Orthopedic Manifestations of Genetic Disorders — MCQs

In which condition is the presence of an extra pair of ribs sometimes observed?
Which of the following is least commonly associated with Down's syndrome?
A 10-year-old boy presents with frequent fractures and blue sclerae. This patient most likely carries a mutation in a gene that encodes which of the following proteins?
A 10-year-old girl presents with severe joint laxity, scoliosis, and a history of easy bruising. Which of the following conditions is most likely?
Mutations in type I collagen fibres results in:
An intrauterine scan at the 13th week of pregnancy showed a fetus with multiple long bone fractures. What is commonly associated with this finding?
The most commonly involved nerve in lunate dislocation is -
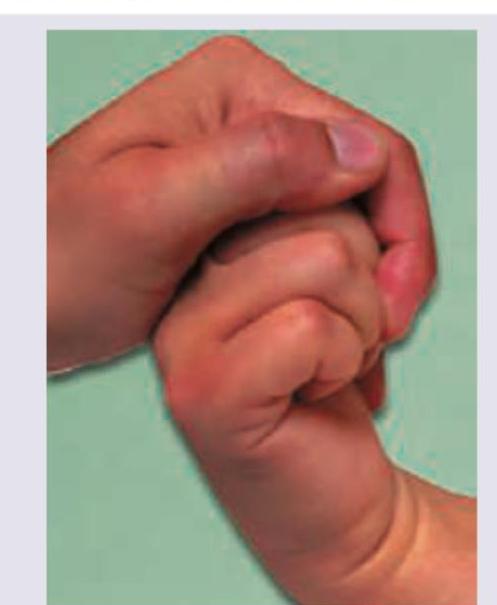
Identify the true statement regarding the clinical examination given in the image:
False about fracture of vertebrae
Slipped capital femoral epiphysis is seen most commonly in which age group?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
