Metabolic Bone Diseases — MCQs

On this page
A 60-year-old person suffering from myositis ossificans progressive, what is the usual cause of death?
Nodular growth of alveolus is seen in which of the following?
Which bone is most commonly involved in Paget's disease?
Which of the following are characteristic features of childhood osteopetrosis?
An X-ray of a patient shows bulbous ends of long bones, normal appositional bone growth, and failure of physiologic root resorption. Laboratory findings show myelophthisic anemia. What is the probable diagnosis?
Absence of lamina dura in the alveolus occurs in which of the following conditions?
Rickets in an infant present with which of the following signs, except?
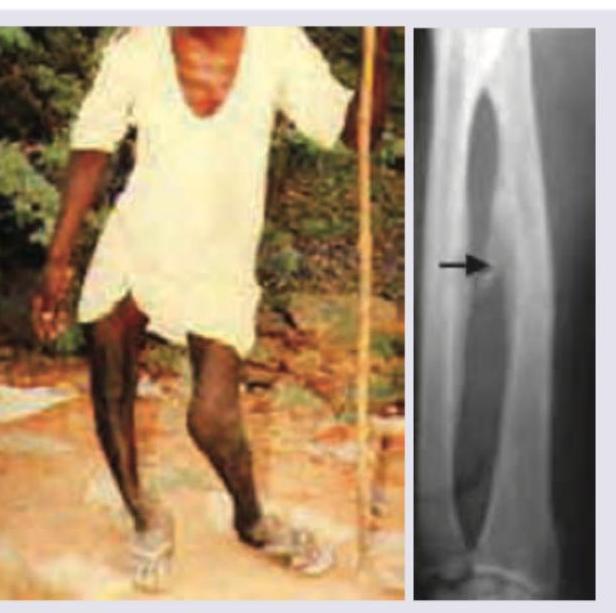
In a rural posting, a 35-year-old farmer comes to the OPD. Identify the condition shown:
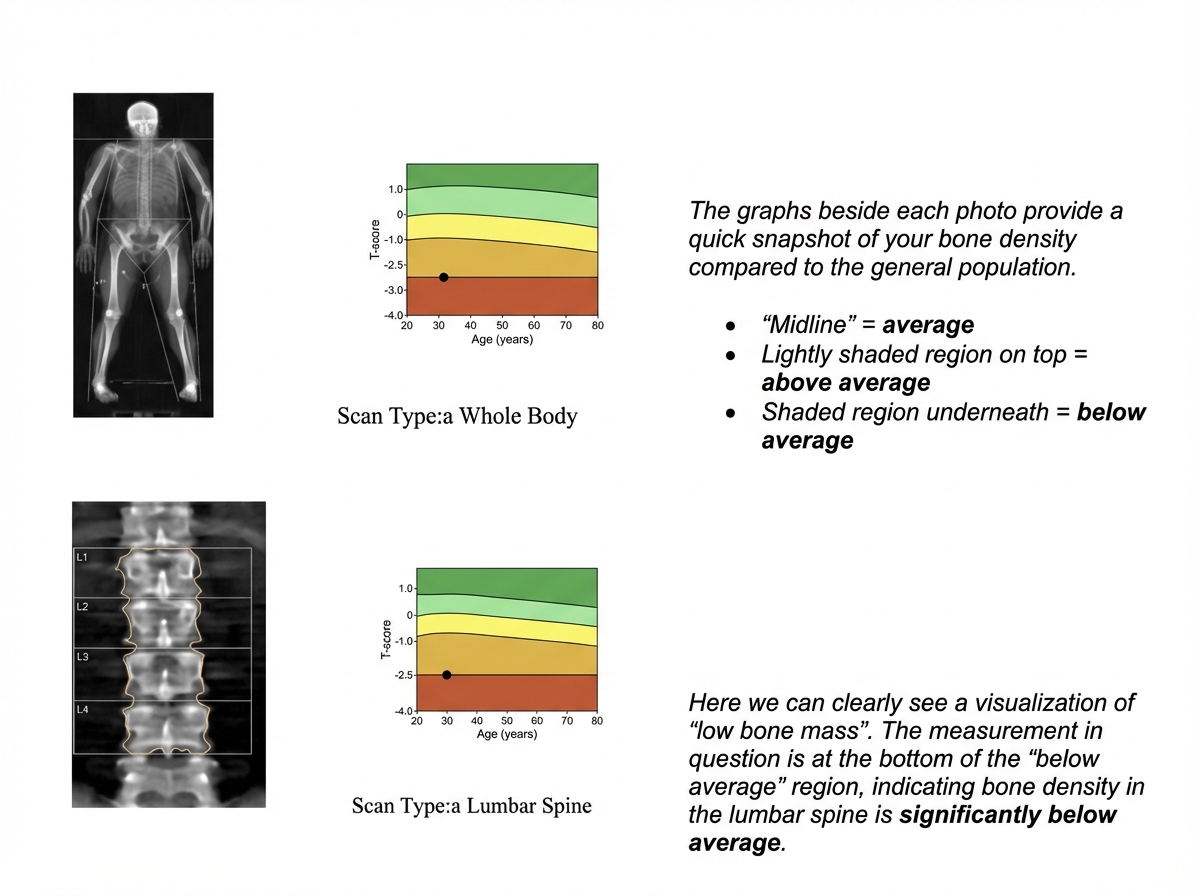
Which of the following is correct about the report of bone densitometry shown?
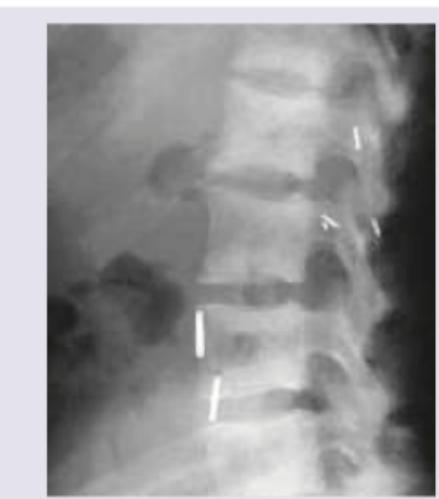
A 72-year-old woman presents with bone pain and tenderness in her lower extremities and left clavicle. Laboratory studies reveal elevated calcium, decreased phosphate, and elevated serum alkaline phosphatase. X-ray spine shows?
Practice by Chapter
Osteoporosis
Practice Questions
Osteomalacia and Rickets
Practice Questions
Paget's Disease of Bone
Practice Questions
Hyperparathyroidism
Practice Questions
Renal Osteodystrophy
Practice Questions
Fluorosis
Practice Questions
Osteogenesis Imperfecta
Practice Questions
Bone Mineral Density Assessment
Practice Questions
Pharmacological Management of Metabolic Bone Diseases
Practice Questions
Surgical Considerations in Metabolic Bone Diseases
Practice Questions
Fragility Fractures
Practice Questions
Prevention Strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
