Hand Surgery — MCQs

On this page
Dupuytren's contracture commonly affects which finger?
Which of the following is NOT a cause of carpal tunnel syndrome?
An oblique view in an X-ray of the hand is required for the diagnosis of which carpal bone?
All of the following are true about Klumpke's paralysis except:
A patient experienced a fall onto an outstretched hand, and an X-ray revealed a fracture of the base of the first metacarpal with accompanying subluxation at the carpometacarpal (CMC) joint. Define this type of fracture.
Which nerve will be involved in the following finding at rest?
A labourer falls on an outstretched hand and complains of pain in the anatomical snuff box. Which of the following is the most appropriate next step?
What is Incorrect about the test being performed?
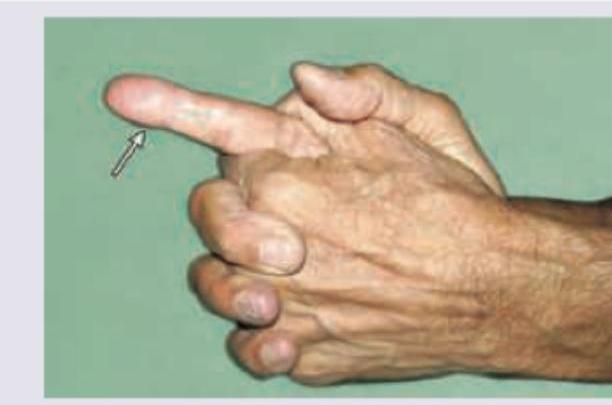
Identify the true statement regarding the clinical examination given in the image:
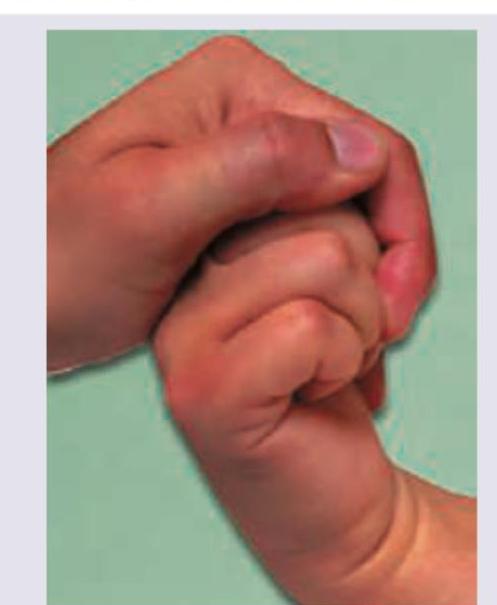
The following test is done to elicit:
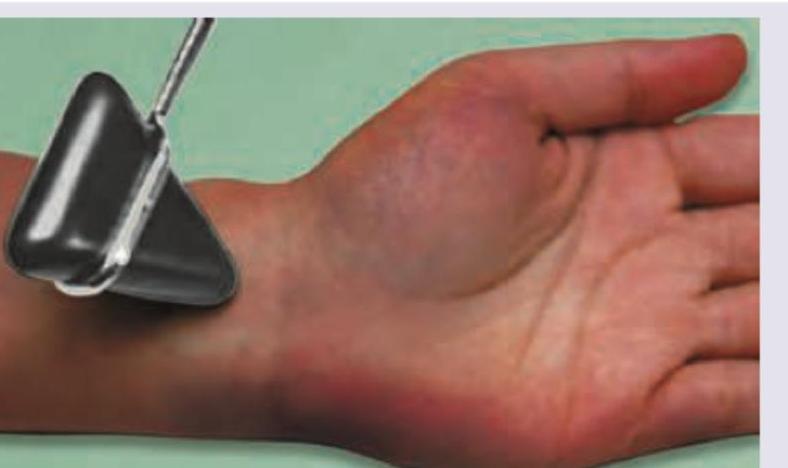
Practice by Chapter
Hand Anatomy and Biomechanics
Practice Questions
Hand Fractures and Dislocations
Practice Questions
Tendon Injuries
Practice Questions
Nerve Injuries in Hand
Practice Questions
Dupuytren's Disease
Practice Questions
Carpal Tunnel Syndrome
Practice Questions
Rheumatoid Hand
Practice Questions
Reconstructive Hand Surgery
Practice Questions
Tendon Transfers
Practice Questions
Congenital Hand Anomalies
Practice Questions
Hand Infections
Practice Questions
Microsurgery in Hand Surgery
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
