Metabolic Bone Diseases — MCQs

On this page
Looser's zone occurs in all of the following conditions except?
In osteoporosis, what is observed?
Albers-Schonberg's disease is characterized by which of the following pathological conditions?
A 4-year-old child presents with blue sclera and a history of multiple fractures following minimal trauma. For the mentioned disorder, select the serum concentrations of calcium and phosphate with which it is most likely to be associated.
Albright syndrome includes which of the following combinations of features?
A 25-year-old female patient presented with anemia and seventh and eighth nerve palsy. Skull and spine X-rays revealed abnormalities consistent with a specific diagnosis. What is the diagnosis based on these findings?
What is true about Paget's disease?
Osteoporosis is caused by all of the following, except?
Blue sclera is a characteristic feature of which condition?
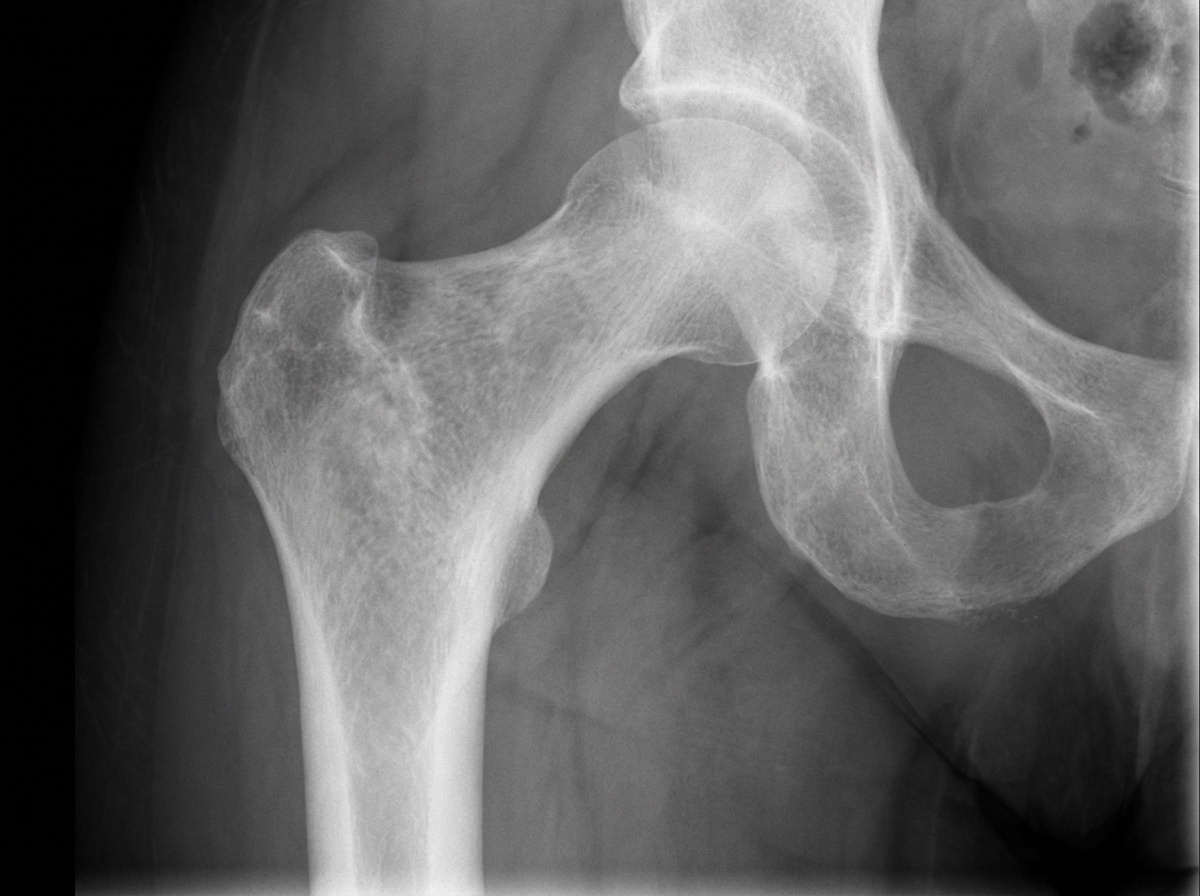
An X-ray of the proximal femur in a patient presenting with hip pain shows a specific deformity. What is this deformity?
Practice by Chapter
Osteoporosis
Practice Questions
Osteomalacia and Rickets
Practice Questions
Paget's Disease of Bone
Practice Questions
Hyperparathyroidism
Practice Questions
Renal Osteodystrophy
Practice Questions
Fluorosis
Practice Questions
Osteogenesis Imperfecta
Practice Questions
Bone Mineral Density Assessment
Practice Questions
Pharmacological Management of Metabolic Bone Diseases
Practice Questions
Surgical Considerations in Metabolic Bone Diseases
Practice Questions
Fragility Fractures
Practice Questions
Prevention Strategies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
