Bone Development and Growth — MCQs

10 questions
Read Study NotesQ1
Achondroplasia shows which type of inheritance?
Q2
Osteochondroma arises from which part of the bone?
Q3
Bone mass is reduced in all of the following conditions EXCEPT:
Q4
What is the primary organic component of bone?
Q5
Which bone tumor involves the epiphysis?
Q6
All of the following physiological processes occur during growth at the epiphyseal plate except:
Q7
Systemic factor which is responsible for bone remodeling :
Q8
All of the following produce osteoblastic secondaries except:
Q9
Inorganic component of bone is:
Q10
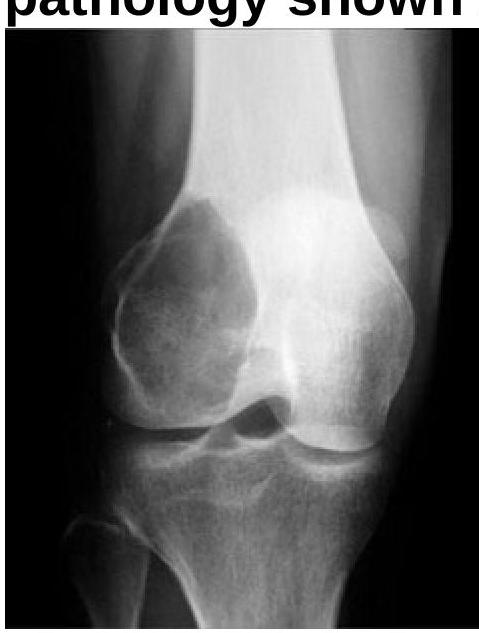
Which statement is incorrect about the pathology of the bone tumor?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
