Prosthetics and Orthotics — MCQs

On this page
The Milwaukee brace is used in the treatment of which of the following conditions?
Taylor's Brace is used for which of the following?
Which of the following is NOT true regarding the SACH Foot?
Who invented the Jaipur foot?
Which of the following statements is FALSE about the SACH Foot?
Which prosthesis is shown below in the X-ray?
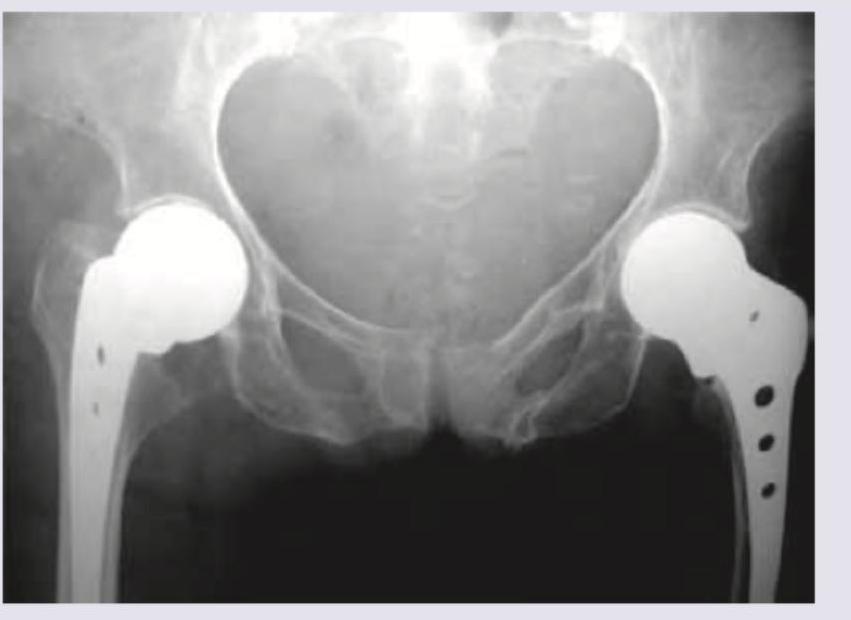
The shown apparatus is used for

All the following are advantages of the Jaipur foot over the conventional prosthetic foot except
Shortest functional level of trans tibial amputation is:
All of the following statements about SACH feet are true, except:
Practice by Chapter
Upper Limb Prosthetics
Practice Questions
Lower Limb Prosthetics
Practice Questions
Spinal Orthoses
Practice Questions
Upper Limb Orthoses
Practice Questions
Lower Limb Orthoses
Practice Questions
Assistive Devices for Mobility
Practice Questions
Prosthetic Fitting and Training
Practice Questions
Biomechanics of Prostheses
Practice Questions
Materials in Prosthetics and Orthotics
Practice Questions
Rehabilitation with Prostheses
Practice Questions
Modern Advances in Prosthetics
Practice Questions
Psychosocial Aspects
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
