Metabolic Bone Diseases — MCQs

What is the gold standard for the diagnosis of osteoporosis?
Which vitamin deficiency is most commonly associated with rickets in children?
A child presents with rachitic changes in the limbs that are not responding to Vitamin D supplementation. Investigations reveal the following results: - Calcium: $9.5 \mathrm{mg} / \mathrm{dl}$ - Phosphorus: $1.6 \mathrm{mg} / \mathrm{dl}$ - Alkaline phosphatase (ALP): 814 IU - Serum PTH: $24.2 \mathrm{pg} / \mathrm{ml}$ - Serum electrolytes, creatinine, and blood gases: Normal. What is the most likely diagnosis?
The most important regulator of serum 1,25(OH)2 vitamin D concentration is:
A 70 year old male, known case of chronic renal failure suffers from a pathological fracture of Rt femur, the diagnosis is -
What type of lesions in the skull bones can be identified on this X-ray?
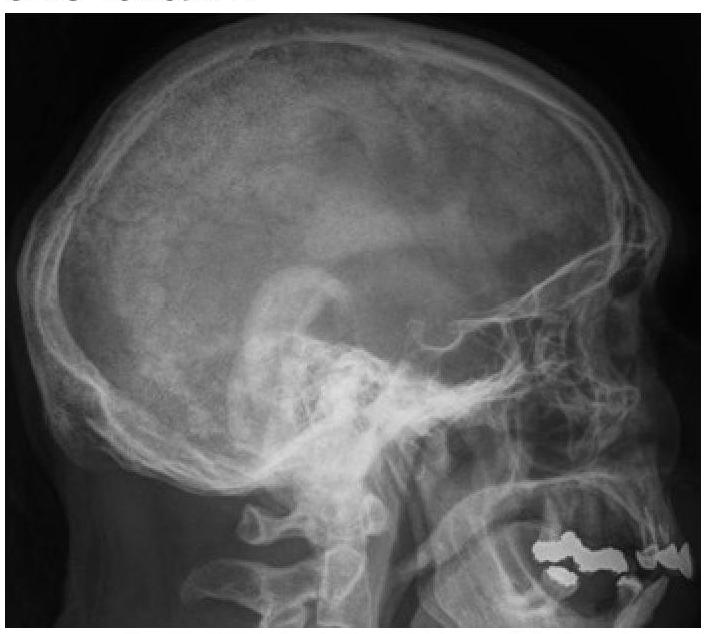
Select the type of bone disease which is most likely to be associated with genetically determined disorder in the structure or processing of type I collagen (SELECT 1 DISEASE)
All are causes of Osteoporosis, except:
Albers-Schönberg disease is:
Marble bone disease is:
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
