Pediatric Orthopaedics — MCQs

On this page
An 8-year-old boy with a history of a fall from a 10-foot height complains of right ankle pain. Initial X-rays were normal and showed no fracture line. However, after 2 years, he developed a calcaneovalgus deformity. What is the most likely diagnosis?
What is the typical duration of delayed onset of muscle soreness (DOMS) in an 8-month-old child?
Sprengel's shoulder is a deformity of which bone?
All are true about Achondroplasia except?
What type of cast is typically used after closed reduction for a 4-month-old child diagnosed with developmental dysplasia of the hip (DDH)?
A child is spinned around by holding his hand by his father. While doing this, the child started crying and does not allow his father to touch his elbow. What is the most likely diagnosis?
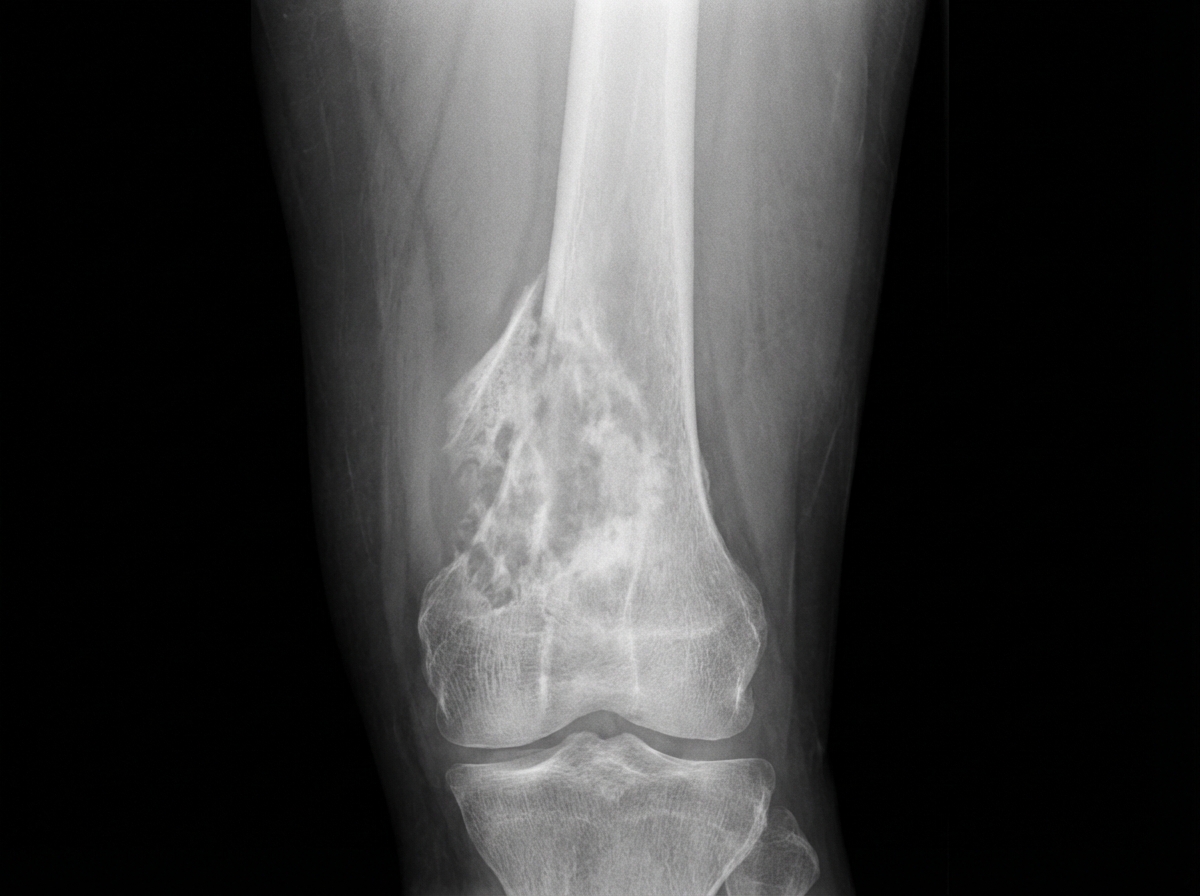
A 12-year-old boy presents with chronic knee pain for 2 years. The X-ray shows significant pathology. What is the probable diagnosis?
Congenital Pseudoarthrosis is:
Which of the following statements about Haglund's deformity is false?
Which of the following represents an appropriate management of Legg-Calve-Perthes disease in a young patient?
Practice by Chapter
Developmental Dysplasia of Hip
Practice Questions
Clubfoot
Practice Questions
Pediatric Fractures
Practice Questions
Growth Plate Injuries
Practice Questions
Legg-Calvé-Perthes Disease
Practice Questions
Slipped Capital Femoral Epiphysis
Practice Questions
Pediatric Spine Deformities
Practice Questions
Cerebral Palsy: Orthopaedic Aspects
Practice Questions
Neuromuscular Disorders in Children
Practice Questions
Pediatric Bone and Joint Infections
Practice Questions
Limb Length Discrepancies
Practice Questions
Orthopedic Manifestations of Genetic Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
