Pediatric Orthopaedics — MCQs

On this page
Which of the following movements is restricted in Perthes disease?
Which of the following sites is least commonly involved in arthrogryposis?
An afebrile, obese 14-year-old boy has developed pain at the right knee and a limp. What is the most likely diagnosis?
What is a greenstick fracture?
Von-Rosen's sign is positive in which condition?
Which of the following is true about developmental dysplasia of the hip (DDH)?
In a child with a cavovarus foot deformity, the standing lateral block test assesses the flexibility of which structure?
All of the following statements about Sprengel's deformity are false, except:
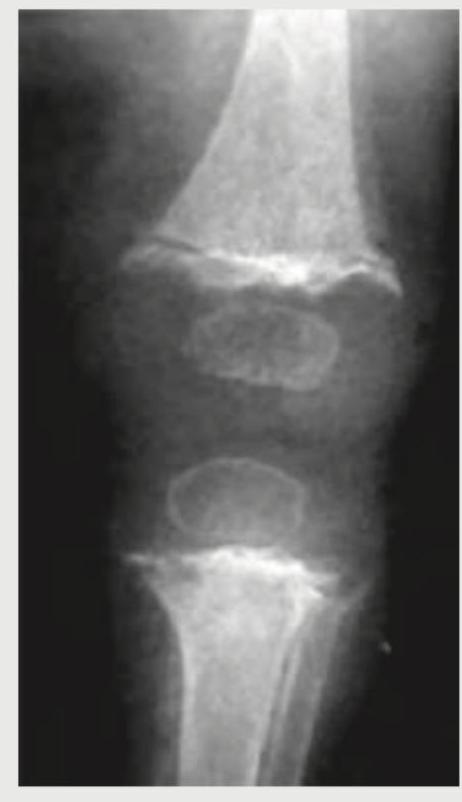
A 12-year-old boy presents with chronic knee pain for 2 years. A knee X-ray is shown. What is the probable diagnosis?
What is the best management for a fracture of the neck of the femur in a child?
Practice by Chapter
Developmental Dysplasia of Hip
Practice Questions
Clubfoot
Practice Questions
Pediatric Fractures
Practice Questions
Growth Plate Injuries
Practice Questions
Legg-Calvé-Perthes Disease
Practice Questions
Slipped Capital Femoral Epiphysis
Practice Questions
Pediatric Spine Deformities
Practice Questions
Cerebral Palsy: Orthopaedic Aspects
Practice Questions
Neuromuscular Disorders in Children
Practice Questions
Pediatric Bone and Joint Infections
Practice Questions
Limb Length Discrepancies
Practice Questions
Orthopedic Manifestations of Genetic Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
