Foot and Ankle Surgery — MCQs

On this page
Which of the following is the commonest cause for neuralgic pain in the foot?
What are the radiographic findings in Freiberg disease?
All of the following are true regarding pes planus except:
A Patients presents with ankle pain and swelling after a forceful eversion injury. Based on the mechanism of injury, which ligament is most likely to be damaged?
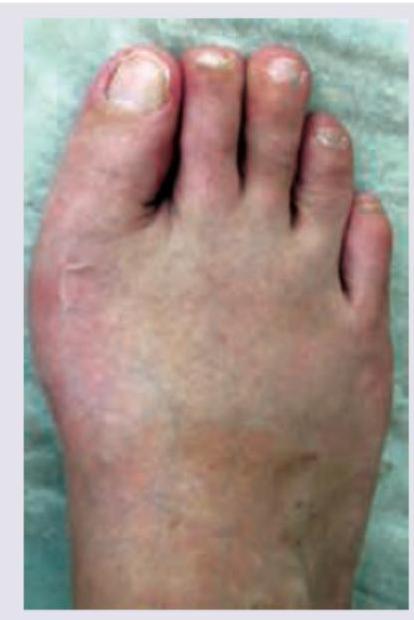
Identify the deformity seen in the given picture:
Which of the following statements regarding flat feet are true? 1. Nearly all children below 3 years have flat feet 2. 15% of adults have flat feet 3. Painless flexible flat feet need no treatment 4. Rigid flat feet result from tarsal coalition Select the correct answer using the code given below:
A patient presents with a 5th metatarsal fracture. How many days would he/she need to wear a cast?
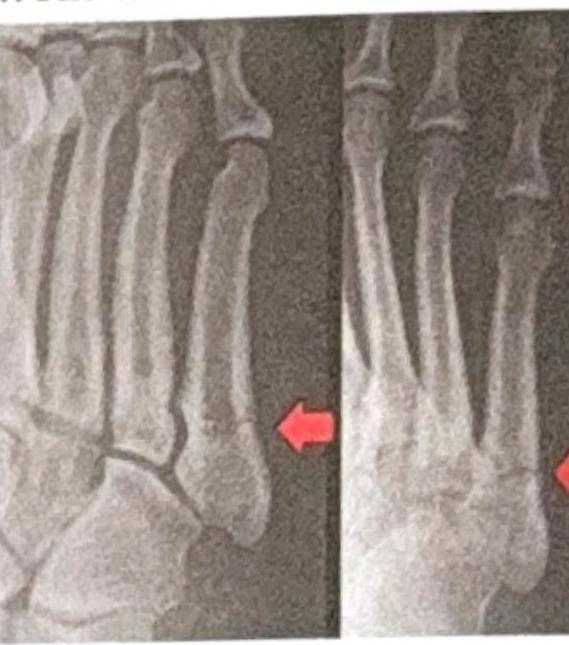
Bohler angle measurement gives the reference for ?
The primary site of pathology in ankle arthritis is the:
High stepping gait is due to
Practice by Chapter
Foot and Ankle Anatomy
Practice Questions
Hallux Valgus
Practice Questions
Flatfoot Deformities
Practice Questions
Cavus Foot
Practice Questions
Ankle Instability and Sprains
Practice Questions
Achilles Tendon Disorders
Practice Questions
Diabetic Foot
Practice Questions
Foot and Ankle Arthritis
Practice Questions
Ankle Fractures
Practice Questions
Foot Fractures
Practice Questions
Tendon Disorders of Foot and Ankle
Practice Questions
Reconstructive Procedures
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
