Orthopedic Biomechanics — MCQs

On this page
When Class III elastics are used, what movement will the maxillary first molars exhibit?
A high crural index is typically observed in which of the following groups?
Which posture is associated with the greatest lumbar intradiscal pressure?
Which of the following muscles is primarily responsible for generating propulsive force during the push-off phase of normal gait?
What is the primary dynamic stabilizer of the patella against the lateral pull of the vastus lateralis?
What is the mechanical advantage obtained from the wheel and axle principle of an elevator?
In the mandibular symphysis region, which additional forces are present that are not usually seen in the body, ramus, or condylar regions?
The following gait is seen due to weakness of:
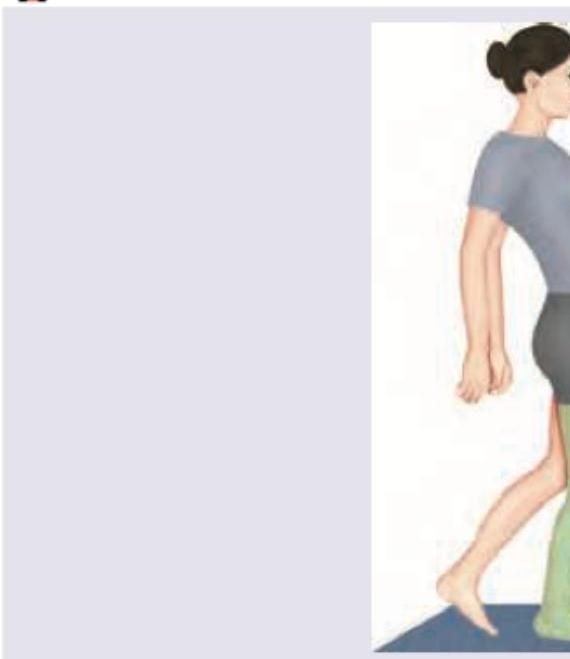
The following gait is due to weakness of:
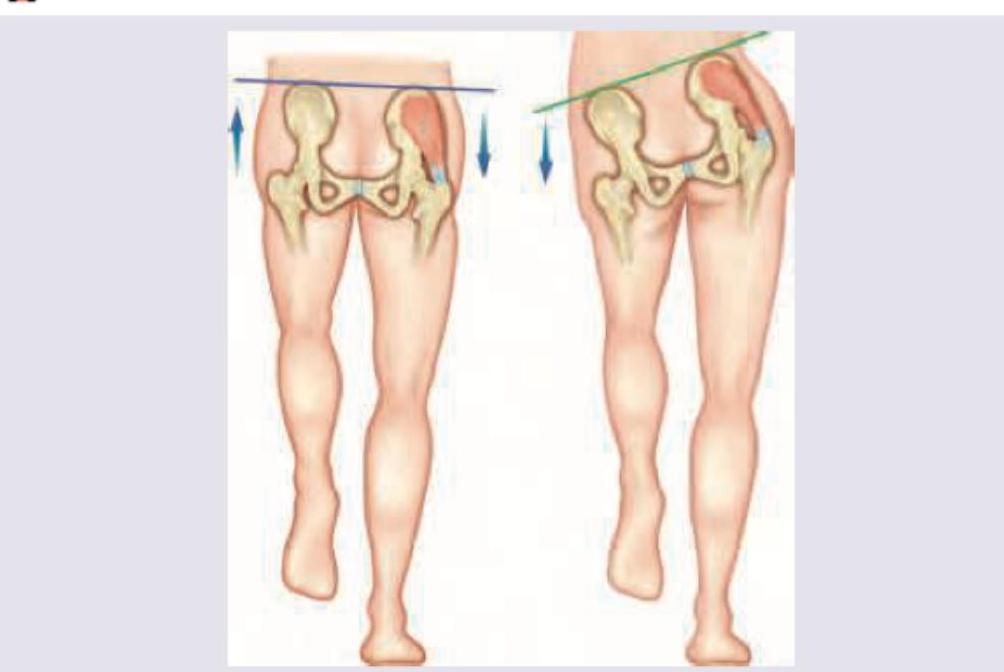
Defect in Gluteus Maximus lead to all of the following, EXCEPT:
Practice by Chapter
Principles of Biomechanics
Practice Questions
Biomechanics of Fracture Fixation
Practice Questions
Biomechanics of Spine
Practice Questions
Biomechanics of Hip
Practice Questions
Biomechanics of Knee
Practice Questions
Biomechanics of Foot and Ankle
Practice Questions
Biomechanics of Upper Limb
Practice Questions
Gait Analysis
Practice Questions
Biomechanics of Arthroplasty
Practice Questions
Biomechanics of Sports Injuries
Practice Questions
Computational Modeling in Orthopaedics
Practice Questions
Clinical Applications of Biomechanics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
