Metabolic Bone Diseases — MCQs

On this page
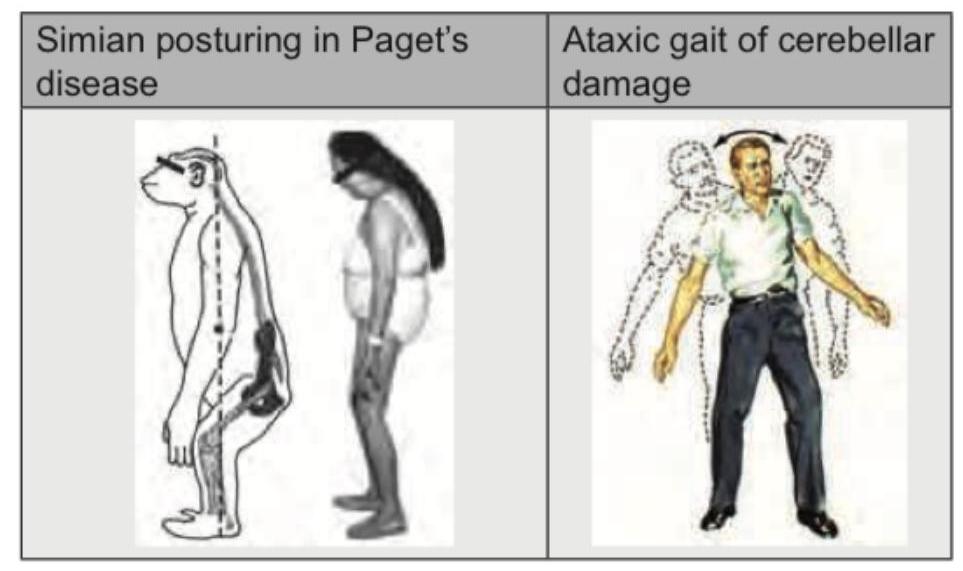
The appearance shown in the image is called as Simian Posturing. Notice the bent trunk, flexed legs and loss of spine normal axis. It occurs due to disordered bone turnover involving pelvis and vertebra. Which condition is most associated with this presentation?
A 60-year-old elderly female with a previous history of a Colles fracture is now complaining of backache. Which of the following statements regarding the treatment of this patient is incorrect?
Not seen in osteogenesis imperfecta
Albers Schonberg disease is also called as -
A 70-year-old female has been on alendronate for 7 years for osteoporosis and now complains of pain in her right thigh. What is the next investigation to be performed?
Wormian bones are seen in all except?
Brittle bone disease is -
A 45-year-old was given steroids after renal transplant. After 2 years he had difficulty in walking and pain in both hips. Which one of the following is most likely cause?
Avascular necrosis of head of femur occurs commonly at :
Avascular necrosis of bone is LEAST likely to be associated with?
Practice by Chapter
Osteoporosis
Practice Questions
Osteomalacia and Rickets
Practice Questions
Paget's Disease of Bone
Practice Questions
Hyperparathyroidism
Practice Questions
Renal Osteodystrophy
Practice Questions
Fluorosis
Practice Questions
Osteogenesis Imperfecta
Practice Questions
Bone Mineral Density Assessment
Practice Questions
Pharmacological Management of Metabolic Bone Diseases
Practice Questions
Surgical Considerations in Metabolic Bone Diseases
Practice Questions
Fragility Fractures
Practice Questions
Prevention Strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
