Pediatric Orthopaedics — MCQs

On this page
What is the perichondrial ring?
Perthes disease is defined as:
A 3-year-old child presents with a complaint of limp. What is the most likely diagnosis?
What is the ideal age for performing a Posterior Malleolar Stress Test (PMSTR)?
The Ortolani test is considered positive when the examiner hears which of the following?
A 16-year-old obese female presents with a history of bilateral hip pain of long duration and a painful, limping gait. Endocrinology tests show hypothyroidism. Which of the following investigations is of no use in the diagnosis of this condition?
Which of the following conditions is managed with a Pavlik harness?
Congenital talipes equinovarus (CTEV) is caused by all of the following except?
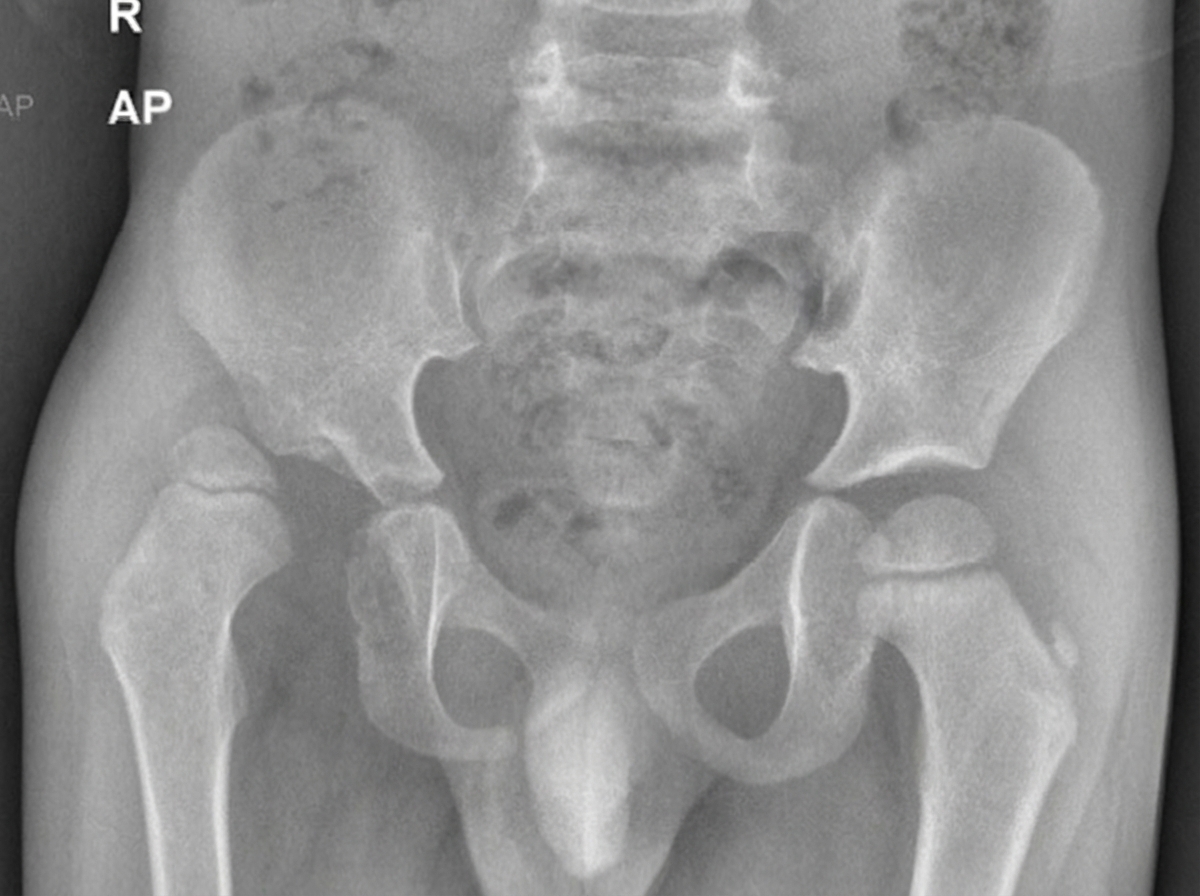
A child presents with hip pain. X-ray of the pelvis shows generalized osteopenia, thin cortices, gracile long bones, and proximal femoral deformity with evidence of healed fractures. What is the most likely clinical diagnosis?
Which joint is most commonly involved in Tom Smith arthritis?
Practice by Chapter
Developmental Dysplasia of Hip
Practice Questions
Clubfoot
Practice Questions
Pediatric Fractures
Practice Questions
Growth Plate Injuries
Practice Questions
Legg-Calvé-Perthes Disease
Practice Questions
Slipped Capital Femoral Epiphysis
Practice Questions
Pediatric Spine Deformities
Practice Questions
Cerebral Palsy: Orthopaedic Aspects
Practice Questions
Neuromuscular Disorders in Children
Practice Questions
Pediatric Bone and Joint Infections
Practice Questions
Limb Length Discrepancies
Practice Questions
Orthopedic Manifestations of Genetic Disorders
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
