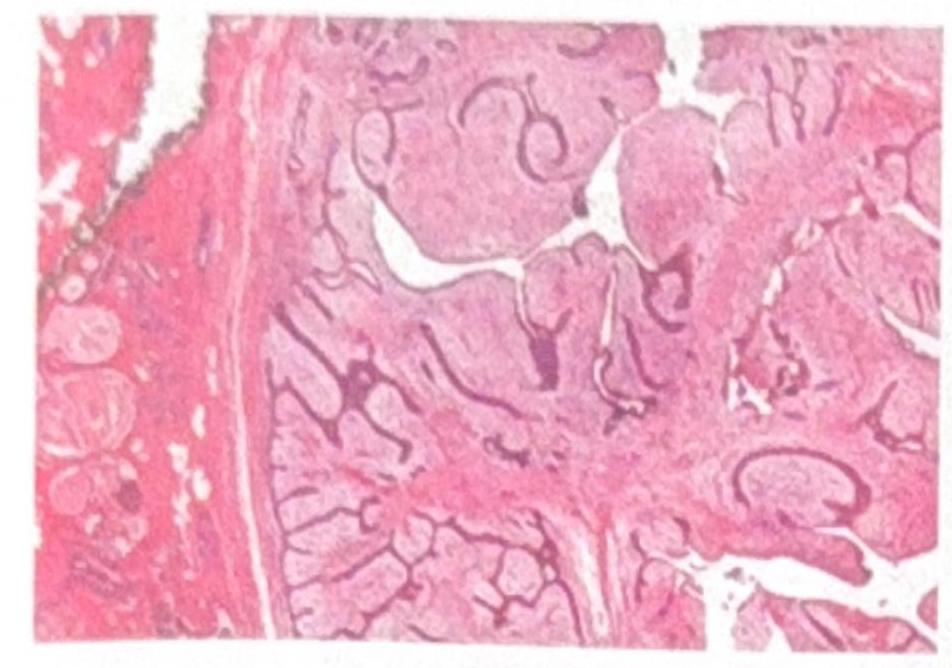
A 40-year-old female presents with an irregular 5 × 6 cm mass in the right breast. Histopathological examination reveals the image shown. What is the most likely diagnosis?
Practice by Chapter
Bone Development and Growth
Practice Questions
Fracture Healing
Practice Questions
Osteomyelitis and Infectious Diseases
Practice Questions
Metabolic Bone Diseases
Practice Questions
Bone Tumors and Tumor-like Lesions
Practice Questions
Joints and Rheumatologic Diseases
Practice Questions
Soft Tissue Tumors
Practice Questions
Muscular Dystrophies and Myopathies
Practice Questions
Diseases of Tendons and Fascia
Practice Questions
Pathology of Orthopedic Implants
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
