Orthopaedic Techniques — MCQs

On this page
Mc.Murray osteotomy is used in which of the following conditions?
Which type of distraction osteogenesis does not involve a transport disc?
What is the recommended pressure used in a pneumatic tourniquet for the upper limb?
Which of the following is NOT used for skeletal traction?
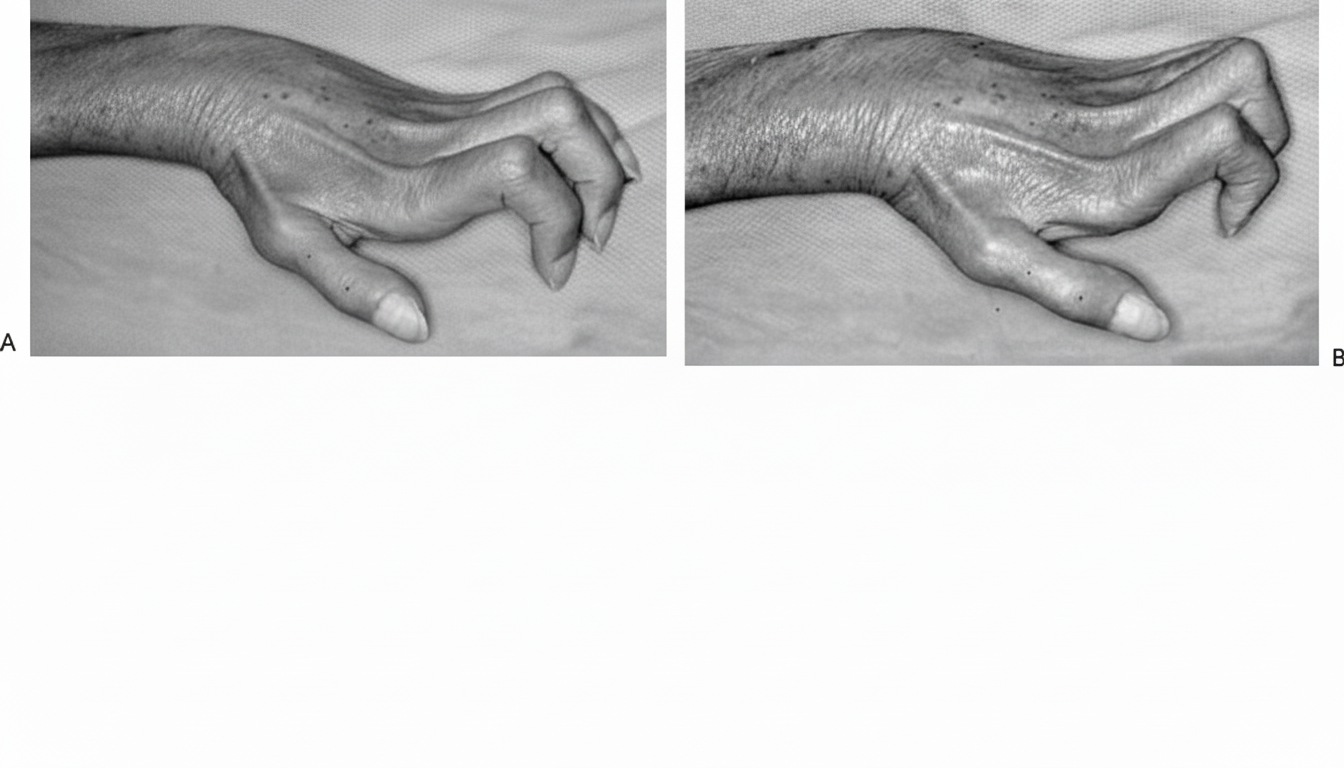
Which splint is used for the condition shown below?
Exsanguination is one of the first steps before the application of a tourniquet preoperatively. All of the following are contraindications for exsanguination EXCEPT:
What is the correct direction for the bevel of a chisel when cutting bone?
What is the rate of distraction beyond which soft tissue limits the distraction?
Osteotomes differ from chisels in that they are
All of the following are associated with tests or operations around the hip joint except?
Practice by Chapter
Principles of Internal Fixation
Practice Questions
External Fixation
Practice Questions
Intramedullary Nailing
Practice Questions
Plate Osteosynthesis
Practice Questions
Tension Band Wiring
Practice Questions
Minimally Invasive Orthopaedic Surgery
Practice Questions
Arthroscopic Techniques
Practice Questions
Suture Techniques in Orthopaedics
Practice Questions
Navigation and Robotics
Practice Questions
3D Printing Applications
Practice Questions
Bone Grafting Techniques
Practice Questions
Local Flaps and Soft Tissue Coverage
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
