Metabolic Bone Diseases — MCQs

On this page
Which disease is shown by the following X-ray of a foot?
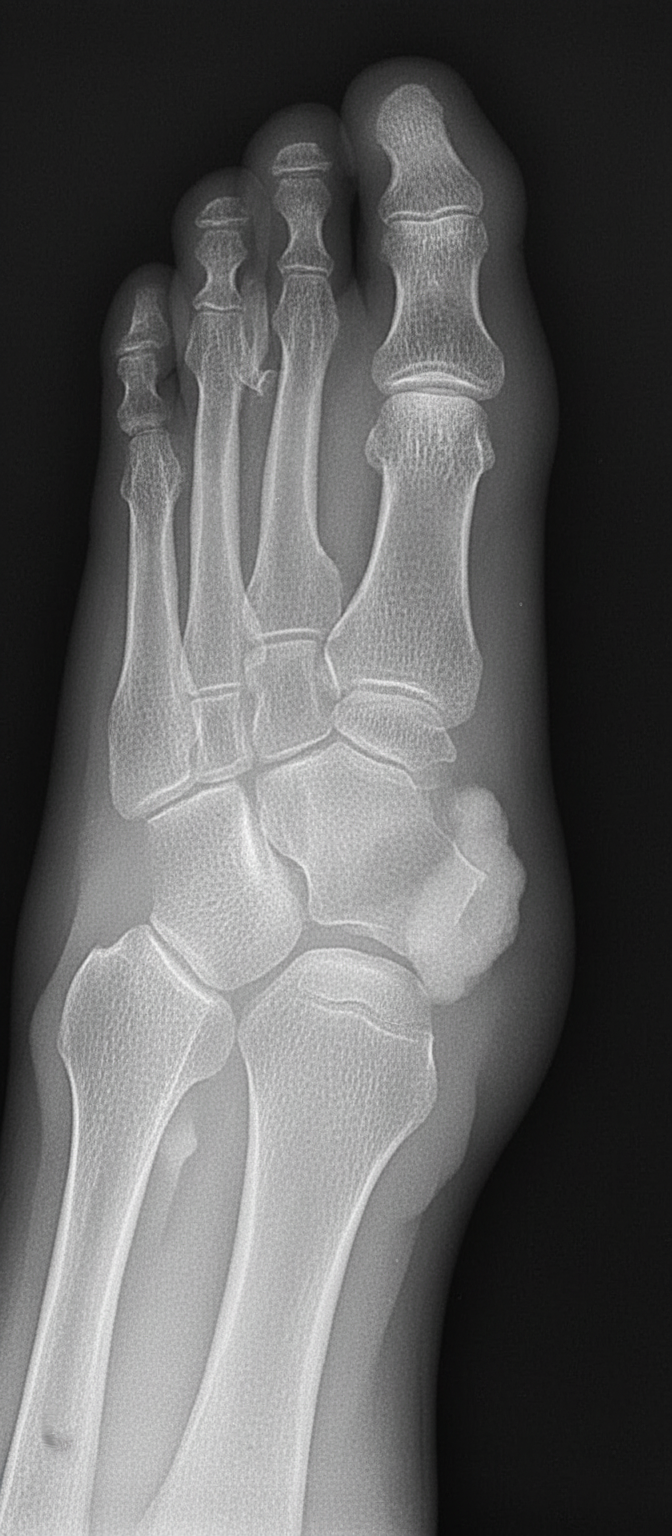
All are features of Jansen's disease, except?
Osteoporosis may be seen in all of the following conditions EXCEPT:
Which of the following carcinomas metastasizes to bone EXCEPT:
The most common manifestation of osteoporosis is:
Paget's disease is associated with which of the following?
Increased alkaline phosphatase is seen in which of the following conditions?
Windswept deformity in the foot is seen in which condition?
Wind swept deformity is seen in which condition?
In osteomalacia, all the following are seen except?
Practice by Chapter
Osteoporosis
Practice Questions
Osteomalacia and Rickets
Practice Questions
Paget's Disease of Bone
Practice Questions
Hyperparathyroidism
Practice Questions
Renal Osteodystrophy
Practice Questions
Fluorosis
Practice Questions
Osteogenesis Imperfecta
Practice Questions
Bone Mineral Density Assessment
Practice Questions
Pharmacological Management of Metabolic Bone Diseases
Practice Questions
Surgical Considerations in Metabolic Bone Diseases
Practice Questions
Fragility Fractures
Practice Questions
Prevention Strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
